“Everyone in the very short line was a woman,” said Steiner, 70.
Her observation reflects a national reality: More women than men are getting covid vaccines, even as of the disease. KHN examined vaccination dashboards for all 50 states and the District of Columbia in early April and found that each of the 38 that listed gender breakdowns showed more women had received shots than men.
Public health experts cited many reasons for the difference, including that women make up three-quarters of the workforce in health care and education, sectors prioritized for initial vaccines. Women’s also mean that older people in the first rounds of vaccine eligibility were more likely to be female. But as eligibility expands to all adults, the gap has continued. Experts point to women’s roles as caregivers and their greater likelihood to seek out preventive health care in general as contributing factors.
In Steiner’s case, her daughter spent hours on the phone and computer, scoping out and setting up vaccine appointments for five relatives. “In my family, the women are about a million times more proactive” about getting a covid vaccine, Steiner said. “The females in families are often the ones who are more proactive about the health of the family.”
As of early April, statistics showed the vaccine breakdown between women and men was generally close to 60% and 40% — women made up 58% of those vaccinated in Alabama and 57% in Florida, for example.
States don’t measure vaccinations by gender uniformly, though. Some break down the statistics by total vaccine doses, for example, while others report people who have gotten at least one dose. Some states also have a separate category for nonbinary people or those whose gender is unknown.
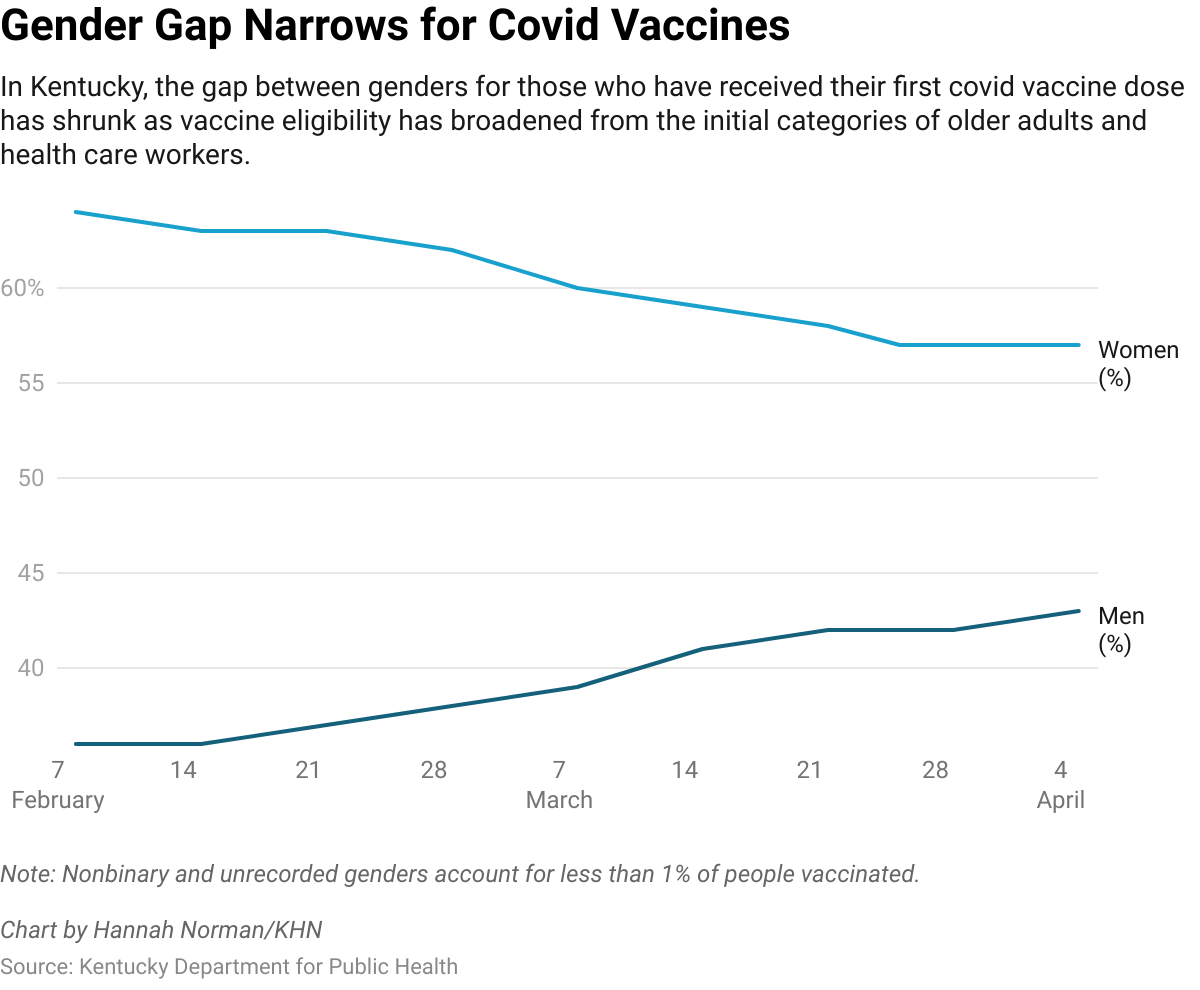
A handful of states report gender vaccination statistics over time. That data shows the gap has narrowed but hasn’t disappeared as vaccine eligibility has expanded beyond people in long-term care and health care workers.
, for instance, 64% of residents who had received at least one dose of vaccine by early February were women and 36% were men. As of early April, the stats had shifted to 57% women and 43% men.
— one of the states furthest along in rolling out the vaccines, of the population fully vaccinated — the gap has narrowed from 30 percentage points (65% women and 35% men) the week of Dec. 13 to 18 points (59% women and 41% men) the week of March 21.
A few states break the numbers down by age as well as gender, revealing that the male-female difference persists across age groups. , for example, the gender breakdown of vaccine recipients as of April 4 was slightly wider for younger people: 61% of vaccinated people ages 25-34 were women compared with 57% female for age 65 and older.
Dr. , a professor at the medical school at Washington University in St. Louis, said women of all age groups, races and ethnicities generally use health services more than men — which is one reason they live longer.
, an assistant professor who specializes in medical geography at the University of North Carolina-Chapel Hill, said it’s often women who manage medical appointments for their households so they may be more familiar with navigating health systems.
Decades of research have documented how and why men are less likely to seek care. A 2019 in the American Journal of Men’s Health, for example, examined health care use in religious heterosexual men and concluded masculine norms — such as a perception that they are supposed to be tough — were the main reason many men avoided seeking care.
Attitudes about the covid pandemic and the vaccines also affect who gets the shots.
Dr. , director of public health administration and policy at the University of Minnesota, said women have been more likely to lose jobs during the pandemic, and in many cases bear the brunt of teaching and caring for children at home.
“Women are ready for this to be done even more than men are,” Wurtz said.
Political attitudes, too, play a part in people’s views on coping with the pandemic, experts said. A found that among both Democrats and Republicans, women were more likely to say they took precautions to avoid covid, such as always practicing physical distancing and wearing masks indoors when they couldn’t stay 6 feet apart from others.
In a by KFF, 29% of Republicans and 5% of Democrats said they definitely would not get the shot.
Paul Niehaus IV of St. Louis, who described himself as an independent libertarian with conservative leanings, said he won’t get a covid vaccine. He said the federal government, along with Big Tech and Big Pharma, are pushing an experimental medicine that is not fully approved by the Food and Drug Administration, and he doesn’t trust those institutions.
“This is a freedom issue. This is a civil liberties issue,” said Niehaus, a 34-year-old self-employed musician. “My motto is ‘Let people choose.’”
Steiner, who plans to retire at the end of the month from editing a magazine for the Catholic Health Association, said she was eager to be vaccinated. She has an immune disorder that puts her at high risk for severe illness from covid and hasn’t seen some of her grandchildren in a year and a half.
But she said some of the men in her life were willing to wait longer for the shots, and a few nephews haven’t wanted them. She said her brother, 65, received the one-shot Johnson & Johnson vaccine in early April after her daughter made it easy by arranging it for him.
Steiner, who has now received both doses of the Moderna vaccine, said she doesn’t regret taking the more difficult step of traveling five hours round trip to get her first shot in February. (She was able to find a closer location for her second dose.)
“It’s for my safety, for my kids’ safety, for my neighbors’ safety, for the people who go to my church’s safety,” she said. “I really don’t understand the resistance.”
Ńîąóĺú´«Ă˝Ň•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/chinese/public-health/gender-vaccine-gap-more-women-than-men-vaccinated-against-covid/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1288362&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>That’s the challenge President Joe Biden has put forward with his bold proposal to spend $400 billion over eight years on home and community-based services, a major part of his $2 trillion infrastructure plan.
It’s a “historic and profound” opportunity to build a stronger framework of services surrounding vulnerable people who need considerable ongoing assistance, said Ai-jen Poo, director of Caring Across Generations, a national group advocating for older adults, individuals with disabilities, families and caregivers.
It comes as the coronavirus pandemic has wreaked havoc in nursing homes, assisted living facilities and group homes, killing more than 174,000 people and triggering awareness of the need for more long-term care options.
“There’s a much greater understanding now that it is not a good thing to be stuck in long-term care institutions” and that community-based care is an “essential alternative, which the vast majority of people would prefer,” said Ari Ne’eman, senior research associate at Harvard Law School’s Project on Disability.
“The systems we do have are crumbling” due to underfunding and understaffing, and “there has never been a greater opportunity for change than now,” said Katie Smith Sloan, president of LeadingAge, at a recent press conference where the president’s proposal was discussed. LeadingAge is a national association of more than 5,000 nonprofit nursing homes, assisted living centers, senior living communities and home care providers.
But prospects for the president’s proposal are uncertain. Republicans and argue that much of what the proposed American Jobs Plan contains, including the emphasis on home-based care, .
“Though this [proposal] is a necessary step to strengthen our long-term care system, politically it will be a challenge,” suggested Joseph Gaugler, a professor at the University of Minnesota’s School of Public Health, who studies long-term care.
Even advocates acknowledge the proposal doesn’t address the full extent of care needed by the nation’s rapidly growing older population. In particular, middle-income seniors won’t qualify directly for programs that would be expanded. They would, however, benefit from a larger, better paid, better trained workforce of aides that help people in their homes — one of the plan’s objectives.
“This [plan] isn’t everything that’s needed, not by any step of the imagination,” Poo said. “What we really want to get to is universal access to long-term care. But that will be a multistep process.”
Understanding what’s at stake is essential as communities across the country and Congress begin discussing Biden’s proposal.
The services in question. Home and community-based services help people who need significant assistance live at home as opposed to nursing homes or group homes.
Services can include home visits from nurses or occupational therapists; assistance with personal care such as eating or bathing; help from case managers; attendance at adult day centers; help with cooking, cleaning and other chores; transportation; and home repairs and modifications. It can also help pay for durable medical equipment such as wheelchairs or oxygen tanks.
The need. At some point, 70% of older adults will require help with dressing, hygiene, moving around, managing finances, taking medications, cooking, housekeeping and other , usually for two to four years. As the nation’s aging population expands to 74 million in 2030 (the year all baby boomers will have entered older age), that need will expand exponentially.
Younger adults and children with conditions such as cerebral palsy, blindness or intellectual disabilities can similarly require significant assistance.
The burden on families. Currently, 53 million family members provide most of the care that vulnerable seniors and people with disabilities require — without being paid and often at significant financial and emotional cost. According to AARP, family caregivers on average devote about 24 hours a week, to helping loved ones and spend around $7,000 out-of-pocket.
This reflects a sobering reality: Long-term care services are simply too expensive for most individuals and families. According to a survey last year by Genworth, a financial services firm, the hourly cost for a home health aide averages $24. Annually, assisted living centers charge an average $51,600, while a semiprivate room in a nursing home goes for $93,075.
Medicare limitations. Many people assume that Medicare — the nation’s health program for 61 million older adults and people with severe disabilities — will pay for long-term care, including home-based services. But Medicare coverage is extremely limited.
In the community, Medicare covers home health only for older adults and people with severe disabilities who are homebound and need skilled services from nurses and therapists. It does not pay for 24-hour care or homemakers or routinely cover care from personal aides. In 2018, about 3.4 million Medicare members received home health services.
In nursing homes, Medicare pays only for rehabilitation services for a maximum of 100 days. It does not provide support for long-term stays in nursing homes or assisted living facilities.
Medicaid options. Medicaid — the federal-state health program for 72 million children and adults in low-income households — can be an alternative, but financial eligibility standards are strict and only people with meager incomes and assets qualify.
Medicaid supports two types of long-term care: home and community-based services and those provided in institutions such as nursing homes. But only care in institutions is mandated by the federal government. Home and community-based services are provided at the discretion of the states.
Although all states offer home and community-based services of some kind, there’s enormous variation in the types of services offered, who is served (states can set caps on enrollment) and state spending. Generally, people need to be frail enough to need nursing home care to qualify.
Nationally, 57% of Medicaid’s long-term care budget goes to home and community-based services — $92 billion in the 2018 federal budget year. But half of states still spend twice as much on institutional care as they do on community-based care. And 41 states have waiting lists, totaling nearly 820,000 people, with an average wait of 39 months.
Based on the best information available, between 4 million and 5 million people receive Medicaid-funded home and community-based services — a fraction of those who need care.
Workforce issues. Biden’s proposal doesn’t specify how $400 billion in additional funding would be spent, beyond stating that access to home and community-based care would be expanded and caregivers would receive “a long-overdue raise, stronger benefits, and an opportunity to organize or join a union.”
Caregivers, including nursing assistants and home health and personal care aides, earn $12 an hour, on average. Most are women of color; about one-third of those working for agencies don’t receive health insurance from their employers.
By the end of this decade, an extra 1 million workers will be needed for home-based care — a number of experts believe will be difficult, if not impossible, to reach given poor pay and working conditions.
“We have a choice to keep these poverty-wage jobs or make them good jobs that allow people to take pride in their work while taking care of their families,” said Poo of Caring Across Generations.
Next steps. Biden’s plan leaves out many details. For example: What portion of funding should go to strengthening the workforce? What portion should be devoted to eliminating waiting lists? What amount should be spent on expanding services?
How will inequities of the current system — for instance, the lack of accessible services in rural counties or for people with dementia — be addressed? “We want to see funding to states tied to addressing those inequities,” said Amber Christ, directing attorney of the health team at Justice in Aging, an advocacy organization.
Meanwhile, supporters of the plan suggest it could be just the opening of a major effort to shore up other parts of the safety net. “There are huge gaps in the system for middle-income families that need to be addressed,” said David Certner, AARP’s legislative counsel.
Reforms that should be considered include tax credits for caregivers, expanding Medicare’s home health benefit and removing the requirement that people receiving Medicare home health be homebound, said Christ of Justice in Aging.
”We should be looking more broadly at potential solutions that reach people who have some resources but not enough to pay for these services as well,” she said.
Ńîąóĺú´«Ă˝Ň•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/chinese/aging/biden-seeks-400-billion-to-buttress-long-term-care-a-look-at-whats-at-stake/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1289177&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>