“I really wanted to take control over how I left this world,” said the 61-year-old who lives in Lancaster. “I decided that this was an option for me.”
Dying with medical assistance wasn’t an option when Milano learned in early 2023 that her disease was incurable. At that point, she would have had to travel to Switzerland — or live in the District of Columbia or one of the .
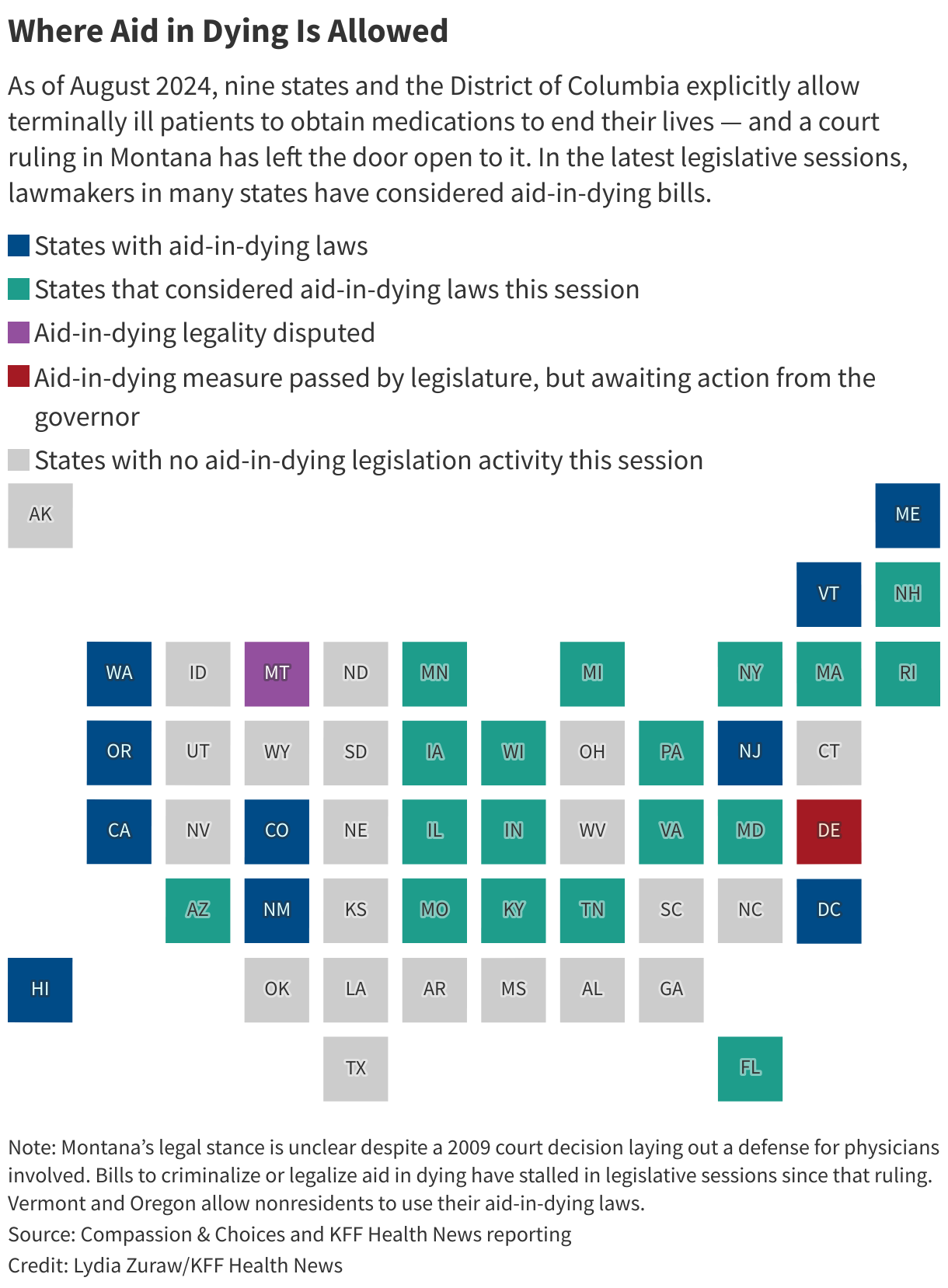
But Vermont lifted its residency requirement in May 2023, followed by Oregon two months later. (Montana effectively allows aid in dying through a 2009 court decision, but that ruling doesn’t spell out rules around residency. And though New York and legislation that would allow out-of-staters to secure aid in dying, neither provision passed.)
Despite the limited options and the challenges — such as finding doctors in a new state, figuring out where to die, and traveling when too sick to walk to the next room, let alone climb into a car — dozens have made the trek to the two states that have opened their doors to terminally ill nonresidents seeking aid in dying.
At least 26 people have traveled to Vermont to die, representing nearly 25% of the reported assisted deaths in the state from May 2023 through this June, according to the Vermont Department of Health. In Oregon, 23 out-of-state residents died using medical assistance in 2023, just over 6% of the state total, according to the .
Oncologist Charles Blanke, whose clinic in Portland is devoted to end-of-life care, said he thinks that Oregon’s total is likely an undercount and he expects the numbers to grow. Over the past year, he said, he’s seen two to four out-of-state patients a week — about one-quarter of his practice — and fielded calls from across the U.S., including New York, the Carolinas, Florida, and “tons from Texas.” But just because patients are willing to travel doesn’t mean it’s easy or that they get their desired outcome.
“The law is pretty strict about what has to be done,” Blanke said.
As in other states that allow what some call physician-assisted death or assisted suicide, Oregon and Vermont require patients to be assessed by two doctors. Patients must have less than six months to live, be mentally and cognitively sound, and be physically able to ingest the drugs to end their lives. Charts and records must be reviewed in the state; neglecting to do so constitutes practicing medicine out of state, which violates medical licensing requirements. For the same reason, the patients must be in the state for the initial exam, when they request the drugs, and when they ingest them.
State legislatures impose those restrictions as safeguards — to balance the rights of patients seeking aid in dying with a legislative imperative not to pass laws that are harmful to anyone, said Peg Sandeen, CEO of the group . Like many aid-in-dying advocates, however, she said such rules create undue burdens for people who are already suffering.
Diana Barnard, a Vermont palliative care physician, said some patients cannot even come for their appointments. “They end up being sick or not feeling like traveling, so there’s rescheduling involved,” she said. “It’s asking people to use a significant part of their energy to come here when they really deserve to have the option closer to home.”
Those opposed to aid in dying include that say taking a life is immoral, and who argue their job is to make people more comfortable at the end of life, not to end the life itself.
Anthropologist , who interviewed dozens of terminally ill patients while researching her 2022 book, “,” said she doesn’t expect federal legislation to settle the issue anytime soon. As the Supreme Court did with abortion in 2022, it ruled assisted dying to be a states’ rights issue in 1997.
During the 2023-24 legislative sessions, (including Milano’s home state of Pennsylvania) considered aid-in-dying legislation, according to the advocacy group . Delaware was the sole state to , but the governor has yet to act on it.

Sandeen said that many states initially pass restrictive laws — requiring 21-day wait times and psychiatric evaluations, for instance — only to eventually repeal provisions that prove unduly onerous. That makes her optimistic that more states will eventually follow Vermont and Oregon, she said.
Milano would have preferred to travel to neighboring New Jersey, where aid in dying has been legal since 2019, but its residency requirement made that a nonstarter. And though Oregon has more providers than the largely rural state of Vermont, Milano opted for the nine-hour car ride to Burlington because it was less physically and financially draining than a cross-country trip.
The logistics were key because Milano knew she’d have to return. When she traveled to Vermont in May 2023 with her husband and her brother, she wasn’t near death. She figured that the next time she was in Vermont, it would be to request the medication. Then she’d have to wait 15 days to receive it.
The waiting period is standard to ensure that a person has what Barnard calls “thoughtful time to contemplate the decision,” although she said most have done that long before. Some states have shortened the period or, like Oregon, have a waiver option.
That waiting period can be hard on patients, on top of being away from their health care team, home, and family. Blanke said he has seen as many as 25 relatives attend the death of an Oregon resident, but out-of-staters usually bring only one person. And while finding a place to die can be a problem for Oregonians who are in care homes or hospitals that prohibit aid in dying, it’s especially challenging for nonresidents.
When Oregon lifted its residency requirement, Blanke advertised on Craigslist and used the results to compile a list of short-term accommodations, including Airbnbs, willing to allow patients to die there. Nonprofits in states with aid-in-dying laws also maintain such lists, Sandeen said.
Milano hasn’t gotten to the point where she needs to find a place to take the meds and end her life. In fact, because she had a relatively healthy year after her first trip to Vermont, she let her six-month approval period lapse.
In June, though, she headed back to open another six-month window. This time, she went with a girlfriend who has a camper van. They drove six hours to cross the state border, before sitting in a parking lot where Milano had a Zoom appointment with her doctors rather than driving three more hours to Burlington to meet in person.
“I don’t know if they do GPS tracking or IP address kind of stuff, but I would have been afraid not to be honest,” she said.
That’s not all that scares her. She worries she’ll be too sick to return to Vermont when she is ready to die. And, even if she can get there, she wonders whether she’ll have the courage to take the medication. About one-third of people approved for assisted death don’t follow through, Blanke said. For them, it’s often enough to know they have the meds — the control — to end their lives when they want.
Milano said she is grateful she has that power now while she’s still healthy enough to travel and enjoy life. “I just wish more people had the option,” she said.

This <a target="_blank" href="/rural-health/aid-in-dying-travel-medical-tourism-vermont-oregon-state-legislation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1899194&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>In more than 4,200 comments, readers shared their struggles in caring for spouses, older parents, and grandparents. They expressed anxieties about getting older themselves and needing help to stay at home or in institutions like nursing homes or assisted living facilities.
Many suggested changes to U.S. policy, like expanding the government’s payments for care and allowing more immigrants to stay in the country to help meet the demand for workers. Some even said they would rather end their lives than become a financial burden to their children.
Many readers blamed the predominantly for-profit nature of American medicine and the long-term care industry for depleting the financial resources of older people, leaving the federal-state Medicaid programs to take care of them once they were destitute.
“It is incorrect to say the money isn’t there to pay for elder care,” , 72, a retired financial controller in Placitas, New Mexico, commented. “It’s there, in the form of profits that accrue to the owners of these facilities.”
“It is a system of wealth transference from the middle class and the poor to the owners of for-profit medical care, including hospitals and the long-term care facilities outlined in this article, underwritten by the government,” he added.
Other readers pointed to insurance policies that, despite limitations, had helped them pay for services. And some relayed their concerns that Americans were not saving enough and were unprepared to take care of themselves as they aged.
What Other Nations Provide
Other countries’ treatment of their older citizens was repeatedly mentioned. Readers contrasted the care they observed older people receiving in foreign countries with the treatment in the United States, which as a portion of its gross domestic product than do most wealthy nations.
Marsha Moyer, 75, a retired teaching assistant in Memphis, Tennessee, said she spent 12 years as a caregiver for her parents in San Diego County and an additional six for her husband. While they had advantages many don’t, Moyer said, “it was a long, lonely job, a sad job, an uphill climb.”
By contrast, her sister-in-law’s mother lived to 103 in a “fully funded, lovely elder care home” in Denmark during her last five years. “My sister-in-law didn’t have to choose between her own life, her career, and helping her healthy but very old mother,” Moyer said. “She could have both. I had to choose.”

Birgit Rosenberg, 58, a software developer in Southampton, Pennsylvania, said her mother had end-stage dementia and had been in a nursing home in Germany for more than two years. “The cost for her absolutely excellent care in a cheerful, clean facility is her pittance of Social Security, about $180 a month,” . “A friend recently had to put her mother into a nursing home here in the U.S. Twice, when visiting, she has found her mother on the floor in her room, where she had been for who knows how long.”
Brad and Carol Burns moved from Fort Worth, Texas, in 2019 to Chapala, Jalisco, in Mexico, dumping their $650-a-month long-term care policy because care is so much more affordable south of the border. Brad, 63, a retired pharmaceutical researcher, said his mother lived just a few miles away in a memory care facility that costs $2,050 a month, which she can afford with her Social Security payments and an annuity. She is receiving “amazing” care, .
“As a reminder, most people in Mexico cannot afford the care we find affordable and that makes me sad,” he said. “But their care for us is amazing, all health care, here, actually. At her home, they address her as Mom or Barbarita, little Barbara.”
Insurance Policies Debated
Many, many readers said they could relate to problems with , and their soaring costs. Some who hold such policies said they provided comfort for a possible worst-case scenario while others castigated insurers for making it difficult to access benefits.
“They really make you work for the money, and you’d better have someone available who can call them and work on the endless and ever-changing paperwork,” , 62, a technical writer in Fancy Gap, Virginia.
Derek Sippel, 47, a registered nurse in Naples, Florida, cited the $11,000 monthly cost of his mother’s nursing home care for dementia as the reason he bought a policy. He pays about $195 a month with a lifetime benefit of $350,000. “I may never need to use the benefit[s], but it makes me feel better knowing that I have it if I need it,” he said in his comment. He said he could not make that kind of money by investing on his own.
“It’s the risk you take with any kind of insurance,” he said. “I don’t want to be a burden on anyone.”
Pleas for More Immigrant Workers
One solution that readers proposed was to increase the number of immigrants allowed into the country to help address the chronic shortage of long-term care workers. Larry Cretan, 73, a retired bank executive in Woodside, California, said that over time, his parents had six caretakers who were immigrants. “There is no magic bullet,” , “but one obvious step ŌĆö hello, people ŌĆö we need more immigrants! Who do you think does most of this work?”
Victoria Raab, 67, a retired copy editor in New York, said that many older Americans must use paid help because their grown children live far away. Her parents and some of their peers rely on immigrants from the Philippines and Eritrea, , “working loosely within the margins of labor regulations.”
“These exemplary populations should be able to fill caretaker roles transparently in exchange for citizenship because they are an obvious and invaluable asset to a difficult profession that lacks American workers of their skill and positive cultural attitudes toward the elderly,” Raab said.
Federal Fixes Sought
Other readers called for the federal government to create a comprehensive, national long-term care system, as some other countries have. In the United States, federal and state programs that finance long-term care are mainly available only to the very poor. For middle-class families, sustained subsidies for home care, for example, are fairly nonexistent.
“I am a geriatric nurse practitioner in New York and have seen this story time and time again,” . “My patients are shocked when we review the options and its costs. Medicaid can’t be the only option to pay for long-term care. Congress needs to act to establish a better system for middle-class Americans to finance long-term care.”

John Reeder, 76, a retired federal economist in Arlington, Virginia, “from birth to senior care in which we all pay and profit-making [is] removed.”
Other readers, however, argued that people needed to take more responsibility by preparing for the expense of old age.
Mark Dennen, 69, in West Harwich, Massachusetts, more rather than expect taxpayers to bail them out. “For too many, the answer is, ŌĆśHow can we hide assets and make the government pay?’ That is just another way of saying, ŌĆśHow can I make somebody else pay my bills?’” he said, adding, “We don’t need the latest phone/car/clothes, but we will need long-term care. Choices.”
Questioning the Value of Life-Prolonging Procedures
A number of readers condemned the country’s medical culture for pushing expensive surgeries and other procedures that do little to improve the quality of people’s few remaining years.
Thomas Thuene, 60, a consultant in Boston’s Roslindale neighborhood, a friend’s mother who had heart failure was repeatedly sent from the elder care facility where she lived to the hospital and back, via ambulance. “There was no arguing with the care facility,” he said. “However, the moment all her money was gone, the facility gently nudged my friend to think of end-of-life care for his mother. It seems the financial ruin is baked into the system.”
Joan Chambers, 69, an architectural draftsperson in Southold, New York, during a hospitalization on a cardiac unit she observed many fellow patients “bedridden with empty eyes,” awaiting implants of stents and pacemakers.
“I realized then and there that we are not patients, we are commodities,” she said. “Most of us will die from heart failure. It will take courage for a family member to refuse a ŌĆśsimple’ procedure that will keep a loved one’s heart beating for a few more years, but we have to stop this cruelty.
“We have to remember that even though we are grateful to our health care professionals, they are not our friends. They are our employees and we can say no.”
One physician, James Sullivan, 64, in Cataumet, a neighborhood of Bourne, Massachusetts, hospitalization and other extraordinary measures if he suffered from dementia. “We spend billions of dollars, and a lot of heartache, treating demented people for pneumonia, urinary tract infections, cancers, things that are going to kill them sooner or later, for no meaningful benefit,” Sullivan said. “I would not want my son to spend his good years, and money, helping to maintain me alive if I don’t even know what’s going on,” he said.
Considering ŌĆśAssisted Dying’
Others went further, declaring they would rather arrange for their own deaths than suffer in greatly diminished capacity. “My long-term care plan is simple,” , 65, a library assistant in St. Louis. “When the money runs out, I will take myself out of the picture.” Clodfelter said she helped care for her mother until her death at 101. “I’ve seen extreme old age,” she said, “and I’m not interested in going there.”
Some suggested that medically assisted death should be a more widely available option in a country that takes such poor care of its elderly. , 76, of Sunnyvale, California, said: “If we can’t manage to provide assisted living to our fellow Americans, could we at least offer assisted dying? At least some of us would see it as a desirable solution.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/dying-broke-reader-reaction-long-term-care-crisis/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1785264&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>California’s original law allowing terminally ill adults to obtain prescriptions for life-ending drugs was passed in 2016. Advocates say the that took effect last year removes crucial safeguards and violates the U.S. Constitution and the Americans with Disabilities Act.
Plaintiffs in the federal lawsuit, which was filed in Los Angeles County, argue that life-ending drugs are more likely to be used by people with disabilities and racial and ethnic minorities because those groups to receive proper medical and mental health care. The advocates fear that vulnerable people could be pressured into taking their lives by family members or caretakers or feel pressure themselves because they don’t want to be a burden.
The lawsuit contends that California’s approach, known as the End of Life Option Act, harks back to the discredited practice of eugenics, which once sought to keep people with disabilities and other minority groups from reproducing.
The system “steers people with terminal disabilities away from necessary mental health care, medical care, and disability supports, and towards death by suicide under the guise of ŌĆśmercy’ and ŌĆśdignity’ in dying,” the suit argues. The terminal disease required for assistance is, by definition, a disability under the Americans with Disabilities Act, it says.
Proponents of the law rejected those claims. “We will do everything possible to ensure the law remains in effect,” said Kevin Díaz, chief legal advocacy officer for Compassion & Choices, a group that backed the California laws, in a statement. Diaz said there was for “medical aid in dying for terminally ill adults, who are destined to die, and just want to have the option to die peacefully, rather than with needless suffering.”
Sean Crowley, a spokesperson for the group, pointed to of the practice in Oregon and the Netherlands that found “no evidence of heightened risk” for vulnerable groups.
Michael Bien, an attorney for the plaintiffs, said the law violates constitutional equal protection and due process safeguards designed to protect people from discrimination and exclusion. Bien is one of the attorneys who sued on behalf of the United Spinal Association, which has at least 60,000 members with spinal cord injuries or who use wheelchairs, including 5,000 in California; , which opposes physician-assisted death; the Institute for Patients’ Rights, which advocates for those at the end of life facing health care disparities; and Communities Actively Living Independent & Free, an independent living center in Los Angeles County.
Bien pointed to statistics showing inequities in infant and maternal mortality, and covid-19 deaths.
“This is how our system works, and end-of-life care has the exact same problems,” Bien said.

People who choose to use drugs supplied by a doctor to kill themselves may not realize they could instead , potentially including sedation that can render them unconscious, said Ingrid Tischer, one of two individual plaintiffs in the lawsuit.
“It really does create two classes of people” based on whether they are perceived to be terminally ill, said the 57-year-old Berkeley resident. “One side gets [suicide] prevention, one side gets a [life-ending] prescription. And that is discriminatory.”
Tischer was born with a type of muscular dystrophy, a progressive disease that now makes it difficult for her to breathe and requires her to use a walker or a wheelchair.
“I want the care that people get at the end of life, including my own, to be much better,” she said. “And I don’t want assisted suicide to become the new American way of death.”
California is one of 10 states, along with Washington, D.C., that have so-called aid-in-dying laws. The others are Colorado, Hawaii, Maine, Montana, New Jersey, New Mexico, Oregon, Vermont, and Washington.
Bien said his clients were looking for a way to challenge the laws and settled on California’s 2022 statute because it removed safeguards in the original law.
reduced the minimum waiting period required between the time patients must make two oral requests for medication from 15 days to 48 hours. The suit notes that, by contrast, California has a 10-day cooling-off period between buying a gun and taking possession of it. The law also eliminated requiring patients to make a written attestation within 48 hours before taking life-ending medication.
Proponents of the revised law said those safeguards had and that other protections remain in the statute. Compassion & Choices, which advocates for assisted death laws, cited that found 21% of people died or became too ill to proceed with the steps. Supporters of the law said they weren’t aware of any abuse or coercion.
The suit argues that people who could live indefinitely with proper medical care can be considered terminally ill and thus eligible for the drugs if they likely would die within six months without such care. That, it says, could include diabetes patients who refuse insulin or people with kidney disorders who refuse dialysis.
Bien cited who wrote in a medical journal that she had steered two patients with anorexia to take prescribed life-ending drugs. Compassion & Choices said .
Even doctors unwilling to assist patients in killing themselves are required under California’s law to document the patient’s request, which still counts as the first of two required spoken requests. Christian Medical & Dental Association sued over that requirement and a federal in September. The state is appealing the ruling.
The California Attorney General’s Office had no immediate comment on the lawsuit, and the law’s author, Democratic state Sen. Susan Talamantes Eggman, did not immediately respond to requests for comment.
This article was produced by čŅ╣¾Õ·┤½├ĮęĢŅl Health News, which publishes , an editorially independent service of the .╠²
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/california-physician-assisted-death-disability-rights-lawsuit/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1680934&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>After decades of deliberations involving physicians, bioethicists, attorneys, and theologians, a U.S. presidential commission in 1981 settled on a scientifically derived dividing line between life and death that has endured, more or less, ever since: A person was considered dead when the entire brain ŌĆö including the brainstem, its most primitive portion ŌĆö was no longer functioning, even if other vital functions could be maintained indefinitely through artificial life support.
In the decades since, the committee’s criteria have served as a foundation for laws in most states adopting brain death as a standard for legal death.
Now, with the overturning of Roe v. Wade and dozens of states rushing to impose abortion restrictions, American society is engaged in a chaotic race to define the other pole of human existence: When exactly does human life begin? At conception, the hint of a heartbeat, a first breath, the ability to survive outside the womb with the help of the latest technology?
That we’ve been able to devise and apply uniform clinical standards for when life ends, but not when it begins, is due largely to the legal and political maelstrom around abortion. And in the two months since the U.S. Supreme Court issued its opinion in Dobbs v. Jackson Women’s Health Organization, eliminating a long-standing federal right to abortion, state legislators are eagerly bounding into that void, looking to codify into law assorted definitions of life that carry profound repercussions for abortion rights, birth control, and assisted reproduction, as well as civil and criminal law.
“The court said that when life begins is up to whoever is running your state ŌĆö whether they are wrong or not, or you agree with them or not,” said Mary Ziegler, a law professor at the University of California-Davis who has written several books on the history of abortion.
Unlike the debate over death, which delved into exquisite medical and scientific detail, the legislative scramble to determine when life’s building blocks reach a threshold that warrants government protection as human life has generally ignored the input of mainstream medical professionals.
Instead, red states across much of the South and portions of the Midwest are adopting language drafted by elected officials that is informed by conservative Christian doctrine, often with little scientific underpinning.
A handful of Republican-led states, including Arkansas, Kentucky, Missouri, and Oklahoma, have passed laws declaring that life begins at fertilization, a contention that opens the door to a host of pregnancy-related litigation. This includes wrongful death lawsuits brought on behalf of the estate of an embryo by disgruntled ex-partners against physicians and women who end a pregnancy or even miscarry. (One such in Arizona. Another reached the Alabama Supreme Court.)
In Kentucky, the law outlawing abortion uses morally explosive terms to define pregnancy as “the human female reproductive condition of having a living unborn human being within her body throughout the entire embryonic and fetal stages of the unborn child from fertilization to full gestation and childbirth.”
Several other states, including Georgia, have adopted measures equating life with the point at which an embryo’s nascent cardiac activity can be detected by an ultrasound, at around six weeks of gestation. Many such laws mischaracterize the flickering electrical impulses detectible at that stage as a heartbeat, including in Georgia, whose Department of Revenue recently announced that “any unborn child with a detectable human heartbeat” can be claimed as a dependent.
The Supreme Court’s 1973 decision in Roe v. Wade that established a constitutional right to abortion did not define a moment when life begins. The opinion, written by Justice Harry Blackmun, observed that the Constitution does not provide a definition of “person,” though it extends protections to those born or naturalized in the U.S. The court majority made note of the many disparate views among religions and scientists on when life begins, and concluded it was not up to the states to adopt one theory of life.
Instead, Roe intended to balance a pregnant woman’s right to make decisions about her body with a public interest in protecting potential human life. That decision and a key ruling that followed generally recognized a woman’s right to abortion up to the point medical professionals judge a fetus viable to survive outside the uterus, at about 24 weeks of gestation.
In decisively overturning Roe in June, the Supreme Court’s conservative majority drew on legal arguments that have shaped another contentious end-of-life issue. The legal standard employed in Dobbs ŌĆö that there is no right to abortion in the federal Constitution and that states can decide on their own ŌĆö is the same rationale used in 1997 when the Supreme Court said terminally ill people did not have a constitutional right to medically assisted death. That decision, Washington v. Glucksberg, is mentioned 15 times in the majority opinion for Dobbs and a concurrence by Justice Clarence Thomas.
Often, the same groups that have led the fight to outlaw abortion have also challenged medical aid-in-dying laws. Even after Dobbs, so-called right-to-die laws remain far less common than those codifying state abortion rights. Ten states allow physicians to prescribe lethal doses of medicine for terminally ill patients. Doctors are still prohibited from administering the drugs.
James Bopp, general counsel for the National Right to Life Committee who has been central to the efforts to outlaw abortion, said that both abortion and medically assisted death, which he refers to as physician-assisted suicide, endanger society.
“Every individual human life has inherent value and is sacred,” said Bopp. “The government has the duty to protect that life.”
Both issues raise profound societal questions: Can the government keep a patient on life support against his wishes, or force a woman to give birth? Can states bar their own residents from going to other states to end a pregnancy, or prohibit out-of-state patients from coming in to seek medically assisted death? And who gets to decide, particularly if the answer imposes a singular religious viewpoint?
Just as there are legal implications that flow from determining a person’s death, from organ donation to inheritance, the implied rights held by a legally recognized zygote are potentially vast. Will death certificates be issued for every lost pregnancy? Will miscarriages be investigated? When will Social Security numbers be issued? How will census counts be tallied and congressional districts drawn?
Medical professionals and bioethicists caution that both the beginning and end of life are complicated biological processes that are not defined by a single identifiable moment ŌĆö and are ill suited to the political arena.
“Unfortunately, biological occurrences are not events, they are processes,” said David Magnus, director of the Stanford Center for Biomedical Ethics.
Moreover, asking doctors “What is life?” or “What is death?” may miss the point, said Magnus: “Medicine can answer the question ŌĆśWhen does a biological organism cease to exist?’ But they can’t answer the question ŌĆśWhen does a person begin or end?’ because those are metaphysical issues.”
Ben Sarbey, a doctoral candidate in Duke University’s department of philosophy who studies medical ethics, echoed that perspective, recounting the Paradox of the Heap, a thought experiment that involves placing grains of sand one on top of the next. The philosophical quandary is this: At what point do those grains of sand become something more ŌĆö a heap?
“We’re going to have a rough time placing a dividing line that this counts as a person and this does not count as a person,” he said. “Many things count as life ŌĆö a sperm counts as life, a person in a persistent vegetative state counts as life ŌĆö but does that constitute a person that we should be protecting?”
Even as debate over the court’s abortion decision percolates, the 1981 federal statute that grew out of the presidential committee’s findings, the Uniform Determination of Death Act, is also under review. This year, the Uniform Law Commission, a nonpartisan group of legal experts that drafts laws intended for adoption in multiple states, has taken up the work to revisit the definition of death.
The group will consider sharpening the medical standards for brain death in light of advances in the understanding of brain function. And they will look to address lingering questions raised in recent years as families and religious groups have waged heated legal battles over terminating artificial life support for patients with no brain wave activity.
Bopp, with the National Right to Life Committee, is among those serving on advisory panels for the effort, along with an array of doctors, philosophers, and medical ethicists. The concept of “personhood” that infuses the anti-abortion movement’s broader push for fetal rights is expected to be an underlying topic, albeit in mirror image: When does a life form cease being a person?
Magnus, who is also serving on an advisory panel, has no doubt the commission will reach a consensus, a sober resolution rooted in science. What’s less clear, he said, is whether in today’s political environment that updated definition will hold the same sway, an enduring legal standard embraced across states.
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/in-the-rush-to-curtail-abortion-states-adopt-a-jumbled-stew-of-definitions-for-human-life/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1546187&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But after 18 cancer-free months, the disease returned with a vengeance in June 2003. It fractured her bones and invaded her spinal canal, bathing her brain in malignancy.
During the final six months, as she lay on her home hospice bed in constant pain, attached to a morphine drip around-the-clock while losing her eyesight and withering to a skeleton, the idea of ending her suffering by ending her life didn’t even enter into our conversations.
I’ve been thinking a lot about those bleak days while looking into California’s , which allows terminally ill patients with a life expectancy of less than six months to end their lives by taking medications prescribed by a physician. In October, Gov. Gavin Newsom signed a of the law, extending it to January 2031 and loosening some restrictions in the 2015 version that proponents say have become barriers to dying people who wish to avail themselves of the law.
The original law, which remains in effect until Jan. 1, contains numerous safeguards meant to ensure that patients are not being coerced by family members who view them as a burden or a potential financial bonanza.
Under the current law, patients who want to die must make two oral requests for the medications at least 15 days apart. They also must request the drugs in writing, and two doctors must agree the patients are legally eligible. After receiving the medications, patients must confirm their intention to die by signing a form 48 hours before ingesting them.
The patients must take the drugs without assistance, either orally, rectally or through a feeding tube. And physicians can decline to prescribe the death-inducing drugs.
After the law had been in effect for a while, its proponents and practitioners concluded that some safeguards made the option unavailable to certain patients.
Some patients were so sick they died during the 15 days they were required to wait between their first and second requests for the medications. Others were too weak or disoriented to sign the final attestation.
The revised law reduces the 15-day waiting period to just two days and eliminates the final attestation.
It also requires health care facilities to post their aid-in-dying policies online. Doctors who decline to prescribe the drugs ŌĆö whether on principle or because they don’t feel qualified ŌĆö are obliged to document the patient’s request and transfer the record to any other doctor the patient designates.
The most important part of the new law, advocates say, is the shortening of the waiting period.
, an assistant clinical professor specializing in palliative medicine at National Medical Center in Duarte, California, says she’s seen many patients who were afraid to broach the subject of their own death until they were very close to the end.
“By the time they made that first request and then had to wait for those 15 days, they either became completely nondecisional or went into a coma or passed away,” Banerjee says.
Amanda Villegas, 30, of Ontario, California, became an outspoken advocate for updating the law after watching her husband, Chris, die an agonizing death from metastatic bladder cancer in 2019.
When the couple asked about the possibility of a physician-assisted death, Villegas says, staff at the Seventh-day Adventist hospital where Chris was being treated told them, inaccurately, that it was illegal. When he finally made a request for death-inducing drugs, it was too late: He died before the 15-day waiting period was up.
The new law “will open doors for people who might ŌĆ” experience the same roadblocks,” Villegas says. “When you are dying, the last thing you need is to go through bureaucratic barriers to access peace.”


Medical aid in dying straddles the same political fault line as abortion and has long been opposed by many religious institutions and anti-abortion groups. It has also encountered resistance from that claim it belittles the lives of those who are physically dependent on others.
“We object to the whole idea of a state providing a vehicle for people to kill themselves,” says Alexandra Snyder, CEO of the Life Legal Defense Foundation, an anti-abortion nonprofit law firm. The 15-day waiting period, she says, provided an important cooling-off period for patients to reflect on a decision that is irreversible. “Now, any safeguards that were in the law are gone.”
Proponents of the law say they haven’t seen evidence that a patient’s decision to take the life-ending medications has ever been anything other than voluntary.
Though neither version of the law requires a medical professional to be present when a patient takes the drugs, medical standards encourage professional participation in the dying process, says Dr. Lonny Shavelson, chair of the American Clinicians Academy on Medical Aid in Dying. The drugs should be kept at the pharmacy until the patient is ready to ingest them, he says ŌĆö though that doesn’t always happen.
From the time the aid-in-dying law took effect in June 2016 through Dec. 31, 2020, just under two-thirds of the 2,858 people who received prescriptions actually took the medications and died, according to the from the California Department of Public Health. The rest died before they could take the drugs or found other ways to manage their pain and emotional distress.
Most major commercial health plans ŌĆö including Kaiser Permanente, Anthem Blue Cross, Blue Shield of California and Health Net ŌĆö cover aid-in-dying drugs and the related doctor visits, as does Medi-Cal, the government-run health insurance program for people with low incomes.
However, more than 60% of those who take the drugs are on Medicare, which does not cover them. Effective life-ending drug combinations are available for as little as $400.
If you are contemplating aid in dying, here are some resources to learn more about it:
- Compassion & Choices, 1-800-247-7421 or
- The California Department of Public Health, (click “programs”)
- The American Clinicians Academy on Medical Aid in Dying,
- End of Life Choices California, or 1-760-636-8009
Talk to your doctor sooner rather than later if you are considering medically assisted death, in case you’ll need to seek a different physician’s help. If your doctor agrees to help, the law requires that he or she discuss other end-of-life options with you, including hospice and palliative care.
Whatever choice a patient makes, being more open about our mortality is important, says state Sen. Susan Eggman (D-Stockton), the author of the revised aid-in-dying law.
“We should all have more conversations about life and death and what we want and don’t want and what is a peaceful death,” she says. “We are all going to die.”
Leslie and I had plenty of those conversations, until the cancer ultimately robbed her of her mind.
In her final months, she would often sink into a semiconscious state, far out of our reach for days on end. Then, just when we thought she wasn’t coming back, she would suddenly open her eyes and ask for the children. She’d get into her wheelchair and join us at the dinner table.
Those periods, which we called “awakenings,” were a source of great comfort to everyone who loved Leslie ŌĆö but especially to the kids, who were relieved and overjoyed to have their mommy back.
Though I’ll never know for sure, I suspect Leslie would not have wanted to foreclose on such moments.
This story was produced by , which publishes , an editorially independent service of the .
This <a target="_blank" href="/aging/new-california-law-eases-aid-in-dying-process/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1414610&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>After two years of being sick, Heim’s dad got the diagnosis in 2019: stage 4 kidney cancer. His physician offered treatments that might extend his life by months. Instead, the 81-year-old asked the doctor for help dying. Heim said her parents left the appointment in their hometown of Billings with two takeaways: The legality of medically assisted death was questionable in Montana, and her father’s physician didn’t seem willing to risk his career to put that question to the test.
“My parents knew when they left there that was the end of that conversation,” said Heim, now 54. “My dad was upset and mad.”
The day after the appointment, Heim’s mother went grocery shopping. While she was gone, Heim’s dad went to the backyard and fatally shot himself. (Heim asked that her father’s name not be published due to the lingering stigma of suicide.)
About a decade earlier, in 2009, the Montana Supreme Court had, in theory, cracked open the door to sanctioned medically assisted death. The court ruled physicians could if charged with homicide for prescribing life-ending medication.
However, the ruling sidestepped whether terminally ill patients have a constitutional right to that aid. Whether that case made aid in dying legal in Montana has been debated ever since. “There is just no right to medical aid in dying in Montana, at least no right a patient can rely on, like in the other states,” said former state Supreme Court Justice Jim Nelson. “Every time a physician does it, the physician rolls the dice.”
Every session of the biennial Montana state legislature since then, a lawmaker has proposed a bill to formally criminalize physician-assisted death. Those who back the bills say the aid is morally wrong while opponents say criminalizing the practice would be a backstep for patients’ rights. But so far, lawmakers haven’t gained enough support to pass any legislation on the issue, though it has been close. stalled on March 1, on a split vote.
Even the terminology to describe the practice is disputed. Some say it’s “suicide” anytime someone intentionally ends their life. Others say it’s “death with dignity” when choosing to expedite a painful end. Such debates have gone on for decades. But Montana remains the sole state stuck in a legal gray zone, even if the practice can still seem taboo in many states with clear laws. Such continued uncertainty makes it especially hard for Montana patients like Heim’s dad and their doctors to navigate what’s allowed.
“Doctors are risk-averse,” said Dr. , director of the health law program at the University of Nevada-Las Vegas, who helped write clinical aid-in-dying published in the Journal of Palliative Medicine in 2016. “The fear of being sued or prosecuted is still there.”
Despite that, access to medical aid in dying is gaining momentum across the U.S. Outside Montana, eight states and the District of Columbia allow the life-ending aid — six of them since 2014. So far in 2021, legislators in at least have pushed aid-in-dying bills, most seeking to legalize the practice and some seeking to drop barriers to existing aid such as expanding which medical professionals can offer it. Many are repeat legalization efforts with some, like in New York, dating as far back as 1995. Only the Montana bill this year specifically sought to criminalize it.
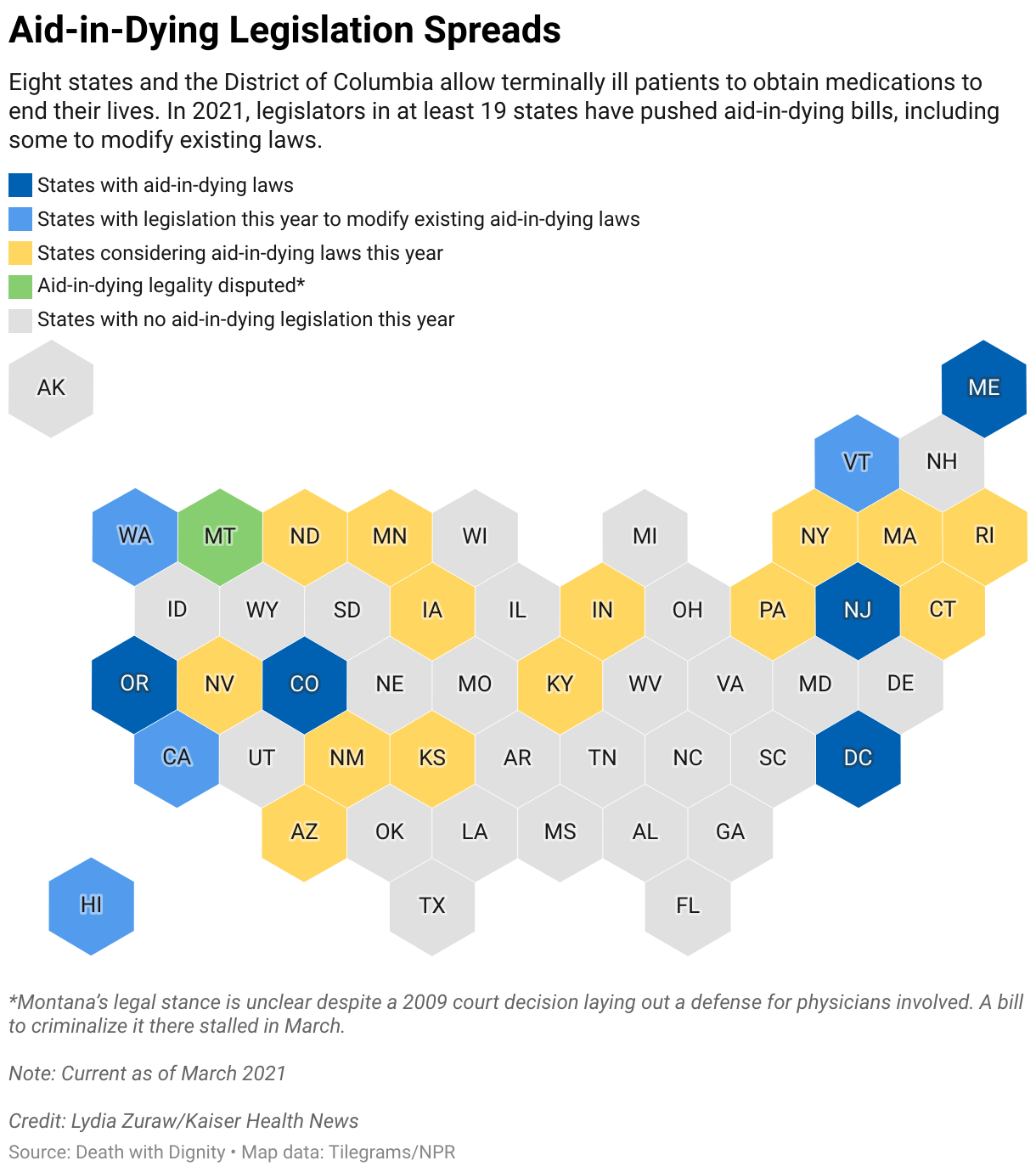
North Dakota considered legislation to legalize medically assisted death for the first time. Rep. , a Democrat from Fargo who proposed the measure after hearing from a cancer patient, said she wasn’t surprised when the bill failed in February in . The state’s medical association said it was “.” Angry voters called Anderson asking why she wanted to kill people.
“But I heard from just as many people that this was a good bill,” Anderson said. “There is momentum to not let this concept go away.”
Back in Montana, now retired state Supreme Court Justice Nelson said he has always regretted joining the majority in the case that allowed the practice because the narrow ruling focused on physicians’ legal defense, not patients’ rights. Having watched a friend die slowly from disease, Nelson, 77, wants the choice himself if ever needed.
Despite — or because of — the court decision, some Montana doctors do today feel that they can accommodate such patient decisions. For example, Dr. , a hospice and palliative care physician, said until she retired from private practice last year she considered patients’ requests for life-ending drugs.
Physicians who help in such cases follow well-established guidelines set by other states, Kirchhoff said. A patient must have six months or less to live — a fact corroborated by a second physician; can’t be clinically depressed; needs to ask for the aid; and be an adult capable of making health care decisions, which is determined by the attending physician. They must also administer the life-ending medication themselves.
“You’re obviously not going to do a case that is vague or nebulous or has family discord,” Kirchhoff said. “The doctors who are prescribing have felt comfortable and that they’re doing the right thing for their patient, alleviating their suffering.” Of her few patients who qualified for a prescription, she said, none actually took the drugs. Kirchhoff noted that, in some cases, getting the prescription seemed to provide comfort to her patients — it was enough knowing they had the option if their illness became unbearable.
For the past six legislative sessions — dating to 2011 — a Montana lawmaker has proposed a bill to clarify that state law doesn’t allow physician-assisted death. Republican Sen. picked up that effort the past two sessions. Glimm said the current status, based on the more than decade-old court decision, sends a mixed message in a state that the Centers for Disease Control and Prevention as having among the nation’s highest suicide rates. Glimm said allowing someone to end their life because of pain from a terminal illness could normalize suicide for people living with depression, which is also a form of pain.
“It’s really hard because I do sympathize with them,” Glimm said. “What it boils down to is, if you’re going to take your own life, then that’s suicide.”
, president and CEO of national nonprofit Compassion & Choices, said the comparison to suicide is frustrating. “People who are seeking medical aid in dying want to live, but they are stricken with a life-ending illness,” she said.
Glimm and his bill’s supporters say that some patients could be pressured into it by family members with something to gain, and doctors could prescribe it more often than they should.
But Callinan, whose group advocates for aid in dying, said that since Oregon first legalized it in 1997, no data has shown any merit to the warnings about abuse and coercion. showed no evidence of heightened risk of abuse within the practice for vulnerable populations such as the elderly. But critics have said states aren’t doing enough to track the issue.

By now, Leslie Mutchler, 60, knows most of the people on all sides of the debate after years of testifying in support of protecting aid in dying. Her dad, Bob Baxter, was a plaintiff in the case that eventually led to the 2009 Montana Supreme Court decision on medically assisted death. After leukemia whittled his body for years, he died in 2008 without the option, the same day a lower court ruled in his favor.
Mutchler said she didn’t understand how complicated the Supreme Court’s ultimate ruling was until her son TJ was diagnosed with terminal metastatic pancreatic cancer in 2016.
He was 36 and lived in Billings, Montana. By then, the 6-foot-5 man had lost 125 pounds off what had been a 240-pound frame. He couldn’t keep food down and needed a feeding tube for medicine and water. TJ Mutchler wanted to have the choice his grandfather never got. But when he went to his physician and asked for aid in dying, the response was it wasn’t legal. Eventually, Mutchler found a doctor to evaluate her son and write the prescriptions for phenobarbital and amitriptyline. TJ took the drugs more than two months later and died.
“People contact me asking how to find someone and it’s difficult,” Mutchler said. “That’s why people end up taking matters into their own hands.” Research into terminally ill populations is limited, but published in 2019 found the risk of someone with cancer taking their own life is four times higher than the general population.

For Roberta King, another one of Baxter’s daughters, the ongoing fight over aid in dying in Montana means she knows every other winter she’ll make the more than 200-mile round trip from her Missoula home to the state capital. King, 58, has testified against all six bills that sought to ban aid in dying following her dad’s case. She memorized a speech about how her dad became so thin after his medicine stopped working that it hurt for him to sit.
“It’s still terrible, you still have to get up there in front of everybody and they know what you’re going to say because it’s the same people doing the same thing,” King said. But skipping a hearing doesn’t feel like an option. “If something were to happen to this and I didn’t try, I would never forgive myself,” she said.
This <a target="_blank" href="/courts/montana-medical-aid-in-dying-legal-gray-zone-reviving-legislation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1277356&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
It can be republished for free.
GOLDEN, Colo. ŌĆĢ The call came the last week of September, when Neil Mahoney could still stagger from his bed to the porch of his mobile home to let out his boisterous yellow Lab, Ryder.
Rodney Diffendaffer, a clinical pharmacist in Longmont, 45 miles away, had left a message.
Your prescription is ready, it said.
Mahoney, a once-rugged outdoorsman now reduced to bones, his belly swollen with incurable cancer, sighed with relief. After months of obstacles, the frail 64-year-old finally had access to lethal drugs under Colorado’s 2016 End of Life Options Act, one of a growing number of U.S. state laws that allow terminally ill patients to obtain medications to end their lives.
Even as an increasing number of U.S. states have legalized aid-in-dying laws, exercising that option is challenging for patients in a country where most large hospital systems have deep religious ties and the religious right is powerful. One in 6 hospital patients is now cared for at a Catholic hospital, according to the Catholic Health Association. Aid-in-dying is a legal right, but desperate patients are often left feeling they are doing something terribly, morally wrong.
Centura Health Corp., the Christian-run hospital where Mahoney sought treatment for his cancer, regards the practice as “intrinsically evil,” citing the ’¼ürm’s governing rules, the Ethical and Religious Directives for Catholic Health Care Services. The hospital has barred its doctors from following the state law. In August, it fired his physician, Dr. Barbara Morris, for consulting with Mahoney with the aim of carrying out his wishes.
As his condition deteriorated over the summer, Mahoney left the lawsuit, with Morris still unable to assist him. She sued the hospital for wrongful dismissal; the case is pending. In December, Centura officials filed a countersuit that says the hospital’s actions are protected by the U.S. and state constitutions’ freedom of religion guarantees.

In opposing the practice, the country’s religious institutions have received support from the Trump administration, which has consistently given providers wide latitude to refuse to participate in medical interventions they object to on religious grounds, though that previously applied primarily to abortion and contraception.

That leaves dying patients like Mahoney feeling abandoned during the most vulnerable time of their lives. When Centura fired Morris for encouraging “a morally unacceptable option,” Mahoney lost both his doctor and the confidence that he would be able to end his life when the suffering became too great.
So the brief message on his phone meant an important victory.
“This way I can say, ŌĆśYes, I can go,’” he said last summer. “I can call them up with a couple days’ notice and do it.”
Legal But Not Accessible
Oregon was out front in permitting aid-in-dying, approving it more than two decades ago. In recent years, District of Columbia have allowed the practice. It’s being considered in others.
Even when the practice is legal, it often isn’t accessible. Some doctors are barred from participating by their employers. Others refuse to do so. In some cases, the drugs themselves may be too expensive. A dose of Seconal, which was once the most commonly prescribed drug for the practice, can run more than $3,000. The government and some private insurers won’t cover it.
One of nine siblings in a close Catholic family, Mahoney seemed an unlikely candidate to test the Colorado law.

Weathered and rangy, with a reddish crew cut and broad hands, he’d never had a major illness or injury despite years of physical labor. For the past five years, he managed planting crews at Welby Gardens, a wholesale nursery near Denver.
“The dahlias have always been one of my favorites,” Mahoney said. “Just because of the flowers, the way those millions of petals can open up. That just still baffles me.”
He lived with Ryder, his 6-year-old golden Lab, and Lakewood, a sleek calico cat.
Mahoney was never comfortable around doctors, said his youngest brother, Patrick Mahoney, 60, who supported his older brother’s efforts to obtain help in planning his death.
“Neil had a long belief that health systems, including physicians, capitalize on those that are ill,” Patrick Mahoney said.


Neil Mahoney started feeling sick last January, then worse in April and May. By mid-June, he couldn’t ignore a bout of stomach cramps, nausea and vomiting that sent him to urgent care.
Doctors ordered a CT scan, which showed multiple masses on his liver and likely in his lymph nodes, plus tumors at the junction of his stomach and esophagus. In July, tests at a local cancer center confirmed the bad news: stage 4 adenocarcinoma, a cancer that forms in the body’s glands.
There’s no cure, the doctor said. Without treatment, Mahoney could expect to live four more months. With chemotherapy, he might make it a little more than a year.
Neil Mahoney immediately asked about medical aid-in-dying. He was among 65% of Colorado voters who supported the law in 2016, and now he expected to use it. The medical oncologist turned him down flat.
Neil Mahoney recalled: “I feel like I got slapped in the face.”

ŌĆśThe Healing Ministry’
Mahoney’s primary care doctor had no qualms about participating. At 65, with 40 years of experience, Morris said that, in her view, medical aid-in-dying should be part of a continuum of care for dying patients.
“We cannot know when a person has reached their limit of suffering,” she said. “Only that person knows.”

But Centura, jointly run by Catholic and Seventh-day Adventist churches, describes its work as “the healing ministry of Christ.” When it became aware of the plans in the works, Centura fired Morris, contending that Morris had violated an employment contract requiring her to abide by its faith-based rules.
Morris immediately lost her malpractice insurance and access to a medical office, leaving her unable to prescribe drugs or provide care for Mahoney ŌĆĢ and 400 geriatric patients.
The lawsuit she and Mahoney filed in August alleged that Centura’s faith-based policy violates both the End of Life Options Act and Colorado laws barring health systems from interfering with medical judgment. It sought to clarify whether Centura could prevent Morris from helping Mahoney as long as he wasn’t on the health system premises.
“We believe it is a morally unacceptable act, regardless of how you couch it, and we are not going to participate in it,” Centura chief executive Peter Banko told Kaiser Health News.
In December, Centura officials hired a Colorado law firm that specializes in religious freedom cases. In its counterclaim, Centura officials are asking a judge to declare that a health care organization cannot be forced to allow its employees to support or carry out provisions of Colorado’s End of Life Options Act.
Mahoney didn’t have the time to let the legal battle play out in the courts. By July, he’d lost 30 pounds from his 185-pound frame. He grew weaker, wrenched with pain from tumors at the junction of his stomach and esophagus.
The Mahoney children had watched their mother, Charlotte Mahoney, endure a slow decline two weeks before her death in 2007 at age 85.
“I did not want to face an agonizing death without any means to help control when and where I will die,” Neil Mahoney told lawyers.
With his own doctor’s hands tied, a desperate Mahoney resorted to a backdoor route to exercise his legal right.

Rodney Diffendaffer, a pharmacist who runs a network that quietly connects terminally ill patients in Colorado with doctors willing to follow the law, reached out after reading about Mahoney’s dilemma.
“It’s his choice to have that drug,” said Diffendaffer, 51, who works at the independently owned . “No one else should even have a say.”
In the past two years, Diffendaffer and his fledgling group, Dying With Dignity of the Rockies, have helped more than 50 terminally ill Coloradans obtain medications to end their lives.
“I have seen the pure torture that people went through,” said Diffendaffer, who grew up on a farm and says dying animals are treated more humanely.
Instead of planning for retirement, I’m planning for death.
Neil Mahoney
Although nearly 4,000 people in the United States have used a medical aid-in-dying law, under-the-radar groups like Diffendaffer’s have emerged to match patients with doctors willing to help ŌĆö but not willing to be included on a public list.
“They don’t want to be labeled ŌĆśDr. Death,’” said Lynne Calkins, a board member for , a volunteer group formed in that state last spring.
The problem grows not just from powerful religious medical centers, but also the loud voice of the religious right in national politics as well as a genuine discomfort among some physicians who are loath to use their skills to end lives rather than save them.
Dr. Ira Byock, founder and chief medical officer at the at Providence St. Joseph Health in Gardena, Calif., has long opposed the practice he calls “hastened death.” He said his objections are based on his understanding of his profession, not on faith.
“I can only say that from my perspective, and that of many non-Catholic practitioners, it is outside the scope of medical practice,” he said. “Ending somebody’s life intentionally is not part of medical practice. It is something else.”
In Vermont, where the practice has been legal since 2013, few doctors outside larger cities such as Burlington are trained to administer the law and few pharmacies are equipped to supply the drugs, said Betsy Walkerman, president of the group .
“The rest of the state is very thin on medical presence,” Walkerman said. “It’s much more difficult.”
In New Jersey, which enacted a law in August, the family of Zeporah “Zebbie” Geller contacted 40 doctors before they found two willing to help. Geller, 80, a retired teacher, had been diagnosed with terminal lung cancer and died on Sept. 30 after ingesting the prescribed medication.

Neil Mahoney’s Choice
Dr. Glenda Weeman, 60, a family physician who operates an independent practice in Longmont, agreed to prescribe aid-in-dying drugs for Mahoney after two exams, which confirmed he met the law’s requirements.
Weeman had prescribed the drugs for only one patient before Mahoney under Colorado’s relatively young law.
“My role is to relieve pain and suffering. That is my job,” Weeman said. “I have to help people understand that there are choices. If you don’t know the choices of how to die, I’m going to help you figure that out.”
By late September, Mahoney had his prescription, which included two anti-nausea drugs and a cocktail of four medications that would induce death. He paid about $575 for it all, out-of-pocket.
Still, he wasn’t sure when ŌĆö or if ŌĆö he’d use them. About a third of people who get the drugs don’t wind up taking them, and Washington show.
“It’s a little spooky,” Mahoney said on Sept. 30, sitting in his small, cluttered mobile home. A green T-shirt hung from his bony shoulders; he’d lost another 20 pounds. Around his neck was a pendant that said DNR: Do not resuscitate.
Mahoney still had a list of things to do. A friend had promised to care for Ryder, the dog. The cat might do OK on her own, though his sister later offered to take her. He wanted to write a will.
“It’s quite a turnaround,” he said quietly. “Instead of planning for retirement, I’m planning for death.”

Over the next few weeks, Neil grew frailer day by day. Patrick Mahoney, who quit his job to help, said that he and another brother, John, took turns sleeping on their brother’s couch.
Neil Mahoney knew he had a window of time where he could take the medicine. If he waited too long, he wouldn’t be able to swallow it. Then he’d lose his chance to make the choice.
On Tuesday, Nov. 5, he decided it was time.
At 9:45 p.m., in bed, surrounded by family, Neil Mahoney took the drugs to halt anxiety and nausea. Minutes later, using a straw, he quickly drank the rest of the medications, dry powders mixed with raspberry-flavored liquid. Then they waited.
“It was perhaps the hardest hour of our lives,” Patrick Mahoney said.
About 10:45, Patrick “felt for his pulse. I put my hand on his chest to check his respiration rate, and then I said, ŌĆśHe’s gone.’”
Reached by email, Barbara Morris was somber about the death of a patient whom the religious teachings of her former employer had prevented her from helping. She has found another place to practice, starting in the new year.
“It was great honor to know Neil both as his doctor and his friend,” she wrote. “Out of respect for his memory, we will continue to advocate for care focused on patient values and wishes.”
This <a target="_blank" href="/aging/when-aid-in-dying-is-legal-but-the-medicine-is-out-of-reach/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1033979&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Centura Health Corp. this week abruptly terminated Dr. Barbara Morris, 65, a geriatrician with 40 years of experience, who had planned to help her patient, Cornelius “Neil” Mahoney, 64, end his life at his home. Mahoney, who has terminal cancer, is eligible to use the state’s law, overwhelmingly approved by Colorado voters in 2016.
The growing number of state aid-in-dying provisions are increasingly coming into conflict with the precepts of faith-based hospitals, which oppose the practice on religious grounds.
Morris’ dismissal presents an early test of state laws. The Trump administration has moved to broaden the latitude of providers to refuse to participate in medical interventions they object to on religious grounds, though that has previously applied primarily to abortion and contraception.
As hospitals across the country have consolidated, are associated with the Roman Catholic Church, according to Definitive Health. That includes hospitals that did not previously have any religious affiliation. Meanwhile, there are 10 U.S. jurisdictions where aid-in-dying has been approved and public support for the option is increasing.
The Aug. 26 firing came days after Morris joined with Mahoney in that alleges that Centura’s faith-based policy violates the law that allows doctors to prescribe lethal drugs to dying patients who want to end their own lives.
Officials at Centura, a system jointly run by Catholic and Seventh-day Adventist churches, told Morris on Monday that she had defied church doctrines that govern her employment.
“I was shellshocked,” Morris said in an exclusive interview with Kaiser Health News. “Because of all the things I expected them to do, that was not in the playbook. Because it seemed so obvious that they can’t do it.”
But in that ask to elevate the case to federal court and invoke the First Amendment in defense of their actions, Centura officials said Morris had violated terms of her physician’s employment agreement and “encouraged an option that she knew was morally unacceptable to her employer.”

For Mahoney, the firing deals yet another setback in his quest to use the law. Mahoney, who in July was given four to 14 months to live, said he watched his mother die a slow, painful death and hopes to avoid that for himself.
“Knowing that I could die at home is huge,” said Mahoney, who has lost 30 pounds since April, even as his belly swelled painfully with fluid as a result of the cancer. “This gets dragged out too long.”
The Trump administration in May approved a so-called that strengthens the rights of hospitals and health workers to refuse to participate in patient care based on religious or moral grounds.
At the same time, more doctors and patients in the country are providing and receiving health care subject to religious restrictions. About 1 in 6 acute care beds nationally is in a hospital that is , said Lois Uttley, a program director for the consumer advocacy group Community Catalyst.
In Colorado, one-third of the state’s hospitals operate under Catholic guidelines.
In a letter hand-delivered to Morris, who has worked for the health care system since 2013, Centura president Vance McLarren said that she had violated the firm’s governing rules, the
“Rather than encouraging patient Cornelius Mahoney to receive care consistent with that doctrine or transferring care to other providers, you have encouraged a morally unacceptable option,” the letter said.
The directives state that Catholic health care providers “may never condone or participate in euthanasia or assisted suicide in any way.” Such acts are described as “intrinsically immoral” and “intrinsically evil” in the document.
“Patients experiencing suffering that cannot be alleviated should be helped to appreciate the Christian understanding of redemptive suffering,” the document states.
Centura officials confirmed Thursday that Morris is no longer employed there, adding in a statement that the firm “expects all our caregivers to act in a manner consistent with our Mission and Core Values.”

Company officials did not address claims that Centura violated state law but argued that its policy prohibiting doctors from prescribing drugs or otherwise participating in medical aid-in-dying is federally protected.
“We believe the freedom of religion doctrine at the heart of the First Amendment to the U.S. Constitution supports our policies as a Christian health-care ministry,” Centura spokeswoman Wendy Forbes said in an email. “We will vigorously defend our Constitutional rights.”
Legal experts said that Morris’ firing may be rare or even unprecedented, but the argument based on the First Amendment has gained support recently in conservative circles.
“In recent years, the radical right has gotten traction with the argument that religious peoples’ constitutional rights are violated if they have to follow the same law as everybody else,” said Robert Rivas, a Florida lawyer who serves as general counsel for the Final Exit Network, a nonprofit group that promotes right-to-die causes.
“When you look closely at what they are saying,” he said, “it turns out they really want to be empowered to force their religion on others.”
Officials with the Archdiocese of Denver said they supported Centura’s efforts to uphold church doctrine.
“Asking a Christian hospital to play any role in violating the dignity of human life is asking the Christian hospital to compromise its values and core mission,” spokesman Mark Haas said in a statement. “This is not the hospital forcing its beliefs upon others, but rather having outside views forced upon it.”
The issue is playing out against growing federal protections for religious views of health care, said Kathryn Tucker, executive director of the End of Life Liberty Project and co-counsel on the Centura lawsuit filed Aug. 21.
The Trump administration conscience rule, which was challenged by two dozen states and cities, including Colorado, has been delayed until Nov. 22.
“What’s getting lost here is the patient, and the doctor may hold equally strong ethical and religious views as Centura,” Tucker said. “Why should their views be overridden by the views of corporate religious medicine?”
Morris’ termination was immediate, according to the letter. She was asked to hand over her badge and her company laptop computer. The action abruptly halted her care of 400 geriatric ╠²patients and left Morris worried about their future.
“These are complex, ill patients,” Morris said. “We have a pretty big thing in medicine about not abandoning patients, so that’s a pretty big issue.”
In the lawsuit, Morris joined with Mahoney, a Golden, Colo., nursery manager diagnosed in July with stage 4 metastatic cancer. The pair alleged that Centura’s policy prohibiting doctors from prescribing aid-in-dying drugs is broader than state law allows.
Colorado’s , approved by 65% of voters in 2016, allows hospitals and health systems to opt out of offering aid-in-dying drugs for use on their premises.
In addition, another Colorado law says health care facilities may not “limit or otherwise exercise control” over a physician’s medical judgment.
The suit asks a judge to rule that the hospital system may not bar Morris from prescribing the lethal drugs ŌĆö or penalize her if she does.
Centura officials expressed sadness over Mahoney’s illness but said the institution promotes “the sacredness of every human life.”
After he received his grim diagnosis, Mahoney asked an oncologist and a social worker at his cancer center to help him access aid-in-dying. Both said no.
“I feel like I got slapped in the face,” Mahoney said.
Mahoney was advised to transfer his care to a secular provider, but he said he didn’t want to undergo additional tests, costs and travel as he struggled with debilitating symptoms.
Morris said she understood that Centura was religiously affiliated when she was hired but didn’t anticipate a problem.
“I didn’t think it was going to affect my general family practice,” she said. “Until these conversations about medical aid-in-dying, I hadn’t felt any interference.”
Once the law passed, however, a growing number of patients asked about the option.
“I’ve had patients as they face devastating illness or the end of life where they say, ŌĆśWill you do this for me?’” she said, adding later: “At a certain point, we have to stand up for what’s right.”
Morris is considering her next steps, including separate legal action against Centura over her termination. Mahoney, who is scheduled for his third round of chemotherapy soon, said he’s not sure what to do in the wake of the firing.
Raised Catholic, he said, he rejected that theology long ago.
“I don’t believe in church. I don’t believe in religion,” he said. “I just think they’re getting way too much power.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/doctor-fired-catholic-hospital-challenges-aid-in-dying-laws/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=991939&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>At issue is a proposal that UCSF Medical Center affiliate with Dignity Health, a massive Catholic health care system that, like other Catholic chains, is bound by ethical and religious directives from the United States Conference of Catholic Bishops. Among other prohibitions on services, Dignity hospitals ban abortions unless the mother’s life is at risk, in vitro fertilization and physician-assisted death. Twenty-four of Dignity’s 39 hospitals prohibit contraception services and gender-confirming care for transgender people, such as hormone therapy and surgical procedures.
The affiliation would not keep UCSF from performing such procedures at its own medical center and outpatient clinics, and both entities would remain independent. UC doctors with practicing privileges at Dignity would be free to discuss all treatment options and could refer patients to other facilities when necessary.
But they would have to abide by Dignity’s care restrictions while practicing at Dignity hospitals.
For opponents of the plan, the issue boils down to a clear-cut principle: How can a public hospital that has been a leader in women’s health care and medical services for the gay and transgender community partner with a private system that not only denies such services but also casts them as immoral?
“It feels really concerning to me that our university that has been a fierce advocate for women’s health and LGBTQ health would be affiliating with a corporation that doesn’t support those values and restricts care,” said Dr. Jody Steinauer, who directs UCSF’s Bixby Center for Global Reproductive Health.
The two systems already have a relationship among several departments, including neurology, cardiology and adolescent psychology. This new affiliation would formalize the collaboration at Dignity’s four Bay Area hospitals and could expand services to departments including cancer care and cardiology, which would be staffed by UCSF physicians.
The proposal has sharply split faculty and medical staff at UCSF, who are airing their differences in impassioned letters and heated public forums. Participants on both sides include national figures renowned in their specialty fields.
Supporters of a closer alliance with Dignity say it’s an easy way to add capacity to a public health care system that is strapped for bed space and turning away more than 800 patients a year. They also note that Dignity is California’s largest private provider for patients with Medi-Cal, the state-federal insurance program for the poor.
“So much health care is being delivered in this country by faith-based organizations. For us to not participate with them seems like a missed opportunity,” Mark Laret, president and CEO of UCSF Health, told a December meeting of the UC Board of Regents, which must decide the issue.
The agreement could include a new labor and delivery unit based at Dignity’s St. Francis Memorial Hospital, which would be staffed by non-UCSF obstetricians. That would let Dignity absorb more patients with low-risk pregnancies, leaving UCSF time and space to deal with more complex cases, said Dr. Dana Gossett, a UCSF obstetrician-gynecologist who has been part of the negotiations with Dignity.
“I feel a little like women’s health has been portrayed as a casualty of this negotiating,” said Gossett. “But as someone who works in labor and delivery and is in the trenches every day, I see it differently. I see the damages our capacity problems have on women right now because we haven’t expanded our capacity enough to meet the need.”
Of particular concern to opponents of the affiliation are two recent lawsuits against Dignity filed by the American Civil Liberties Union. In one case, a woman was denied a tubal ligation following a cesarean section delivery at a Dignity facility in Redding, Calif. In another, a transgender man was denied a hysterectomy after a Dignity facility in Sacramento learned the procedure was part of his plan to align his gender identity and body.
In March, Steinauer, the head of the Bixby Center, joined more than 1,500 UCSF faculty members, residents, students and alumni in signing a letter opposing the affiliation. “Our affiliation with [Dignity] not only compromises the safety and quality of our patient care, but also threatens the integrity of our reputation as a provider of evidence-based care in an inclusive environment free of bias and discrimination,” they wrote.
UCSF is hardly the first public hospital to wrestle with the question of Catholic health care.
Catholic hospital systems now oversee 1 in 6 acute care hospital beds in the U.S., according to , a nonprofit group that tracks hospital consolidation. And the number of hospitals that are Catholic-owned or -affiliated increased by 22% from 2001 to 2016.
Earlier this year, Dignity Health joined forces with another system called Catholic Health Initiatives in a merger approved by both the California Department of Justice and the Vatican. The resulting $29 billion system, CommonSpirit Health, has 119 acute care hospitals and is now the largest nonprofit hospital system in the country, according to MergerWatch.

As health systems across the country scramble to merge and affiliate to gain market share, Catholic health systems have become an appealing partner for some secular hospitals, even when values diverge. In a highly consolidated region like Northern California, partnership options are limited.
The University of Michigan is affiliated with two Catholic systems: Trinity Health and Ascension. The University of Washington affiliated with the Catholic nonprofit PeaceHealth in 2013.
Entanglements between secular and Catholic hospitals have presented problems, said Lois Uttley, who runs MergerWatch. During a trial affiliation between secular Sierra Vista Regional Health Center and the Catholic Carondelet Health Network, both in Arizona, obstetricians initially were told they could perform tubal ligations, only to be told later they needed to stop. The partnership .
The UCSF administration said a formal affiliation is necessary to expand services and increase revenue. Dignity is already an important part of UCSF’s , a network of doctors and hospitals that can earn bonuses for delivering medical care more efficiently under a program created by the Affordable Care Act. Canopy Health aims to provide care for upwards of 200,000 patients within a few years.
The details of the arrangement are being worked out, but under discussion is the possibility that UCSF will get a financial stake in the affiliated Dignity hospitals, according to UCSF administrators.
The arrangement would provide “a revenue flow to support some of our money-losing programs,” UCSF’s Laret told the UC Regents this month. “There really is not a good alternative from our standpoint,” he added. “If we have to disengage from our partnership with Dignity, forget UCSF, I think that it’s catastrophic for the health care delivery system in San Francisco.”
Dignity, meanwhile, would benefit from the inflow of patients at hospitals that often operate under capacity.
UCSF has promised workarounds to avoid potential conflicts where Dignity’s hospitals prohibit services. Patients would be informed upfront about which services are not provided at Dignity facilities, for example, so they could choose to go to their preferred hospital. No UCSF staff would be asked to provide obstetric or reproductive services at Catholic facilities. And if patients at a Dignity hospital needed a prohibited service, they could be transferred to UCSF.
In an emailed statement, Dr. Todd Strumwasser, a Dignity Health senior vice president, wrote that “physicians practicing at Dignity Health hospitals may discuss all treatment options with patients” and “facilitate access” to another site when a Dignity hospital does not provide a certain service. “In a situation in which a pregnant woman’s life is in danger, life-saving procedures that may result in termination of the pregnancy will be performed.”
Such policies, however, are subject to changes by the bishops who set the rules at Catholic hospitals, said Lori Freedman, a UCSF professor who studies reproductive health care at Catholic hospitals.
“We don’t know what the future really looks like,” Freedman said. “Sometimes workarounds don’t stick around.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/will-ties-to-a-catholic-hospital-system-tie-doctors-hands/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=943552&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Ronni Bennett, who writes a popular , discovered that recently when she heard that cancer had metastasized to her lungs and her peritoneum (a membrane that lines the cavity of the abdomen).
There is no cure for your condition, Bennett was told by doctors, who estimated she might have six to eight months of good health before symptoms began to appear.
Right then and there, this 77-year-old resolved to start doing things differently ŌĆö something many people might be inclined to do in a similar situation.
No more extended exercise routines every morning, a try-to-stay-healthy activity that Bennett had forced herself to adopt but disliked intensely.
No more watching her diet, which had allowed her to shed 40 pounds several years ago and keep the weight off, with considerable effort.
No more worrying about whether memory lapses were normal or an early sign of dementia ŌĆö an irrelevant issue now.
No more pretending that the cliché “we’re all terminal” (since death awaits all of us) is especially insightful. This abstraction has nothing to do with the reality of knowing, in your gut, that your own death is imminent, Bennett realized.
“It colors everything,” she told me in a long and wide-ranging conversation recently. “I’ve always lived tentatively, but I’m not anymore because the worst has happened ŌĆö I’ve been told I’m going to die.”
No more listening to medical advice from friends and acquaintances, however well-intentioned. Bennett has complete trust in her medical team at Oregon Health & Science University, which has treated her since diagnosing pancreatic cancer last year. She’s done with responding politely to people who think they know better, she said.
And no more worrying, even for a minute, what anyone thinks of her. As Bennett wrote in a , “All kinds of things ŌĆ” fall away at just about the exact moment the doctor says, ŌĆśThere is no treatment.’”
Four or five times a day, a wave of crushing fear washes through her, Bennett told me. She breathes deeply and lets it pass. And no, psychotherapy isn’t something she wants to consider.
Instead, she’ll feel whatever it is she needs to feel ŌĆö and learn from it. This is how she wants to approach death, Bennett said: alert, aware, lucid. “Dying is the last great adventure we have ŌĆö the last bit of life ŌĆö and I want to experience it as it happens,” she said.
Writing is, for Bennett, a necessity, the thing she wants to do more than anything during this last stage of her life. For decades, it’s been her way of understanding the world ŌĆö and herself.
In a notebook, Bennett has been jotting down thoughts and feelings as they come to her. Some she already has shared in a series of about her illness. Some she’s saving for the future.
There are questions she hasn’t figured out how to answer yet.
“Can I still watch trashy TV shows?”
“How do I choose what books to read, given that my time is finite?
“What do I think about rationale suicide?” (Physician-assisted death is an option in Oregon, where Bennett lives.)
Along with her “I’m done with that” list, Bennett has a list of what she wants to embrace.
Ice cream and cheese, her favorite foods.
Walks in the park near her home.
Get-togethers with her public affairs discussion group.
A romp with kittens or puppies licking her and making her laugh.
A sense of normalcy, for as long as possible. “What I want is my life, very close to what it is,” she explained.
Deep conversations with friends. “What has been most helpful and touched me most are the friends who are willing to let me talk about this,” she said.
, she has invited readers to “ask any questions at all” and made it clear she welcomes frank communication.
“I’m new to this ŌĆö this dying thing ŌĆö and there’s no instruction book. I’m kind of fascinated by what you do with yourself during this period, and questions help me figure out what I think,” she told me.
Recently, a reader asked Bennett if she was angry about her cancer. No, . “Early on, I read about some cancer patients who get hung up on ŌĆśwhy me?’ My response was ŌĆśwhy not me?’ Most of my family died of cancer and, 40 percent of all Americans will have some form of cancer during their lives.”
Dozens of readers have responded with shock, sadness and gratitude for Bennett’s honesty about subjects that usually aren’t discussed in public.
“Because she’s writing about her own experiences in detail and telling people how she feels, people are opening up and relaying their experiences ŌĆö things that maybe they’ve never said to anyone before,” Millie Garfield, 93, a devoted reader and friend of Bennett’s, told me in a phone conversation.
Garfield’s parents never talked about illness and death the way Bennett is doing. “I didn’t have this close communication with them, and they never opened up to me about all the things Ronni is talking about,” she said.
For the last year, Bennett and her former husband, Alex Bennett, have broadcast video conversations every few weeks over YouTube. (He lives across the country in New York City.) “What you’ve written will be valuable as a document of somebody’s life and how to leave it,” he as they talked about her condition with poignancy and laughter.
Other people may have very different perspectives as they take stock of their lives upon learning they have a terminal illness. Some may not want to share their innermost thoughts and feelings; others may do so willingly or if they feel other people really want to listen.
During the past 15 years, Bennett chose to live her life out loud through her blog. For the moment, she’s as committed as ever to doing that.
“There’s very little about dying from the point of view of someone who’s living that experience,” she said. “This is one of the very big deals of aging and, absolutely, I’ll keep writing about this as long as I want to or can.”
čŅ╣¾Õ·┤½├ĮęĢŅl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/at-deaths-door-shedding-light-on-how-to-live/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=888729&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>