At his addiction clinic at Highland Hospital, a bustling public facility in the heart of Oakland, Herring promotes administering a shot of buprenorphine in the belly to provide a month of addiction treatment rather than prescribing oral versions that must be taken daily. For him, the shots’ longer-acting protection is a “game changer” and may be his only chance to help a vulnerable patient at risk of overdose.
“At any point in time, they’re just a balloon that’s going to go,” Herring said. “You might only have this one interaction. And the question is, how powerful can you make it?”
In California, , addiction experts say administering a month’s worth of anti-addiction medication holds great potential, particularly for people without housing or who struggle with other forms of instability. Yet despite its promise, the use of injectable buprenorphine remains fairly limited, especially compared with other forms of addiction medication. Researchers have yet to publish studies comparing different ways to administer buprenorphine.
Buprenorphine, one of three medications approved in the U.S. to treat opioid use disorder, works by binding to opioid receptors in the brain and reducing cravings and withdrawal symptoms. And because it occupies those receptor sites, buprenorphine keeps other opioids from binding and ensures that if a patient takes a high dose of a drug like heroin or fentanyl, they are less likely to overdose. Patients often stay on buprenorphine for years.

If Herring prescribes a supply of buprenorphine as a tablet or film that is placed under the tongue, the patient must commit to taking the medication at least once a day, and many fall out of treatment. He said this is especially true for his patients experiencing homelessness and those who also use methamphetamine.
“It’s like a religious thing ã you have to wake up every morning and repeat your vows,” said Herring. “In reality, there are a lot of people who deserve treatment who can’t meet that requirement.”
Oral forms of buprenorphine have been available to treat addiction since 2002 and can be purchased as a generic for . Injectable buprenorphine, sold under the brand name Sublocade, received FDA approval in 2017. It has a hefty list price of for a monthly injection. The drugmaker Indivior reported in revenue from Sublocade last year alone, with a company goal to eventually make $1 billion in annual sales. No generic or competing version of the drug is available.
Most patients won’t pay full price, Indivior says, because most health plans cover the drug. Physicians, however, say the high cost can be a barrier for patients with private health plans, which sometimes resist covering the medication. Medi-Cal, California’s health insurance program for low-income people, covers Sublocade without prior authorization, making the treatment accessible to the majority of Herring’s patients.
Still, addiction experts say, Sublocade use remains limited because of the regulatory hurdles required to dispense it.
Providers must register with the U.S. Drug Enforcement Administration and obtain a waiver to prescribe buprenorphine because it’s considered a controlled substance. In addition, clinics must complete an to dispense the medication. And Sublocade can be ordered only by a specialty pharmacy, which must also pass the FDA program.
“At many hospitals, that will mean either a delay in getting this medication on our shelves or just opting out,” said Dr. Rais Vohra, regional director for the , a state-funded program that supports hospitals in offering treatment for substance use disorders, including Herring’s clinic.
Vohra said Community Regional Medical Center in Fresno, where he works as an emergency physician, is still looking through the documentation requirements to see if the hospital’s pharmacy can distribute the medication ã which would make it one of the few Central Valley providers to do so.
Oral buprenorphine, by contrast, is a simple prescription that most local drugstores keep in stock.
“All the hoops that clinicians and patients have to jump through to get this medication is crazy. We don’t do that for any other disease,” said Dr. Hannah Snyder, who runs the addiction clinic at Zuckerberg San Francisco General Hospital across the bay.
Several clinicians noted that access remains a problem even with oral forms of buprenorphine. Despite a cascade of studies proving the effectiveness of medication-assisted treatment, many patients across the country struggle to find a provider willing to prescribe buprenorphine in any form ã especially in .
“The most important question isn’t whether long-acting injectable bupe is a better solution than sublingual buprenorphine for opioid use disorder,” said Dr. Michael Ostacher, a professor at Stanford University School of Medicine, who is comparing injectable and oral versions of buprenorphine through Veterans Affairs. “The bigger question is how we increase access to treatment for all people who need [the medication].”
Angela Griffiths is among the patients who say Sublocade has changed their lives. Griffiths, 41, of San Francisco, used heroin for 18 years. When she was pregnant with her daughter in 2016, doctors put her on methadone, which made her feel “miserable.” Three years ago, she said, she switched to buprenorphine films, but carrying the strips with her everywhere still made her feel tied to her addiction.
“The ritual of taking something every day plays something in your mind,” Griffiths said.
When doctors at the SF General clinic switched her to monthly Sublocade injections, she described the change as “extraordinary.”
“I’m not reaching for my drawer anymore for a fix,” she said. “I have the freedom to wake up and start my day however I want, whether it’s to go to the patio and drink a cup of coffee or to snuggle with my daughter in bed a little longer. It’s there; I don’t have to take anything.”

In states where Medicaid plans may still require prior authorization, waits for Sublocade can stretch into months. Across the border at the Northern Nevada Hopes clinic in Reno, Nevada, for example, Dr. Taylor Tomlinson said she tells patients that between battles for coverage and pharmacy delays, they might have to wait two months for an injection.
“I’m always going to offer it to a patient who I think would be a good candidate, but in the time they have to wait, they get interested in other things,” said Tomlinson. “It creates a barrier to care.”
California’s Medicaid program does not require prior authorization but providing Sublocade is still a challenge. At the Placerville clinic supported by the California Bridge Network, Dr. Juliet La Mers, the director, said a quarter of her buprenorphine patients get injections. Still, they often wait two weeks before Sublocade arrives from the specialty pharmacy.
Herring has been able to cut through some of that red tape at his Oakland clinic by working with the Highland pharmacy to stock and distribute Sublocade. As soon as a patient agrees to an injection, Herring simply calls the pharmacy down the hall and administers it on the spot.
Herring sees urgency ã and opportunity ã to increase the use of injectable buprenorphine as fentanyl use rises across California. For years, the deadly synthetic opioid was concentrated mostly on the East Coast; in 2018, from synthetic opioids occurred in the 28 states east of the Mississippi River. But more recently, fentanyl has begun to infiltrate Western states. From 2018 to 2020, deaths from fentanyl overdoses in California quintupled, .
“No one understands what they’re dealing with,” Herring said of fentanyl’s potency. “This is the time where our greatest deaths are going to occur.”
µÍºÇ¨û§ØŸl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/mental-health/monthly-injectable-opioid-addiction-treatment/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1488902&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>His mother, Brandie Kurtz, said his therapy wasn’t approved through Georgia’s Medicaid program until recently, despite her continued requests. “I know insurance, so it’s even more frustrating,” said Kurtz, who works in a doctor’s office near her home in rural Wrens, Georgia.
Those frustrations are all too familiar to parents who have a child with autism, a complex lifelong disorder. And the pandemic has exacerbated the already difficult process of getting services.
This comes as public awareness of autism and research on it have grown and insurance coverage for treatment is more widespread. In February, Texas became the last state to cover a widely used autism therapy through Medicaid. requiring private health plans to cover the therapy, .
Yet children from Georgia to California often wait months ã and in many cases more than a year ã to get a diagnosis and then receive specialized treatment services. Therapies that can cost $40,000 or more a year are especially out of reach for families who don’t have insurance or have high-deductible health plans. and may face additional barriers to getting help.
“You would never allow a kid with cancer to experience these waits,” said Dr. , a pediatrician at University of Missouri Health Care and chair of the American Academy of Pediatrics’ Autism Subcommittee.
During the early months of the covid-19 pandemic, many families canceled in-home services, fearing infection. Virtual therapy often didn’t seem to work, especially for nonverbal and younger children. With fewer clients, some providers laid off staff or shut down entirely.
And treatment services always face high turnover rates among the low-wage workers who do direct, in-home care for autism. But covid made the staffing problem worse. Companies now struggle to compete with rising wages in other sectors.
The Centers for Disease Control and Prevention estimates that , a higher prevalence rate than ever before. Autism symptoms can include communication difficulties and repetitive behaviors and can be accompanied by a range of developmental and psychiatric health conditions.
Early diagnosis of autism can make a difference, Sohl said. Symptoms of some kids who begin their therapy by age 2 or 3 can be .
Diagnoses are typically done by developmental-behavioral pediatricians, psychologists, psychiatrists, and neurologists, all of whom are in short supply. The shortage of developmental pediatricians is especially acute. Even though they do three more years of fellowship training than a general pediatrician does, developmental pediatricians typically earn less.
General pediatricians with training can also do assessments, but insurers often require a specialist’s diagnosis before paying for services, creating a bottleneck for families.
“If we solely rely on specialists, we’re setting ourselves up for failure because there aren’t enough of us. We need the insurance companies on board,” said Dr. , a pediatric neurologist and president of the Orange County, California, chapter of the American Academy of Pediatrics.
Even in a metro area, getting a child an appointment can take months. “We cannot get these families in fast enough,” said Dr. , a developmental pediatrician in suburban Atlanta. “It’s heartbreaking.”
Some parents pay cash for an evaluation with a private specialist, worsening disparities between kids whose parents can afford to skip the wait and those whose parents cannot.
Once a child has been diagnosed, many face an equal ã or longer ã wait to get autism therapies, including applied behavior analysis, a process that aims to improve social, communication, and learning skills. These sessions can take more than 20 hours a week and last more than a year. ABA techniques , but the American Academy of Pediatrics says that are based on ABA principles.
Accessing such treatment largely depends on insurance coverage ã and for many families how well Medicaid pays. The Georgia Medicaid program reimburses well for ABA, Georgia doctors said, while Missouri’s pay is low, leading to a scarcity of options there, Sohl said.
In California, Medicaid reimbursement rates vary by county, and wait times for ABA range from about three to 12 months. In the rural northern reaches of the state, where few providers work, some families wait years.

During the first year of the pandemic, Claire Hise of Orange County was thrilled with the ABA therapist who worked with her son. But in January 2021, the therapist quit to go back to school. The company she was working with sent others. Hise had to train each new therapist to work with her son, a difficult process that always took more than a month. “It’s a special relationship, and each kid with autism is an individual,” Hise said. “It takes time.”
By then, they were out the door, replaced by another after no more than four to six weeks. Sometimes the family waited weeks for a replacement.
Hise tried switching to another company, but they all had a six-month waitlist. “He’s already so far behind,” Hise said. “It’s really a year I feel we’ve lost.”
The in the U.S. is about 4 years old, but Black and Latino children on average .
“The impact on families having to wait for diagnosis or treatment can be devastating,” said Kristin Jacobson, founder of the Autism Deserves Equal Coverage Foundation, an advocacy group in California. “They know in their gut something is seriously not right and that there is help out there, and yet they are helpless to do anything about it.”
Araceli Barrientos helps run an autism support group in Atlanta for immigrant families, for whom language barriers can cause additional snags. It took her over a year to get her daughter, Lesly, diagnosed and two more years to secure further treatment.
Sabrina Oxford of Dawson, in rural southwestern Georgia, had to take her daughter Jamelyn more than 150 miles to the Marcus Autism Center in Atlanta to get her diagnosed. “You don’t have any resources around here,” Oxford said.
Dr. Michelle Zeanah, a behavioral pediatrician, draws families from 60 mostly rural counties to her clinic in Statesboro, Georgia. “There’s a massive shortage of people willing and able to do an autism diagnosis,” she said.
Getting insurance to pay for autism treatment can be another frustrating process for families. Therapy denials can be triggered by clerical errors or missed paperwork. Insurer approvals can be especially difficult for older children, who can be less likely to get treatment services than younger ones, said Dr. , a child and adolescent psychiatrist at Augusta University in Georgia.
Many children with autism also need speech, occupational, and physical therapy, all of which are generally easier to secure than behavioral therapy. But even then, Weintraub said, the insurers push back: “They really dictate how many services you can have. These families, literally, meet obstacles at every turn.”
David Allen, a spokesperson for AHIP, an insurance industry trade group formerly known as America’s Health Insurance Plans, said insurers often require prior authorization to ensure that autism services are “medically necessary and evidence-based” and that patients are treated by “providers with appropriate education and training in treating autism.”
Tracy-Ann Samuels of New York said she paid out-of-pocket for speech and occupational therapy for her son, Trey, now 15. Two years ago, after 18 months on a waiting list, he finally got ABA services covered by insurance.
“He’s doing so great,” she said. “My son was nonverbal. Now he’s talking my ear off.”
µÍºÇ¨û§ØŸl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/delays-for-autism-diagnosis-and-treatment-grew-even-longer-during-the-pandemic/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1467973&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Over the years, Lockwood, a nurse midwife who runs a group for new moms from her home in Oakland, California, experimented with a gamut of approaches to bedtime. When Rex was a baby, she let him “cry it out” so he could learn to put himself back to sleep. As he got older, she would lie beside him for hours each night. Finally, she hired a sleep consultant who created yet another plan that didn’t solve the problem. By the time Rex was 3, Lockwood, with another baby on the way, was worn out and desperate.
Then she read about melatonin, a hormone released by the human pineal gland that helps regulate the sleep cycle. Melatonin is sold as a dietary supplement at pharmacies across the U.S. and marketed for kids in the form of chewable tablets, flavored liquids, and gummies. “I thought maybe he just needed a reset,” said Lockwood.
From the very first night, said Lockwood, “it was like a whole different kid.” She gave him a melatonin tablet and read him a story, and he fell asleep almost immediately. “Our plan was to use melatonin for two weeks and stop.”
Six years later, he still takes it every night.
Throughout history, parents have searched for the secret to a smoother bedtime: sleeping together, sleeping apart, the war of wills, offering stuffies and pacifiers and warm milk, even spending $1,600 on a “smart” bassinet that responds to a baby’s cries with white noise and motion.
In recent years, melatonin supplements have become an increasingly common child sleep aid that in the U.S. requires no prescription and is only lightly regulated by the FDA.
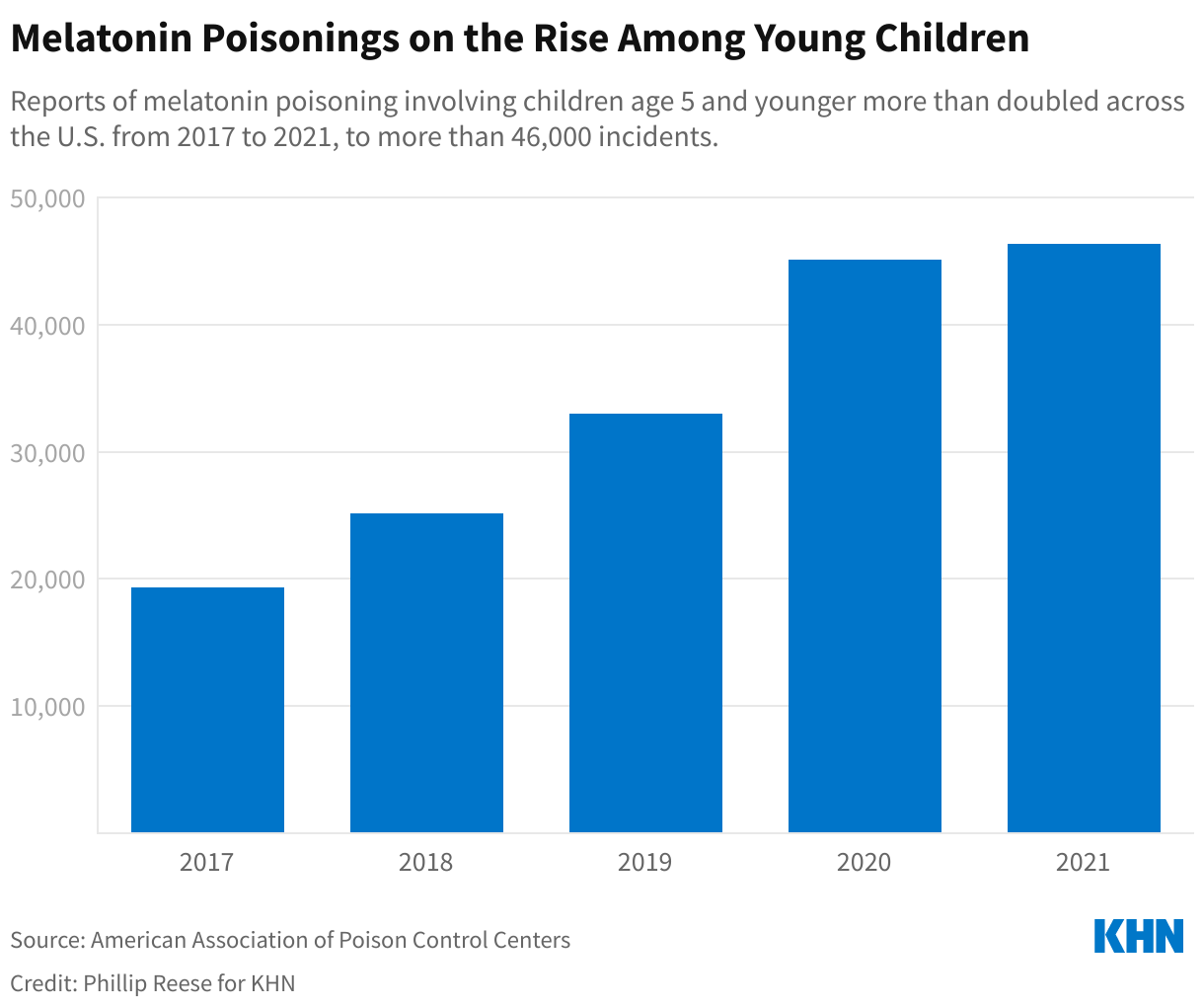
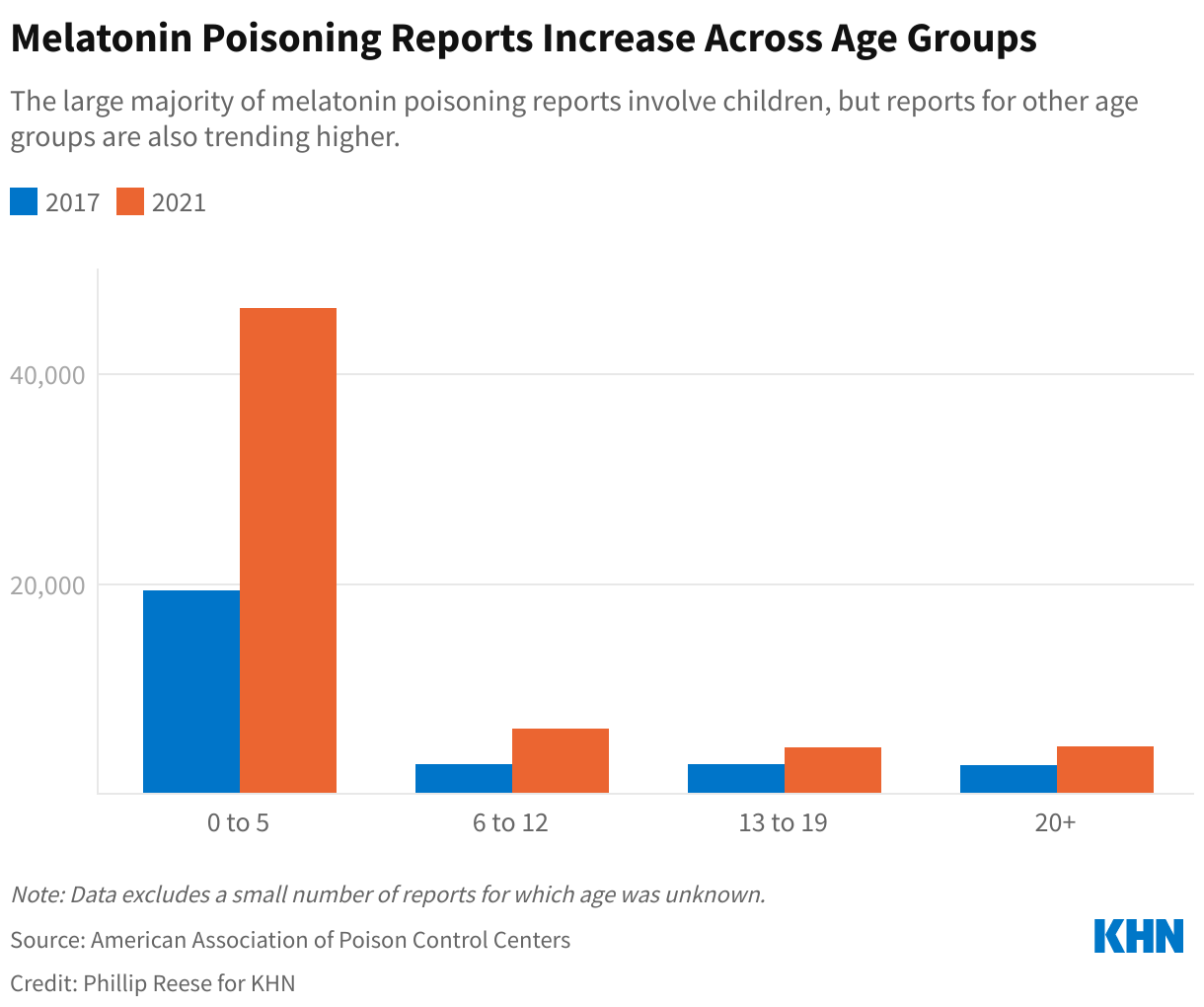
In 2021, Americans spent $1.09 billion overall on melatonin supplements, a nearly 150% increase over 2018 sales, according to data provided by NielsenIQ. Meanwhile, the number of reports of melatonin poisoning involving young children — meaning they ingested excessive dosages — more than doubled from 2017 through 2021, according to the American Association of Poison Control Centers. There were about 46,300 melatonin poisoning reports involving children age 5 and under in 2021, up from nearly 19,400 in 2017. Potential symptoms of an overdose include headaches, dizziness, and irritability. Only a handful of the reported incidents led to major medical issues.
“It speaks to the ubiquitousness of melatonin. It’s trickled down to younger and younger children,” said Dr. Judith Owens, co-director of the sleep center at Boston Children’s Hospital and a professor of neurology at Harvard Medical School. “What I find particularly alarming is that pediatricians are recommending this as a quick fix. It gives parents and then older kids the message that if you can’t sleep, you need to take a pill.”
The American Academy of Sleep Medicine the use of melatonin for chronic insomnia in both adults and children and will soon release a health advisory stating that melatonin should not be used in children without a physician’s supervision, said Dr. Muhammad Adeel Rishi, co-chair of the group’s public safety committee and a sleep specialist at Indiana University.
“More often than not insomnia in children is a behavioral problem, and it’s related to their bedtime routine, access to electronics at bedtime, and other activities they engage with other than sleeping,” said Rishi. “Often you can treat it without medication, with behavioral interventions.”
Rishi attributes the recent increase in children’s use of melatonin in part to marketing efforts by supplement manufacturers, including products like gummies targeted specifically to children. But he also believes the pandemic has spawned a “growing epidemic of insomnia.”
“We’ve been going through a very stressful time as a society. It’s available over the counter, so there’s easy access. Parents are often taking it themselves. And it’s supposedly safe,” said Rishi. “It’s kind of a perfect storm.”
For all the concern expressed about melatonin, it also has staunch defenders among sleep specialists and pediatricians, creating a confusing mixed message for parents seeking a fix for their sleep-deprived households.
Dr. Rafael Pelayo, a professor in the division of sleep medicine at Stanford Medicine, said he considers melatonin a useful tool for treating sleep disorders in children. “It’s simply telling the brain that night is approaching,” he said. “I think the real problem isn’t that it’s being overused. It’s how prevalent sleep problems are for kids.”
“A small improvement in the child’s sleep,” he added, “can have a dramatic impact on the family.”
Pelayo said he sometimes recommends melatonin for children while the family also implements behavioral changes to address an underlying issue. Many kids manage without it after they learn the skill of sleeping on their own, he said, but some do end up taking it long term. He said it works best for children who have trouble falling asleep, rather than those who wake frequently through the night.
Melatonin is a heated topic of conversation in Facebook groups like , of which Jill Kunishima is a member. Kunishima first tried melatonin for her son at the suggestion of their pediatrician. He had been a good sleeper until he went to preschool at age 3. The school’s late naptime disrupted his schedule, and he was staying up until nearly 10 p.m.
“The next day he was a mess. We’d go into his room in the morning, and he was all crotchety,” said Kunishima, who lives in Oakland.
The pediatrician recommended a 1-milligram melatonin tablet for a week or two, and her son’s bedtime went back to 8:30 p.m. “It got his body to calm down,” she said. “It was just what he needed.” But when she tried to wean him, she said, the problem started again.
When Kunishima went in for her son’s next medical visit, the pediatrician said not to worry. “‘If that’s the thing that’s going to keep your life just a little bit sane during this moment, just go ahead,’” she recalled the doctor telling her. “But now he’s 6, in first grade, and he’s still using it.”
Studies suggest that melatonin appears to be safe for short-term use in children, but there is little information on the long-term effects, . Because melatonin is a hormone, some experts worry its use could delay puberty, though the evidence is scarce. Other possible side effects include drowsiness, bed-wetting, and agitation.
Because melatonin is treated as a supplement in the U.S. — as opposed to a drug — the quality and dosage levels can vary widely. that tested 31 melatonin supplements found the actual melatonin levels ranged from less than a fifth to nearly five times the dosage listed on their labels. One in 4 of the products tested also contained serotonin, a hormone that can have serious side effects even at low doses.
Owens said she worries about the teenagers and young adults who have been on melatonin for a decade or more, the effects of which are still unknown. “Whenever you recommend or prescribe a sleep medication, you have to have an exit strategy. What is your benchmark for saying we’re going to stop this medication now?” she said. “I have patients who ask for their sleep pill every night, and that sends chills up my spine.”
She also worries that the American Academy of Pediatrics has not released official guidelines on the use of melatonin in children, given pediatricians frequently recommend melatonin as a sleep aid and in ever-younger patients — sometimes starting at 6 months old.
Lockwood said her now-9-year-old son still takes about a quarter of a milligram of melatonin every night before bed. It’s such a small dose that she wonders if perhaps he might be experiencing a placebo effect, but efforts to wean him revive his insomnia.
At Lockwood’s new moms group in Oakland, sleep is often the main topic of conversation. “It’s just this thing that consumes us as parents,” she said. “For me, it was that no one was helping me and no one had the answer.”
“Sometimes I wonder if he’s going to have to keep doing this for his whole life,” she added. “But I don’t beat myself up anymore. It works, and he’s happy.”
Phillip Reese, an assistant professor of journalism at California State University-Sacramento, contributed to this article.
µÍºÇ¨û§ØŸl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/melatonin-children-gummies-bedtime-struggles-caution/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1468010&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>In a matter of days, Lags Medical, a sprawling network of privately owned pain clinics serving more than 20,000 patients throughout the state’s Central Valley and Central Coast, would shut its doors. Its patients, most of them working-class people reliant on government-funded insurance, were left without ready access to their medical records or handoffs to other physicians. Many patients were dependent on opioids to manage the pain caused by a debilitating disease or injury, according to that state health officials emailed to area physicians. They were sent off with one final 30-day prescription, and no clear path for how to handle the agony ã whether from their underlying conditions or the physical dependency that accompanies long-term use of painkillers ã once that prescription ran out.
The closures came on the same day that the California Department of Health Care Services suspended state Medi-Cal reimbursements to 17 of Lags Medical’s 28 locations, citing without detail “potential harm to patients” and an ongoing investigation by the state Department of Justice into “credible allegations of fraud.” In the months since, the state has declined to elaborate on the concerns that prompted its investigation. Patients are still in the dark about what happened with their care and to their bodies.
Even as the government remains largely silent about its investigation, interviews with former Lags Medical patients and employees, as well as KHN analyses of reams of Medicare and Medi-Cal billing data and other court and government documents, suggest the clinics operated based on a markedly high-volume and unorthodox approach to pain management. This includes regularly performing skin biopsies that industry experts describe as out of the norm for pain specialists, as well as notably high rates of other sometimes painful procedures, including nerve ablations and high-end urine tests that screen for an extensive list of drugs.
Those procedures generated millions of dollars in insurer payments in recent years for Lags Medical Centers, an affiliated network of clinics under the ownership of Dr. Francis P. Lagattuta. The clinics’ patients primarily were insured by Medicare, the federally funded program for seniors and people with disabilities, or Medi-Cal, California’s Medicaid program for low-income residents.
Taken individually, the fees for each procedure are not eye-popping. But when performed at high volume, they add up to millions of dollars.
Take, for example, the punch biopsy, a medical procedure in which a circular blade is used to extract a sample of deep skin tissue the size of a pencil eraser. The technique is commonly used in dermatology to diagnose skin cancer but has limited use in pain management medicine, usually involving a referral to a neurologist, according to multiple experts interviewed. These experts said it would be unusual to use the procedure as part of routine pain management.
In Lagattuta’s specialty ã physical medicine and rehabilitation, a common pain management field ã just six of the nearly 8,000 U.S. physicians treating Medicare patients billed for punch biopsies on more than 10 patients in 2019, the most recent year for which data was available. Four, including Lagattuta, were affiliated with Lags Medical.
Medicare and Medi-Cal data are organized differently, and each provides distinct insights into Lags Medical’s billing practices. For Medicare, KHN’s findings reflect the number of procedures and actual reimbursements billed through Lagattuta’s provider number. But the Medicare figures do not encompass services and billing amounts for other providers across the chain, nor reimbursements for patients enrolled in private Medicare Advantage plans.
KHN used Medi-Cal records to assess the volume of services performed across the entire chain. But the state could not provide totals for how much Lags Medical was reimbursed because of California’s extensive use of managed-care plans, which do not make their reimbursement rates public. Where possible, KHN estimated the worth of Medi-Cal procedures based on the set rates Medi-Cal pays traditional fee-for-service plans, which are public.
Lags Medical clinics performed more than 22,000 punch biopsies on Medi-Cal patients from 2016 through 2019, according to state data. Medi-Cal reimbursement rates for punch biopsies changed over time. In 2019 the state’s reimbursement rate was more than $200 for a set of three biopsies performed on patients in fee-for-service plans.
Laboratory analysis of punch biopsies was worth far more. Lags Medical clinics sent biopsies to a Lags-affiliated lab co-located at a clinic in Santa Maria, according to medical records and employee interviews. From 2016 through 2019, Lags Medical clinics and providers performed tens of thousands of pathology services associated with the preparation and examination of tissue samples from Medi-Cal patients, according to state records. The services would have been worth an estimated $3.9 million using Medi-Cal’s average fee-for-service rates during that period.
In that same period, Medicare reimbursed Lagattuta at least $5.7 million for pathology activities using those same billing codes, federal data shows.
Much of the work at Lags Medical was performed by a relatively small number of nurse practitioners and physician assistants, each juggling dozens of patients a day with sporadic, often remote supervision by the medical doctors affiliated with the clinics, according to interviews with former employees. Lagattuta himself lived in Florida for more than a year while serving as medical director, according to testimony he provided as part of an ongoing malpractice lawsuit that names Lagattuta, Lags Medical, and a former employee as defendants.
Former employees said they were given bonuses if they treated more than 32 patients in a day, a strategy Lagattuta confirmed in his deposition in the malpractice lawsuit. “If they saw over, like, 32 patients, they would get, like, $10 a patient,” Lagattuta testified.
The lawsuit, filed in Fresno County Superior Court, accuses a Lags Medical provider in Fresno of puncturing a patient’s lung during a botched injection for back pain. Lagattuta and the other named defendants have denied the incident was due to negligent treatment, saying, in part, the patient consented to the procedure knowing it carried risks.

Hector Sanchez, the nurse practitioner who performed the injection and is named in the lawsuit, testified in his own deposition that providers at the Lags Medical clinic in Fresno each treated from 30 to 40 patients on a typical workday.
According to Sanchez’s testimony and interviews with two additional former employees, Lags Medical clinics also offered financial bonuses to encourage providers to perform certain medical procedures, including punch biopsies and various injections. “We were incentivized initially to do these things with cash bonuses,” said one former employee, who asked not to be named for fear of retribution. “There was a lot of pressure to get those done, to talk patients into getting these done.”
In his own deposition in the Fresno case, Lagattuta denied paying bonuses for specific medical procedures.
Interviews with 17 former patients revealed common observations at Lags Medical clinics, such as crowded waiting rooms and an assembly-line environment. Many reported feeling pressure to consent to injections and other procedures or risk having their opioid supplies cut off.
Audrey Audelo Ramirez said she had worried for years that the care she was receiving at a Lags Medical clinic in Fresno was subpar. In the past couple of years, she said, there were sometimes so many patients waiting that the line wrapped around the building.
Ramirez, 52, suffers from trigeminal neuralgia, a rare nerve disease that sends shocks of pain across the face so severe it’s known as the “suicide disease.” Over the years, Lags Medical had taken over prescribing almost all her medications. This included not only the opioids and gabapentin she relies on to endure excruciating pain, but also drugs to treat depression, anxiety, and sleep issues.
Ramirez said she often felt pressured to get procedures she didn’t want. “They were always just pushing injections, injections, injections,” she said. She said staffers performed painful punch biopsies on her that resulted in an additional diagnosis of small fiber neuropathy, a nerve disorder that can cause stabbing pain.
She was among numerous patients who said they felt they needed to undergo the recommended procedures if they wanted continued prescriptions for their pain medications. “If you refuse any treatment they say they’re going to give you, you’re considered noncompliant and they stop your medication,” Ramirez said.
She said she eventually agreed to an injection in her face, which she said was administered without adequate sedation. “It was horrible, horrible,” she said. Still, she said, she kept going to the office because there weren’t many other options in her town.
Lagattuta, through his lawyer, declined a request from KHN to respond to questions about the care provided at his clinics, citing the state investigation. “Since there is an active investigation, Dr. Lagattuta cannot comment on it until it is completed,” attorney Matthew Brinegar wrote in an email. Lagattuta’s license remains in good standing, and he said in his deposition in the Fresno lawsuit that he is still seeing patients in California.
Experts interviewed by KHN noted that medical procedures such as injections can have a legitimate role in comprehensive pain management. But they also spoke in general terms about the emergence of a troubling pattern at U.S. pain clinics involving the overuse of procedures. In the 1990s and early 2000s, problematic pain clinics hooked patients on opioids, then demanded cash to continue prescriptions, said Dr. Theodore Parran, who is a professor of medicine at Case Western Reserve University and has served as an expert witness in federal investigations into pain clinics.
“What has replaced them are troubled pain clinics that hook patients with the meds and accept insurance, but overuse procedures which really pay well,” he said. For patients, he added, the consequences are not benign.
“I mean they are painful,” he said. “You’re putting needles into people.”

ãKnee Injections, Hip Injections, Foot Injections’
Before moving to California in 1998, Dr. Francis Lagattuta lived in Illinois and worked as a team doctor for the Chicago Bulls during its 1995-96 championship season. Out West, he opened a clinic in Santa Maria, a Latino-majority city along California’s Central Coast known for its strawberry fields, vineyards, and barbecue. From 2015 to 2020, the chain grew from a couple of clinics in Santa Barbara County to dozens throughout California, largely in rural areas, as well as far-flung locations in Washington state, Delaware, and Florida.
The California portion of the chain is organized as more than two dozen corporations and limited liability corporations owned by Lagattuta. His son, Francis P. Lagattuta II, was a manager for the company.
On the Lags Medical website and in conversation with employees, the elder Lagattuta claimed he was of diagnosing and treating small fiber neuropathy. Much of the website has now . But pages available via an archival site claim he had pioneered to pain management that made minimal use of opioids and surgeries, instead emphasizing testing, injections, mental health, diet, and exercise. “In keeping with his social justice values, Dr. Lagattuta plans to share these findings to the rest of the world, hopefully to help solve the opioid crisis, and end suffering for millions of people struggling with pain,” once highlighted on the website.
Numerous Lags Medical patients interviewed by KHN said that even when they were given punch biopsies and a subsequent diagnosis of neuropathy, their treatment plan continued to involve high doses of opioid medications.
Dr. Victor C. Wang, chief of the division of pain neurology at Brigham and Women’s Hospital in Boston, said punch biopsies are occasionally used in research but are not a standard part of pain medicine. Instead, small fiber neuropathy is usually diagnosed with a simple clinical exam.
“The treatment is going to be the same whether you have a biopsy or not,” said Wang. “I always tell the fellows, you can do this test or that one, but is it really going to change the management of the patient?”
Ruby Avila, a mother of three in Visalia, remembers having the punch biopsies done at least three times during her four years as a Lags Medical patient. “I have scars down my leg,” she said. Each time, she said, providers removed a set of three skin specimens that were used to diagnose her with small fiber neuropathy.
Avila, 37, who has lived with pain since childhood, had found it validating to finally have a diagnosis. But after learning more about how common the biopsies were at Lags Medical, she was shaken. “It’s overwhelming to hear that they were doing it on a lot of people,” she said.
Sanchez, the nurse practitioner named in the Fresno lawsuit, spoke of other procedures that garnered bonuses: “Trigger point injections, knee injections, hip injections, foot injections for plantar fasciitis and elbow injections” all qualified for $10 bonuses, he said in his testimony.
Two former employees, who asked not to be named, echoed Sanchez, saying they were incentivized to do certain procedures, including injections and punch biopsies.
In his testimony in the Fresno case, Lagattuta denied paying bonuses for procedures. “It was only for the patients,” he said. “We never did it based on procedures.”
Incentive systems for a specific procedure are “completely unethical,” said Dr. Michael Barnett, an assistant professor of health policy at Harvard. “It’s like giving police officers a quota for speeding tickets. What do you think they’re going to do? I can’t think of any justification.”

Dr. Carl Johnson, 77, is a pathologist who directed Lags Medical’s Santa Maria lab from 2018 to 2021. Johnson said the only specimens he looked at came from punch biopsies, the first time in his long career as a pathologist that he had been asked to run such an analysis. On an average day, he said, he examined the slides of about 40 patients, searching for signs of small fiber neuropathy. Lagattuta gave him papers to read on peripheral neuropathy and assured him they were on the cutting edge of care for pain patients. Johnson said he “never thought there was anything untoward going on” until he arrived on his last day and was told to pack up his belongings because the entire operation was shutting down.
Lags Medical performed other procedures at rates that also set them apart. From 2015 through 2020 ã the span for which KHN had state data ã Lags Medical performed more than 24,000 nerve ablations, a procedure in which part of a nerve is destroyed to reduce pain, on Medi-Cal patients. That’s more than 1 in 6 of all nerve ablations billed through Medi-Cal during that period.
An analysis of federal data also shows Lagattuta was an outlier. For example, in 2018 he billed Medicare for nerve ablations more often than 88% of the doctors in his field who performed the procedure.
Lags Medical also used the in-house lab to run drug tests on patients’ urine samples. From 2017 through 2019, Lags Medical facilities often ordered the most extensive ã and expensive ã set of drug tests, which check for the presence of at least 22 drugs, according to state and federal data.
For perspective, in 2019, more than 23,000 of the most extensive drug tests were ordered on Medi-Cal patients under Lagattuta’s provider number, more than double the number tied to the next highest biller. The next five top billers were all lab companies.
Overall, from 2017 through 2019, nearly 60,000 of the most extensive drug tests were billed to Medicare and Medi-Cal under Lagattuta’s provider number. Medicare reimbursed Lagattuta $5.4 million for these tests during that period. Using state fee-for-service rates, the testing billed to Medi-Cal would have been worth an estimated $6.3 million. That doesn’t include less extensive drug screens or those billed under other providers’ numbers.
Pain management experts described the use of extensive screening as unnecessary in routine pain treatment; the overuse of such tests has been the subject of numerous Medicare investigations in recent years.
Private pain clinics like Lags Medical are only loosely regulated and generally are not required to hold a special license from the state. But the physicians who work there are regulated by the Medical Board of California.
In December 2019, a patient who’d visited clinics in both Visalia and the Central Coast against Lagattuta with the medical board claiming, among other things, that she received biopsies that were not properly performed, that she underwent excessive testing, and that positive drug tests had been falsified. The medical board had another pain management doctor review more than 300 pages of documents and found “no deviations from the standard of care” and “did not find any over testing, or improperly performed biopsies.”
He did, however, find some record-keeping problems, including numerous procedures in which patient consent was not documented. He also found instances in which procedures were performed and repeated without documentation that they were effective. The patient who filed the complaint was given a medial branch nerve block in November 2014, followed by a radiofrequency ablation in December, and another in February. No improvements for the patient were ever noted in the charts, the investigating doctor found.
The medical board chalked it up to a record-keeping error and fined Lagattuta $350.
A Halfway-Normal Life
On a warm evening in late July, Leah Munoz drove her power wheelchair around the long plastic tables at the Veterans Memorial Building in Hanford, a dusty farm town in California’s Central Valley. Senior bingo night was crowded with gray-haired players waiting for the game to begin. She found an empty spot and carefully set out $50 worth of bingo cards, alongside her collection of 14 brightly colored daubers.
Munoz, 55 and a mother of six, said she has suffered from a litany of illnesses ã thyroid cancer, breast cancer, lupus, osteoarthritis ã that leave her in near-constant pain. She’s been playing bingo since she was a little girl, and said it helps distract from the pain and calm her mind. She looks forward to this event all week.
Munoz was a Lags Medical patient for about four years and, while her pain never disappeared, the opioids prescribed provided enough relief for her to continue doing the things she loved. “There’s a difference between addiction and dependence. I need it to live a halfway-normal life,” Munoz said.
After Lags Medical closed in May, her primary care doctor initially refused to refill her opioid prescriptions. She said she called the Lags Medical offices to try to get a copy of her medical records to prove her need, and even showed up in person. But she said she was unable to get them. As the pills dwindled and the pain surged, Munoz said, it became hard to leave her home. “I missed a lot of bingo, a lot of grocery shopping, a lot of going to my grandkids’ birthday parties. You miss out on life,” she said. Ultimately, she said, her primary care doctor referred her to another pain clinic, and she was able to resume her prescription.


Even with pain medications, Munoz said, she never received true relief during her time as a patient at Lags Medical. She said she felt coerced to get several injections, none of which seemed to help. “If I didn’t get the procedures, I didn’t get the pain medication,” she said. Her husband, Ramon, a landscaper who was also a patient, received an injection there that he said left him with permanent stiffness in his neck.
Munoz knows at least five other people at bingo night who were former patients at Lags Medical. One of them, Rick Freeman, came over to her table to chat. He swayed back and forth as he walked, his knees, he explained, swollen after 35 years living with HIV. At Lags Medical, Freeman said, he felt pressured by staff to receive injections if he wanted to continue receiving his opioid prescriptions. “If you don’t cooperate with them, they would reduce your meds down,” he said.
At the front of the room, Gail Soto, who ran the event, sold bingo cards to the latecomers. Soto, 72, said she injured her back while working an administrative job at a construction company years ago and suffers from spinal stenosis, rheumatoid arthritis, and fibromyalgia. She, too, was a patient at Lags Medical for years. In addition to her opioid prescription, Soto said, she received repeated injections and three nerve ablations. At first, the ablations helped, but what staff members didn’t tell her, she said, was that the nerves they destroyed could grow back. Ultimately, she said, the procedures left her in worse pain.
Soto’s biggest concern is the spinal stimulator that she said Lags Medical surgically inserted into her back five years ago. She said the doctors told her the device would work so well that she would no longer need her pain pills. She said they didn’t explain that the device would work only two hours a day, and on one side of her body. She remained in too much pain to give up her meds, she said, and, five years later, the battery is failing.
Soto sleeps in a recliner chair in her three-bedroom mobile home in Lemoore, another small city near Hanford. It’s well kept but humble, and she and her husband keep a collection of wind chimes on the front porch that create a wave of gentle music when a breeze passes by. The couple take good care of each other and their two beloved Chihuahuas, but life has become increasingly difficult for Soto.
As the battery on her spinal stimulator has started to fail, she said, she has sudden electrical pulses that shoot up her body. “My husband says sometimes when I sleep that my body will just jump up in the air,” she said. But now that Lags Medical is closed, she said, she can’t find a doctor willing to remove the device. “Most doctors are telling me right now, ãWe can’t, because we didn’t [put it in]. We don’t want nothing to do with that.’”

Waitlists and Withdrawal
Audrey Audelo Ramirez said she picked up her final refill from Lags Medical on June 4 and by July 4 had no meds left to treat her pain. Ramirez said she called every pain management clinic in Fresno, but none were taking new patients.
“They left us all high and dry,” she said. “Everybody.”
In the weeks that followed the closures, county officials throughout the Central Valley saw a flood of patients on high doses of opioids in search of new providers, they said. Patients couldn’t access their medical records, so other providers had no idea what their treatments had been.
“We had to create a crisis response to it because there was no organized response at that time,” said Dr. Rais Vohra, the interim health officer for Fresno County.
Fresno County’s health system is already lean, Vohra said. Toss in this abrupt closure and you end up in the kind of crisis rarely seen in other fields of medicine: “You’d never do this with a cancer clinic,” he said. “You’d never abruptly stop chemo.”
The state asked Dr. Phillip Coffin, director of substance abuse research for the San Francisco Department of Public Health, to run provider training and persuade doctors to take on new patients. Many practices have rules against taking new patients on opioids, or will refuse to prescribe doses above certain thresholds.
“We know that when you stop prescribing opioids, some people end up with death from suicide, overdose, increased illicit opioid use, pain exacerbations. It’s really important to have a continuity, and that is not really possible in the current opioid-prescribing culture,” Coffin said. The threat to patients is so severe that the FDA in 2019 against cutting patients off from prescription opioids.
Gina, a retired nurse who asked to be identified by only her first name for fear she’d be discriminated against by other doctors, had been a Lags Medical patient for six years. She said she called every practice she could find in her Central Coast town, and was put on a waiting list at one. Suffering from a severe case of scoliosis, she started rationing the pain pills she had come to rely on.
When she finally secured an appointment, she said, she was told by the doctor she was on “some very strong meds” and he would fill only one of her two prescriptions. “You’re like a criminal,” she said. “You’re branded as ãwe don’t trust you.’”
She started experiencing withdrawal symptoms ã sweating, lost appetite, sleeplessness, anxiety. Worst of all, her pain “came back with a vengeance,” she said.
“I think about this, what I’d have been like if I’d never gone through pain management. I sometimes wonder if I’d be better off.”
As for Ramirez, her primary care doctor finally secured an appointment for her at another pain clinic, she said. It was in the same space as the old Lags Medical clinic, and she said she recognized many of the staff members. But now there was a new name: Central California Pain Management. From her perspective, it was as if nothing had changed. And she still doesn’t know whether she needs to worry about the care she received during more than four years at Lags Medical.
The new clinic’s owner, Dr. Ashok Parmar, said that he is leasing the space and that Lagattuta is his landlord. Parmar said he doesn’t do punch biopsies, nor does he diagnose small fiber neuropathy. After all, he said, he would treat the pain the same way, with or without the diagnosis.
How We Did This
KHN evaluated the billing practices of physicians and clinics associated with Lags Medical Centers using data from both Medicare and Medi-Cal.
KHN did multiple analyses using that show, for each medical practitioner or lab, every procedure or service billed to the federal government, along with the number of times a procedure was performed, the number of Medicare beneficiaries who received specific services, and how much Medicare reimbursed. The Part B records include billings from 2015 through 2019, the most recent years available. The records are limited to beneficiaries who have traditional fee-for-service Medicare rather than private Medicare Advantage plans. Medicare suppressed data in cases in which a provider performed a procedure on 10 or fewer beneficiaries in a year.
KHN analyzed Medicare billing records for a range of specific procedures, comparing Dr. Francis P. Lagattuta’s billings with those of other practitioners who also identified themselves in the records as Physical Medicine and Rehabilitation specialists.
Through a public records request, KHN also obtained data from the California Department of Health Care Services for a range of specific medical procedures performed on state Medi-Cal recipients by all California providers from 2015 through 2020, as well as every service rendered through Medi-Cal under Lagattuta’s provider number during that time. The Medi-Cal data is organized to show both the rendering and billing provider for a procedure, allowing KHN to look across the network of Lags Medical clinics. To calculate services provided at Lags Medical Centers, KHN included services performed under Lagattuta’s provider number, as well as active provider numbers of organizations with a mailing address associated with Lags Medical clinics that listed Dr. Francis P. Lagattuta or another Lags employee as their authorized official. DHCS suppressed data for instances in which a provider performed a procedure fewer than 11 times on Medi-Cal patients in a year.
The Medi-Cal data did not include reimbursement amounts for procedures, so KHN obtained historical reimbursement amounts from DHCS to calculate the value of the services based on the fee-for-service reimbursement rate in July of each year. Care received by patients with Medi-Cal is generally reimbursed by the state in one of two ways: a fee-for-service model, in which physicians are reimbursed for services according to a set fee schedule that is public; or a managed-care model, in which the state pays insurers a monthly fee per patient, and the insurers reimburse providers amounts that are not public. Only a small percentage of Lags Medical services were reimbursed through fee-for-service plans during the years reviewed. As a result, the values of procedures calculated by KHN are meant to convey a general estimate of their worth. All estimates are calculated using .
KHN senior correspondent Jordan Rau and Phillip Reese, an assistant professor of journalism at California State University-Sacramento, contributed to this report.
This story was produced by , which publishes , an editorially independent service of the .
This <a target="_blank" href="/health-industry/lags-medical-pain-clinic-chain-closure-troubling-questions-opioids-injections/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1437713&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Should I travel to see an elderly relative? Can I see my friends and, if so, is inside OK? Mask or no mask? Test or no test? What day? Which brand? Is it safe to send my child to day care?
Questions that once felt trivial have come to bear the moral weight of a life-or-death choice. So it might help to know (as you’re tossing and turning over whether to cancel your non-refundable vacation) that your struggle has a name: decision fatigue.
In 2004, psychologist Barry Schwartz wrote an influential book, “The Paradox of Choice: Why More Is Less.” The basic premise is this: Whether picking your favorite ice cream or a new pair of sneakers or a family physician, choice can be a wonderful thing. But too many choices can leave us feeling paralyzed and less satisfied with our decisions in the long run.
And that’s just for the little things.
Faced with a stream of difficult choices about health and safety during a global pandemic, Schwartz suggests, we may experience a unique kind of burnout that could deeply affect our brains and our mental health.
Schwartz, an emeritus professor of psychology at Swarthmore College and a visiting professor at the Haas School of Business at the University of California-Berkeley, has been studying the interactions among psychology, morality, and economics for 50 years. He spoke with KHN’s Jenny Gold about the decision fatigue that so many Americans are feeling two years into the pandemic, and how we can cope. The conversation has been edited for length and clarity.
Q: What is decision fatigue?
We all know that choice is good. That’s part of what it means to be an American. So, if choice is good, then more must be better. It turns out, that’s not true.
Imagine that when you go to the supermarket, not only do you have to choose among 200 kinds of cereal, but you have to choose among 150 kinds of crackers, 300 kinds of soup, 47 kinds of toothpaste, etc. If you really went on your shopping trip with the aim of getting the best of everything, you’d either die of starvation before you finished or die of fatigue. You can’t live your life that way.
When you overwhelm people with options, instead of liberating them, you paralyze them. They can’t pull the trigger. Or, if they do pull the trigger, they are less satisfied, because it’s so easy to imagine that some alternative that they didn’t choose would have been better than the one they did.
Q: How has the pandemic affected our ability to make decisions?
In the immediate aftermath of the pandemic, all the choices that we faced vanished. Restaurants weren’t open, so you didn’t have to decide what to order. Supermarkets weren’t open, or they were too dangerous, so you didn’t have to decide what to buy. All of a sudden your options were restricted.

But, as things eased up, you sort of go back to some version of your previous life, except [with] a whole new set of problems that none of us thought about before.
And the kinds of decisions you’re talking about are extremely high-stakes decisions. Should I see my parents for the holidays and put them at risk? Should I let my kid go to school? Should I have gatherings with friends outside and shiver, or am I willing to risk sitting inside? These are not decisions we’ve had practice with. And having made this decision on Tuesday, you’re faced with it again on Thursday. And, for all you know, everything has changed between Tuesday and Thursday. I think this has created a world that is just impossible for us to negotiate. I don’t know that it’s possible to go to bed with a settled mind.
Q: Can you explain what’s going on in our brains?
When we make choices, we are exercising a muscle. And just as in the gym, when you do reps with weights, your muscles get tired. When this choice-making muscle gets tired, we basically can’t do it anymore.
Q: We’ve heard a lot about more people feeling depressed and anxious during the pandemic. Do you think that decision fatigue is exacerbating mental health issues?
I don’t think you need decision fatigue to explain the explosion of mental health problems. But it puts an additional burden on people.
Imagine that you decided that, starting tomorrow, you are going to be thoughtful about every decision you make. OK, you wake up in the morning: Should I get out of bed? Or should I stay in bed for another 15 minutes? Should I brush my teeth, or skip brushing my teeth? Should I get dressed now, or should I get dressed after I’ve had my coffee?
What the pandemic did for a lot of people is to take routine decisions and make them non-routine. And that puts a kind of pressure on us that accumulates over the course of the day, and then here comes tomorrow, and you’re faced with them all again. I don’t see how it could possibly not contribute to stress and anxiety and depression.
Q: As the pandemic wears on, are we getting better at making these decisions? Or does the compounded exhaustion make us worse at gauging the options?
There are two possibilities. One is that we are strengthening our decision-making muscles, which means that we can tolerate more decisions in the course of a day than we used to. Another possibility is that we just adapt to the state of stress and anxiety, and we’re making all kinds of bad decisions.
In principle, it ought to be the case that when you’re confronted with a dramatically new situation, you learn how to make better decisions than you were able to make when it all started. And I don’t doubt that’s true of some people. But I also doubt that it’s true in general, that people are making better decisions than they were when it started.
Q: So what can people do to avoid burnout?
First, simplify your life and follow some rules. And the rules don’t have to be perfect. [For example:] “I am not going to eat indoors in a restaurant, period.” You will miss out on opportunities that might have been quite pleasant, but you’ve taken one decision off the table. And you can do that with respect to a lot of things the way that, when we do our grocery shopping, we buy Cheerios every week. You know, I’m going to think about a lot of the things I buy at the grocery, but I’m not going to think about breakfast.
The second thing you can do is to stop asking yourself, “What’s the best thing I can do?” Instead, ask yourself, “What’s a good enough thing I can do?” What option will lead to good enough results most of the time? I think that takes an enormous amount of pressure off. There’s no guarantee that you won’t make mistakes. We live in an uncertain world. But it’s a lot easier to find good enough than it is to find best.
This <a target="_blank" href="/mental-health/ready-for-another-pandemic-malady-its-called-decision-fatigue/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1444158&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>First came the anti-mask protests, amplified by vows from that her deputies would refuse to enforce the state’s mask mandate. Next was the vocal resentment of covid-related business restrictions. Cap that off with roiling distrust of the new covid vaccines and a large migrant farmworker population with long-standing challenges accessing health care. Little surprise, then, that as of Dec. 3, of Fresno County residents were fully vaccinated, nearly 10 percentage points lower than the statewide average. In some rural pockets of the county, of residents are fully vaccinated.
For almost two years, Vohra and the rest of the county’s health care system have struggled to keep up with what has felt like an unrelenting series of covid surges. The current wave has , with emergency rooms so packed that ambulances line up for hours waiting to offload patients. have been recorded, and more than 2,200 residents have died.
Fresno County stretches over 6,000 square miles and includes the city of Fresno ã the Central Valley’s urban core ã as well as vast expanses of farmland. The county is home to about 1 million residents, a little more than half of whom are Latino.
Vohra, who is also a professor of clinical emergency medicine at UCSF-Fresno, spoke with KHN’s Jenny Gold about the “why” behind the persistent surges and the toll on Fresno’s health care system. The conversation has been edited for length and clarity.

Q: Fresno County’s is four times what Los Angeles County is seeing and eight times San Francisco’s rate. Why?
The whole state experienced a surge in the fall. And when the surge resolved in the rest of the state, unfortunately our numbers did not come down. We plateaued. We may be having another surge this winter, so not to be able to recover our resources and give people time to debrief and think about how to prepare for the next one is obviously very concerning.
Our vaccination rates are not where we need them to be. The amount of masking that we have is definitely lower, and we weren’t able to get a mask mandate. We also have a lot of essential workers. A remote worker who can “Zoom in” is very different from someone who works at Foster Farms, who has to show up and doesn’t have any time off left. Every little thing is connected to every other little thing.
Q: Why does the county’s vaccination rate continue to lag behind rates in much of the state?
There are some people who are still struggling with access, and we’re absolutely trying to address that. Then there are other people who are just not accepting the science, and I don’t know how to get those folks to buy in. I think that the emotion comes first and the reasoning comes later.
Is it disappointing? Yeah, it is. Are we trying to do the right thing and improve that rate? Of course we are.
But when you look at all the things that we’ve been hearing, sometimes I’m pleasantly surprised. A million doses of vaccine have been given. If you told me a year ago we were going to get that done in less than a year, I would not have believed it.
Q: Fresno’s hospital network is struggling to absorb the covid patient load and has pleaded with other counties to take patients. Are you getting help?
We have only seven acute care hospitals here in Fresno County. We probably need twice that many to serve the population. They’re always running at a very high capacity, sometimes over 100% of what they’re licensed for. And so this covid surge really was very challenging.
You would think that given all of our informatics technology, we would have a way to share the burden and transfer people. But that’s not how the system is designed. We had a great conversation with our state partners and all the other hospitals to talk about this, and I’m hoping that something materializes. But these are not easy questions to answer.
In addition to just the logistical issues of finding an open bed and an EMS [emergency medical services] transportation vehicle with the right people able to manage a critically ill patient over hundreds of miles, you also have to have patients consenting. And, it turns out, patients and their families actually resist if you tell them, “Your family member is going to get great care, but it’ll be 100 or 200 miles away.”
Q: When you said Fresno needs twice as many hospitals, did you mean in covid times or normal times?
Non-covid times. We have such a shortage of clinicians and we have such a shortage of nurses that it’s really hard to meet the needs of the patients. The population has grown a lot faster than the hospitals.
Rural hospitals are actually limiting their services, not adding new ones, and that’s just part of a much larger and more tragic story about the health care landscape.
Q: As health officer in Fresno County, you’re operating at a point of natural tension amid the anti-mask and anti-vaccination sentiments. How have you been navigating that?
It’s been very interesting, very humbling and also very instructive. It actually makes us have to be very sure about the recommendations we’re making, because we know they’re going to get scrutinized.
Sometimes we’re disappointed. For example, we really tried hard to get a mask mandate when we saw that the fall surge was impending. And, unfortunately, our county just did not want to embrace that. People were just ready to be done, and to bring it back was not even an option.
Q: I imagine the public health staff and health care providers are exhausted. What are you seeing?
There’s an element of exhaustion and fatigue that I’ve never seen in my colleagues before the pandemic came along. In the early days, we all talked about health care heroes, and even though it was scary and surreal, we had a lot of adrenaline. But that ran out a long time ago. Now people are just managing as best they can.
In the hospitals, many people are really just fed up with a lot of this anti-vaccination sentiment. Because they’re the ones taking care of the people who get sick. It is very sad to see and to live through. What it does, though, is bond people in a way that only severe trauma can. At this point, if you’re still going into work every day, despite your exhaustion, it’s because you really love the team that you’re working with. I certainly see that in our health department.
Q: Your wife, Dr. Stacy Sawtelle Vohra, is an emergency physician at Community Regional Medical Center in Fresno, so also on the covid front lines. What has been the toll on your family?
Whenever there’s high transmission in our community, that affects us personally, too, and people have to take time off of work to take care of relatives or get checked out. We’ve had our kids tested because they came down with the sniffles. And you have to keep a kid out of school when they get their test. Living through that, you understand that if I wasn’t able to do my meetings from home, this would become just an impossibility. We haven’t created good solutions for our communities, especially for parents who have to work and don’t have good child care options.
We’re both fortunate that we have employers that are understanding and flexible. We have two young children who are 4 and 7, and their biggest priority was to make sure that the showed up today. For better or worse, we’re good compartmentalizers, and we just leave all that stuff at the office or in the emergency department. And when we’re home, we’re a family. We just hope to give them as normal a childhood as they can have during this really challenging time.
This <a target="_blank" href="/public-health/fresno-county-covid-surge-interview-health-officer-rais-vohra/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1416978&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>So far, about half of kids 12 to 17 are fully vaccinated in the U.S., compared with nearly 70% of Americans 18 and older. Pediatricians expect it will be even harder to persuade skeptical parents of younger children to get their kids inoculated. Many are concerned about the potential unknowns of a relatively new vaccine compared with the low risk of serious illness covid poses for children.
found 27% of parents of children 5 to 11 said they plan to get them vaccinated “right away,” while 30% said they would “definitely not” get the vaccine for their 5- to 11-year-olds. More than three-quarters of parents of children in this age group reported they were “very” or “somewhat” concerned that not enough is known about the long-term effects of the vaccine in kids.
“I’m not quite on board with everybody getting vaccinated,” said Tara Currier, 42, a mother of four in Marysville, California, who decided not to vaccinate her three older children, ages 12, 14 and 16. She said she also plans to delay vaccinating her 10-year-old daughter.
While she is fully vaccinated herself, Currier said she won’t vaccinate her children until she can be certain the shot is “actually a protection and not something that’s going to affect their bodies later on. I don’t know that can be answered yet, because the vaccine hasn’t been seen in people for very long.”
Public health officials and leading experts have been increasingly vocal in emphasizing that while children are at lower risk of serious illness from covid, they are not at zero risk. Nearly 6.3 million children have tested positive for covid, and more than 580 have died, according to . A small percentage have developed long-term symptoms.
They also stress that vaccinating children is essential to slowing the spread of the virus in the broader population. Nationwide, people have been infected by SARS-CoV-2, which causes covid, and more than 745,000 have died.
The Food and Drug Administration authorized the Pfizer-BioNTech covid vaccine for emergency use in children ages 12-15 , after approving the same shot for teens 16 and older five months earlier. On Friday, the agency authorized for emergency use a smaller dose of the vaccine for children ages 5-11, and shots are expected to be available this week following signoff by the Centers for Disease Control and Prevention.
In clearing the Pfizer vaccine for children and teens, the FDA said ongoing clinical studies show children and adolescents face greater risks from covid and its potentially devastating side effects than they do from a rare side effect of the vaccine involving inflammation of the heart reported in some young adults.
Still, California offers a lens on the challenges health officials and pediatricians face in persuading parents nationwide to embrace the new shots. The state ranks in the nation’s top quartile in overall vaccination rates, of people 12 and older vaccinated, according to the CDC. But that number masks vast disparities among the older and younger age groups.
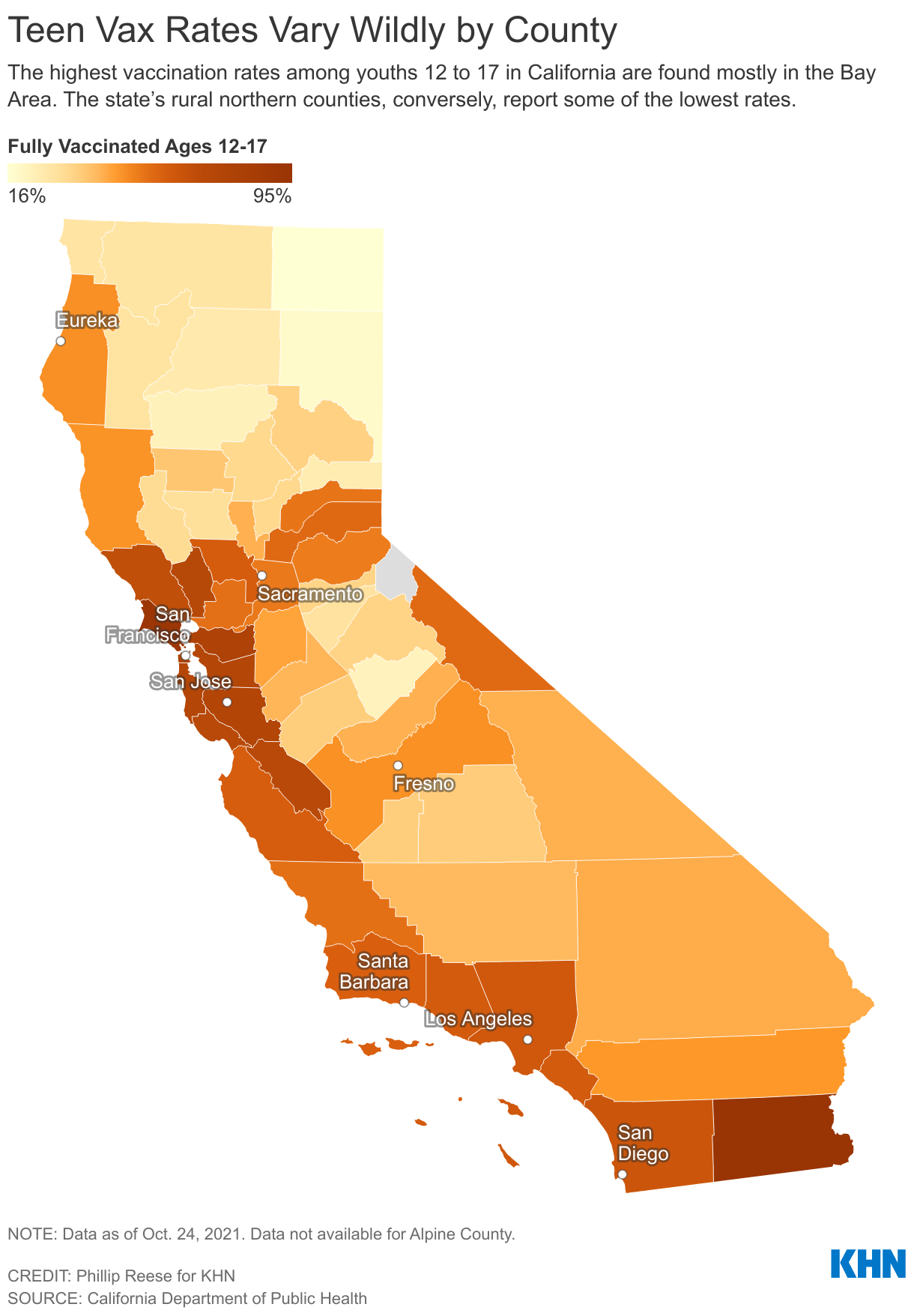
Statewide, just 59% of kids 12 to 17 were fully vaccinated by Oct. 24. By comparison, 71% of people 18 to 49 were vaccinated by that date; 80% of residents 50 to 64; and 75% of residents 65 and older.
In addition, teen vaccination rates vary hugely by region, another microcosm of the U.S. While many of the wealthier urban and suburban counties along the California coast boast vaccination rates upward of 70% for kids 12 to 17, multiple counties in the state’s rugged north report fewer than a quarter of that age group are vaccinated.
Marin County is one of the state’s success stories. Relatively wealthy, decidedly Democratic and overwhelming white, the county had vaccinated 93% of kids 12 to 17 as of Oct. 19, according to the California Department of Public Health. That’s more than twice the rate of 12- to 17-year-olds vaccinated in rural Madera County in the Central Valley; and it dwarfs the 16% of kids 12-17 vaccinated in Modoc County in the state’s mountainous northeast.
When younger teenagers became eligible in the spring, public health officials in Marin County set up two mass vaccination sites with “lots of fanfare and confetti and a ribbon-cutting kind of feeling,” said county public health officer Dr. Matt Willis. Families were eager, and within 10 days, the county had vaccinated half their adolescent population.
For parents who were more hesitant, “pediatricians were crucial,” Willis said. Dr. Nelson Branco, a pediatrician in Larkspur, said his practice waited a few weeks before opening its own vaccination clinic. They checked the vaccine registry for their 4,000 12- to 17-year-old patients, identified 800 who had not been vaccinated, then sent out an email blast inviting them to one of their weekly clinics and to call with any questions.
“We found that there were lots of parents of teenagers who are very anxious for their kids to get back to more normal activities,” said Branco. “We’re seeing the same things with parents of younger kids. The question is ‘When?’ not ‘Should I?’”
In a rural county like Madera, which hasn’t voted for a Democratic president since Jimmy Carter, the low vaccination rates reflect factors beyond a conservative political bent, said Dr. Nicole Webb, a pediatrician at Valley Children’s Healthcare in Madera. Rather, many residents face logistical challenges that don’t exist for Californians in the suburbs and cities, where a pharmacy or doctor’s office is a short drive or transit ride away.
“I think the tempting thing is to try to make global generalizations based on political or ideological blinds, but I think it’s actually a lot more complicated than that in a place like this,” Webb said.
Even in counties reporting high teen vaccination rates, there are pockets where pediatricians are struggling to convince wary parents. Santa Clara County has vaccinated 75% of kids 12 to 17, according to CDPH. But at her practice in central San Jose, Dr. Amna Khan said most of her patients are on the fence.
Santa Clara Valley Medical Center sees mostly Medi-Cal patients, and many of Khan’s patients are recent immigrants. “In my patient population, they have a lot of reason to distrust the government and medicine in general,” Khan said. “It’s not a political statement. It’s distrust from things they’ve heard from their family or church or neighbors.”
Often, these conversations are a “difficult dance” that Khan must navigate with cultural sensitivity and help from translators. Sometimes, she faces the minefield of parent-teen conflict, with arguments breaking out in the exam room between kids who want the vaccine and parents who refuse.
No matter where parents are raising their kids, pediatricians said, the common factor driving their decision to vaccinate — or not — is concern about their child’s safety.
Parents lining up to vaccinate their children are worried about the threat of covid. Parents hesitant about the shot are worried about possible side effects of the vaccine. Somewhere in the middle are parents unsure what to think because of the conflicting information they have gotten from social media or friends.
Even among parents who have unquestioningly vaccinated their children for other diseases, the choice on covid isn’t an obvious one.
“Parents are now saying, ‘You know what? I don’t think this is right for my kid. I don’t think I’m going to make this decision, or at the very least I’m going to wait at least six months, maybe a year or maybe longer before I even consider this for my child,’” said , a professor of sociology at Indiana University who has been monitoring a group of moms in Indiana throughout the pandemic.
“They’ll say, ‘You know what, my kid wears masks. We wash our hands. We are responsible with play dates. And so, the vaccine just isn’t necessary because we’re doing enough, and my kid is healthy enough that they will probably be fine.’”
Doctors and public health officials say they find themselves regularly explaining to parents that covid is indeed harming kids.
“There have been more than 35 pediatric deaths in California alone, and this is more deaths than we see with flu,” Dr. Erica Pan, California’s state epidemiologist, told reporters last week. “This simply is not an acceptable number of child deaths when such effective and safe prevention is available.”
Covid has triggered multisystem inflammatory syndrome in children, a potentially life-threatening condition in which the immune system attacks the body and impedes organ function, in more than 660 California kids since March 2020, Pan said. Six have died.
California is slated to have more than 1.2 million doses of the weaker version of the vaccine for kids 5 to 11 the first week the vaccine is approved for emergency use, Pan said. Pediatricians will be crucial to the state’s efforts to vaccinate kids, along with clinics at school sites and door-to-door campaigns by community leaders.
In Yuba City, pediatrician Dr. Mark Sawyer tells patients, “If you want to stop hearing about covid on the radio and stop hearing about lockdowns and everything, then this is it, this is the way. Just get vaccinated.”
Phillip Reese, an assistant professor of journalism at California State University-Sacramento, contributed to this report.
This story was produced by , which publishes , an editorially independent service of the .
µÍºÇ¨û§ØŸl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/covid-vaccination-teens-parents-proving-tough-sell/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1400024&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>One in every three American families cannot afford enough diapers to keep their infants and toddlers clean, dry and healthy, according to the National Diaper Bank Network. For many parents, that leads to wrenching choices: diapers, food or rent?
The covid-19 pandemic has exacerbated the situation, both by expanding unemployment rolls and by causing supply chain disruptions that have triggered higher prices for a multitude of products, . Diaper banks ã community-funded programs that offer free diapers to low-income families ã distributed 86% more diapers on average in 2020 than in 2019, according to the National Diaper Bank Network. In some locations, distribution increased by as much as 800%.
Yet no federal program helps parents pay for this childhood essential. The government’s food assistance program does not cover diapers, nor do most state-level public aid programs.
California is the only state to directly fund diapers for families, but support is limited. CalWORKS, a financial assistance program for families with children, provides $30 a month to help families pay for diapers for kids under age 3. Federal policy shifts also may be in the works: Democratic lawmakers are pushing to include $200 million for diaper distribution in the massive budget reconciliation package.
Without adequate resources, low-income parents are left scrambling for ways to get the most use out of each diaper. This stressful undertaking is the subject of in American Sociological Review by Jennifer Randles, a professor of sociology at California State University-Fresno. In 2018, Randles conducted phone interviews with 70 mothers in California over nine months. She tried to recruit fathers as well, but only two men responded.
Randles spoke with KHN’s Jenny Gold about how the cost of diapers weighs on low-income moms, and the “inventive mothering” many low-income women adopt to shield their children from the harms of poverty. The conversation has been edited for length and clarity.

Q: How do diapers play into day-to-day anxieties for low-income mothers?
In my sample, half of the mothers told me that they worried more about diapers than they worried about food or housing.
I started to ask mothers, “Can you tell me how many diapers you have on hand right now?” Almost every one told me with exact specificity how many they had ã five or seven or 12. And they knew exactly how long that number of diapers would last, based on how often their children defecated and urinated, if their kid was sick, if they had a diaper rash at the time. So just all the emotional and cognitive labor that goes into keeping such careful track of diaper supplies.
They were worrying and figuring out, “OK, I’m down to almost my last diaper. What do I do now? Do I go find some cans [to sell]? Do I go sell some things in my house? Who in my social network might have some extra cash right now?” I talked to moms who sell blood plasma just to get their infants diapers.
Q: What coping strategies stood out to you?
Those of us who study diapers often call them diaper-stretching strategies. One was leaving on a diaper a little bit longer than someone might otherwise leave it on and letting it get completely full. Some mothers figured out if they bought a [more expensive] diaper that held more and leaked less, they could leave the diaper on longer.
They would also do things like letting the baby go diaperless, especially when they were at home and felt like they wouldn’t be judged for letting their baby go without a diaper. And they used every household good you can imagine to make makeshift diapers. Mothers are using cloth, sheets and pillowcases. They’re using things that are disposable like paper towels with duct tape. They’re making diapers out their own period supplies or adult incontinence supplies when they can get a sample.
One of the questions I often get is, “Why don’t they just use cloth?” A lot of the mothers that I spoke with had tried cloth diapers and they found that they were very cost- and labor-prohibitive. If you pay for a full startup set of cloth diapers, you’re looking at anywhere from $500 to $1,000. And these moms never had that much money. Most of them didn’t have in-home washers and dryers. Some of them didn’t even have homes or consistent access to water, and it’s illegal in a lot of laundromats and public laundry facilities to wash your old diapers. So the same conditions that would prevent moms from being able to readily afford disposable diapers are the same conditions that keep them from being able to use cloth.
Q: You found that many women’s concept of being a good mother is wrapped up in diapering. Why is that?
Diapers and managing diapers was so fundamental to their identity as good moms. Most of the mothers in my sample went without their own food. They weren’t paying a cellphone bill or buying their own medicine or their own menstrual supplies, as a way of saving diaper money.
I talked to a lot of moms who said, when your baby is hungry, that’s horrible. Obviously, you do everything to prevent that. But there’s something about a diaper that covers this vulnerable part of a very young baby’s body, this very delicate skin. And being able to do something to meet this human need that we all have, and to maintain dignity and cleanliness.
A lot of the moms had been through the welfare system, and so they’re living in this constant fear [of losing their children]. This is especially true among mothers of color, who are much more likely to get wrapped up in the child welfare system. People can’t necessarily see when your baby’s hungry. But people can see a saggy diaper. That’s going to be one of the things that tags you as a bad mom.
Q: Was your work on diapers influenced by your experience as a parent?
When I was doing these interviews, my daughter was about 2 or 3. So still in diapers. When my daughter peed during a diaper change, I thought, “Oh, I can just toss that one. Here, let me get another clean one.” That’s a really easy choice. For me. That’s a crisis for the mothers I interviewed. Many of them told me they have an anxiety attack with every diaper change.
Q: Do you see a clear policy solution to diaper stress?
What’s kind of ironic is how much physical, emotional and cognitive labor goes into managing something that society and lawmakers don’t even recognize. Diapers are still not really recognized as a basic need, as evidenced by the fact that they’re still taxed in 35 states.
I think what California is doing is an excellent start. And I think diaper banks are a fabulous type of community-based organization that are filling a huge need that is not being filled by safety net policies. So, public support for diaper banks.
The direct cash aid part of the social safety net has been all but dismantled in the last 25 years. California is pretty generous. But there are some states where just the cost of diapers alone would use almost half of the average state TANF [Temporary Assistance for Needy Families] benefit for a family of three. I think we really do have to address the fact that the value of cash aid buys so much less than it used to.
Q: Your body of work on marriage and families is fascinating and unusual. Is there a single animating question behind your research?
The common thread is: How do our safety net policies support low-income families’ parenting goals? And do they equalize the conditions of parenting? I think of it as a reproductive justice issue. The ability to have a child or to not have a child, and then to parent that child in conditions where the child’s basic needs are met.
We like to say that we’re child and family friendly. The diaper issue is just one of many, many issues where we don’t really put our money or our policies where our mouth is, in terms of supporting families and supporting children. I think my work is trying to get people to think more collectively about having a social responsibility to all families and to each other. No country, but especially the richest country on the planet, should have 1 in 3 very young children not having one of their basic needs met.
I interviewed one dad who was incarcerated because he wrote a bad check. And as he described it to me, he had a certain amount of money, and they needed both diapers and milk for the baby. And I’ll never forget, he said, “I didn’t make a good choice, but I made the right one.”
These are not fancy shoes. These are not name-brand clothes. This was a dad needing both milk and diapers. I don’t think it gets much more basic than that.
This <a target="_blank" href="/public-health/down-to-my-last-diaper-the-anxiety-of-parenting-in-poverty/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1394600&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>NEED HELP?
If you or someone you know is in a crisis, please call the National Suicide Prevention Lifeline at 1-800-273-TALK (8255) or contact the Crisis Text Line by texting HOME to 741741.
In September 2020, Congress passed bipartisan legislation creating a three-digit national suicide hotline: 988. Think of it as an alternative to 911 for mental health emergencies.
The system is intended to make it easier to seek immediate help during a mental health crisis. Instead of calling 911 or the 10-digit national suicide hotline, Americans theoretically will be able to speak to a trained counselor by calling 988 from most any phone line.
The federal law allows states to raise funds for the effort by levying a surcharge on monthly bills for mobile and landline phone service. The money can be used to support the dedicated call centers, pay for trained mobile response teams to be dispatched instead of armed law enforcement officers, and bolster stabilization services for people in crisis.
States are required to have some version of the 988 system up and running by July 2022. But the actual shape it takes is up to each state.
In California, the state Department of Health Care Services in September it would spend $20 million to help launch the 988 system. is legislation that would tack on up to 80 cents a month on phone lines in the state ã both wireless and landline services ã to provide ongoing funding for the system and associated services. The bill has faced opposition from the telecommunications industry, which argues the fee should be capped at 10 cents and fund only the cost of routing 988 calls to an appropriate crisis center. The bill has passed the Assembly and is expected to be taken up by the Senate next year.
Assembly member Rebecca Bauer-Kahan, an Orinda Democrat, is the principal author of AB 988, which she called the “Miles Hall Lifeline Act” in honor of a who was fatally shot by police in Walnut Creek during a mental health crisis. His family said he had been diagnosed with schizoaffective disorder.
Bauer-Kahan, a Bay Area lawyer, talked to KHN’s Jenny Gold about efforts to get 988 operational in California and what the new system might be able to accomplish. The conversation has been edited for length and clarity.
Q: The new federal law requires that every state have a 988 phone system in place by July. How is California doing, and will we be ready?
I’m hopeful that we will. We definitely have more work to do. We appropriated $20 million in September to ensure that we have the startup costs to build up our call centers. The data is showing that we should expect about a 30% increase in call volume [for California’s 13 suicide prevention call centers] when the rollout happens for 988 in July. So, it’s really critical to ensure that the call centers have the ability to increase staffing, and train people so that we’re prepared.
Q: Why is it important to have an emergency system dedicated exclusively to mental health?
This is a health care issue, but currently it’s being treated as a public safety issue. And that’s leading to a whole host of problems. I’d say the largest problem is that [an estimated] are people in mental health crisis. So that tells us that we aren’t getting the support we need to the people who need it.
Our law enforcement has been incredibly supportive of this effort because they know that there are people better trained to manage people who are in crisis. The largest mental health provider in the nation is the L.A. County jail, which is just the most upsetting thing I’ve heard. People shouldn’t be treated in our jails.
Q: What does the completed 988 system look like?
The federal legislation dictated that 988 calls have to be answered by certified suicide prevention call centers. We have 13 of those call centers in California, so they will be the people who answer.
Behind the call, the county where you live would be listening and determining whether you need dispatch. We believe, actually, a good percentage of callers will be served via just a phone call. But for those that need a response on the ground, there would be a warm handoff to county services.
People who have law enforcement showing up today would instead get a mobile crisis team show up to support them in that moment of crisis. Then they’d be handed off to stabilization services and long-term care for their mental health needs.
Q: What happens after emergency personnel respond to a 988 call? Would the patient be routed into a system that looks different from the one we have now, where people are so often taken to an emergency room or jail?
The goal is yes. They wouldn’t go to jail, because law enforcement isn’t the responder. So our jails would not continue to be our largest mental health care providers, but we would be building up a network of services.
Some people do need in-patient care that cannot be provided outside of the hospital, and we should make sure we have the [necessary] beds, which we don’t today. If somebody needs somebody to talk to weekly, then the county will be able to provide those services.
[We need to ensure that] the counties, who really should be the service providers, have the resources to provide care to those in need. And, currently, we just are woefully inadequate in the services that we can provide. The bill really defers to the counties with appropriate funding to create a system that will work for the community.
Q: We have a crisis that extends well beyond the point of police intervention, considering we don’t have places to treat people during mental health emergencies. Is that part of the vision for 988, or does it deal mostly with this very specific moment of initial contact?
I’ve always said in thinking about this legislation that this is a small piece of the puzzle. I will not say that I’m solving mental health in one piece of legislation. I am really focused on this piece of where we have law enforcement responding inappropriately today. How do we turn that into a health care response?
Now, do we need a complete, robust health care, mental health system underneath it? Yes. Am I creating that all through 988? No.
So there’s a lot of work that I think will go with this. I think it’s this incredible step in the right direction, but I by no means believe that it is going to solve all of our problems. The end goal is to have a complete continuum of care, so that the counties are able to provide the services that each individual needs to get them to a healthy place.
Q: Is there a way to raise funding through 988 to help with that broader continuum?
The bill funds both the mobile crisis response and stabilization services. So, we anticipate funding more than just the telephone operators. And we have fought tooth and nail to ensure that funding remains in the bill, because we believe that the phone system will be inadequate unless we have the services behind it to actually provide folks with the ability to be stabilized by their local counties.
[Having] the resources to provide exactly what each person in crisis needs is absolutely the goal. 988 is a piece of that puzzle. Sometimes you take the first step.
NEED HELP?
If you or someone you know is in a crisis, please call the National Suicide Prevention Lifeline at 1-800-273-TALK (8255) or contact the Crisis Text Line by texting HOME to 741741.
µÍºÇ¨û§ØŸl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/mental-health/988-mental-health-line-california-how-it-will-work/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1386273&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The settlement is expected to have nationwide implications on how hospital systems negotiate prices with insurers.
“These plaintiffs are among the first, but will not be the last, to successfully challenge dominant health care systems who undertake land grabs to mark up prices at the expense of patients and employers,” Leemore Dafny, a Harvard Business School professor who studies the industry, wrote in an email. “This settlement has provided a marker for the rest of the nation.”
The settlement, which includes $575 million in damages, was announced on a preliminary basis in December 2019. It marked a dramatic turn in a long-running legal battle initiated in 2014 as a class-action lawsuit filed by the United Food and Commercial Workers International Union & Employers Benefit Trust, representing employers, unions and local governments whose workers use Sutter services. Then-Attorney General Xavier Becerra joined the case in 2018.
Numerous twists and turns have slowed the court’s approval of the settlement in the months since.
San Francisco Superior Court Judge Anne-Christine Massullo had been expected to issue a preliminary approval of the terms in August 2020, but rejected the independent monitor the parties had chosen to oversee the rollout of the agreement. The monitor chosen was neither a woman nor a person of color, and Massullo said the parties’ selection process did not properly take into account the court’s emphasis on diversity, equity and inclusion.
More months passed as Sutter argued for further delays and suggested it would push to alter the settlement in light of the potentially dramatic effects of the covid-19 pandemic on the health care system’s finances and operations.
Preliminary approval was eventually granted, but most recently, final approval was postponed because of a dispute between UEBT and their lawyers over attorney fees. The parties had agreed earlier to plaintiffs’ attorneys, led by Richard Grossman of Pillsbury & Coleman, getting 30% of the settlement amount. Given the size of the settlement, that comes to $172.5 million in attorney fees, a figure UEBT now argues is unreasonably high.
An additional 2% in fees will go to the Attorney General’s Office. UEBT expects to receive about $15 million, and what is left of the $575 million will be distributed among the rest of the class, made up of other unions and employers who purchase health insurance for their workers.
Thursday’s hearing was largely devoted to a tense back-and-forth over the attorney fees. Ultimately, the hearing concluded without resolution on the issue. But Massullo indicated she would approve the terms of the settlement in a written order once the fees had been sorted out. The timing of that final order was left unclear.
Sutter has 23 hospitals, 33 surgery centers and 12,000 physicians across Northern California, with . Among other allegations, the state’s lawsuit argued Sutter has aggressively bought up hospitals and physician practices throughout the Bay Area and the rest of Northern California, and exploited that market dominance for profit.
Health care costs in Northern California are 20% to 30% higher than in Southern California, even after adjusting for the cost of living, according to a 2018 study from the Nicholas C. Petris Center at the University of California-Berkeley that was cited in the complaint.
Among other terms, the settlement requires Sutter to:
- Limit what it charges patients for out-of-network services.
- Increase transparency by allowing insurers and employers to give patients pricing information.
- Cease bundling services and products, and instead offer stand-alone pricing.
In agreeing to the settlement, Sutter did not admit wrongdoing. Throughout the proceedings, it has maintained that its integrated health system offers tangible benefits for patients, including affordable rates and consistent high-quality care. Sutter spokesperson Amy Thoma Tan said in an email that the settlement would not reduce the quality of patient care.
“Our commitment to providing high-quality care to our patients is unwavering, and independent data shows that our quality yields better health outcomes and a lower total cost of care,” she wrote. “Sutter’s quality of care is nationally recognized, with the majority of our hospitals and facilities outperforming state and national averages in nearly every measure of quality.”
Still, under the terms of , Sutter agreed to end a host of practices that Becerra, who now heads the U.S. Department of Health and Human Services, alleged unfairly stifled competition. Among other conditions, the settlement also requires Sutter to limit what it charges patients for out-of-network services and end its all-or-nothing contracting deals with payers, which demanded that an insurer that wanted to include any one of the Sutter hospitals or clinics in its network must include all of them.
Sutter has earned an average 42% annual profit margin over the past decade from medical treatments paid for by commercial insurers like the plaintiff companies, according to a recent analysis by Glenn Melnick, a health care economist at the University of Southern California.
Sutter also faces a second federal class-action lawsuit alleging anti-competitive behavior. But while Sutter remains in the crosshairs, its practices are not unique. Experts say negotiating tactics including all-or-nothing contracts and anti-tiering provisions have become widespread among hospital systems nationwide.
“Any system could change their practices tomorrow. If we have to wait for the courts to force them to not use anti-competitive practices, that’s really disappointing,” said Elizabeth Mitchell, CEO of the Purchaser Business Group on Health, which represents employers that buy insurance coverage for their workers.
“What the Sutter case proves is that the people who pay for and receive care can achieve accountability from the health care system. But it shouldn’t be that hard.”
This story was produced by KHNô (Kaiser Health News), a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programsô atô ô (Kaiser Family Foundation).ô KFF is an endowed nonprofit organization providing information on health issues to the nation.
µÍºÇ¨û§ØŸl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/after-18-months-sutter-antitrust-settlement-finally-poised-for-formal-approval/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1347246&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>