“They’re the folks that work at restaurants. They’re the teacher’s aides,” said Starr, a registered nurse who became Open Door’s chief executive more than six years ago. Those patients, he said, are “really the heart and soul of rural America.”
He said if his remote health centers don’t get a share of the billions of dollars Congress earmarked to transform health care in rural America, patients may soon lose services. About 50% of Open Door’s 60,000 patients are on Medicaid, the joint state and federal insurance program that, together with the related Children’s Health Insurance Program, covers with low incomes or disabilities.
When Congress approved the One Big Beautiful Bill Act last summer, it cut nearly $1 trillion from Medicaid over the next decade. Now, Starr hopes the $50 billion Rural Health Transformation Program, which was part of the same bill, will help keep his patients covered.
Yet, small community health care providers, such as Open Door, may find they are sharing the billions with an army of corporate giants before it reaches their patients.
Months after federal leaders announced that all 50 states won first-year awards, ranging from $147 million for New Jersey to $281 million for Texas, state plans reveal that a heavy dose of prescribed spending will go to companies that can increase the use of electronic health records, strengthen cybersecurity, and improve state and health system technology platforms.
And at least four large-scale coalitions of companies are now pitching multipronged services to the states. Many of the companies already work with regional health systems and states through Medicaid contracting or mobile and telehealth operations.
How those services will help improve the health care of rural Americans at places such as Open Door remains an open question.
States Stare Down Reporting Deadlines
Federal regulators were “really interested in seeing digital health investments” when they crafted the five-year rural health program rules last year, said Maya Sandalow, an associate director at the Bipartisan Policy Center, a think tank based in Washington, D.C. She co-authored a recent report on how the 50 states plan to invest in technology, including modernizing health care infrastructure and expanding virtual care options such as telehealth and remote patient monitoring.
“The rural health fund isn’t really designed to directly replace or offset the lost Medicaid funding,” Sandalow said, noting that the federal staffers in charge of the program — money that could help rural hospitals and clinics pay for patient care — at 15% of the total funding awarded to a state.
Federal regulators also established tight reporting deadlines, forcing states to move quickly.
States must file progress reports and obligate all first-year funding , according to the Centers for Medicare & Medicaid Services, the federal agency overseeing the program. States could see their awards decreased or terminated at any time if they fail to follow federal requirements, according to the .
As of early April, CMS had not approved or had only partially approved some state budgets, including those of Wyoming, Colorado, and Vermont, according to state officials. CMS spokesperson Catherine Howden, who declined to say which states still needed revised budgets approved, said the agency does not provide “state-by-state updates.”
In Alaska, the budget is approved but the state has not announced when it will release full grant proposals and awards, said Tricia Franklin, program coordinator for Alaska’s rural health transformation.
“Early summer was the target,” Franklin said. But the response from vendors and applicants has been “much greater than expected, so it may take us a little longer.”
Working with consulting companies is an established way for states to “quickly and effectively” meet federal deadlines and roll out grant money, said , national director for population health at the Milbank Memorial Fund, a nonprofit focused on state health policy work.
Upgrading Technology, Modernizing Rural Health
Science Applications International Corp., a Fortune 500 government contractor, pulled together the . SAIC does a variety of technology work such as cybersecurity and engineering support. The alliance also includes Walgreens and Mission Mobile Medical, which turns RVs into primary care clinics. A data analytics company, a telemedicine and software company, and a company that helps place medical graduates in health systems are also part of the coalition.
The SAIC alliance offers “an ecosystem” of companies that can coordinate the work states have promised, said , SAIC’s Rural Health Transformation Program lead and a former chief information officer for the Virginia Department of Health. Each of the companies has representatives focused on the rural program, he said.
A lack of digital infrastructure — such as electronic health records at different clinics and hospitals that can talk to one another — has been a consistent barrier for rural medical care teams, said the Bipartisan Policy Center’s Sandalow.
“The funding hasn’t always been there in order for rural areas to create the infrastructure that’s needed to fully adopt remote patient monitoring, telehealth, artificial intelligence in ways that will really be supportive,” Sandalow said. “It takes things like updating infrastructure, changing workflows.”
Sandalow’s found that Maine and Utah are investing in cybersecurity; Indiana, Missouri, and New Mexico plan to modernize their electronic health records; Oklahoma plans to buy hardware and software, subsidize subscriptions, and give technical support to rural providers; and states such as Arizona and South Carolina will use funds to create telehealth hubs or buy remote patient monitoring equipment.
Federal regulators, when creating the rural program’s spending rules, also said no more than 5% of a state’s total funding awarded could be used to replace electronic medical records systems that already meet federal standards. Sandalow said that means states will focus on enhancements and upgrades to their current systems.
Gainwell Technologies, which operates the systems for dozens of state Medicaid programs, is spearheading . Rushil Desai, a Gainwell senior vice president, said states’ detailed spending plans are “changing in real time.”
Maine’s Medicaid plan contracts with Gainwell, and the state’s initial application listed four contracts worth more than $16 million over five years for the company. The state confirmed it has received federal approval for only its first year of spending, which includes a to implement changes to the state’s Medicaid claims system.
James Lomastro, a senior-care advocate in rural Massachusetts with the nonprofit , said he worries that large vendors and health systems will get the state’s transformation dollars.
Clinics, home care agencies, and nursing homes that “actually provide day-to-day support in the community are mostly on the margins” of state discussions about how to spend the money, he said. A spokesperson for Massachusetts’ Executive Office of Health and Human Services, Olivia James, said state officials would “ensure that everyone has a seat at the table” with training, financial incentives, and direct investments.
Arizona’s rural fund budget, which is $167 million for the first year, allocates for medical diagnostic equipment and technology upgrades, including to electronic health records, specifically for rural health care facilities.
But it also for county public health departments, said Pima County Public Health Director Theresa Cullen. The approved budget includes up to $4 million for grants to support community health workers.

“In these rural communities, you need to be present,” Cullen said.
Alina Czekai, director of the CMS rural health transformation office, said her team plans to visit all 50 states. She spoke at the National Rural Health Association’s policy conference in Washington, D.C., in February and told the audience that her team wants “the money to go to rural communities, rural providers, rural patients.” The association’s members include rural hospitals and clinics, which are expected to suffer big losses under the Medicaid cuts.
In California, Open Door’s Starr said he provided input on his state’s initial application, which won $234 million in first-year funding, but he is not clear on what the next steps will be for getting money from the program.
For his patients, Starr said, money is needed for technology upgrades. After all, he said, updated electronic health systems could operate seamlessly and store the documentation needed to keep a patient enrolled in Medicaid.
Updated technology could be exactly what Open Door and other area clinics need to “help keep people covered,” Starr said.
Ñî¹óåú´«Ã½Ò•îl Health News senior correspondent Phil Galewitz and rural health care correspondent Arielle Zionts contributed to this report.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-program-cms-state-contractors-ehr-patients/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228223&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The plan was to begin handing out boxes of groceries at 11, but the truck delivering the food blew a tire en route. No one complained.
Perry Hall was among those waiting. His wife, Lilly Hall, volunteers with the distribution team. Perry has been dealing with a form of cancer called multiple myeloma. The Halls get by on around $1,500 a month from his Social Security benefits, plus assistance from the federal , or SNAP. But because of her age, Lilly, 59, recently became subject to new SNAP work requirements and at risk of losing her benefits.
As part of the federal One Big Beautiful Bill Act, all “able-bodied adults” 64 or younger who don’t have dependents and don’t work, volunteer, or participate in job training at least 80 hours a month are now restricted to three months of benefits every three years from SNAP, formerly known as food stamps. Previously, the federal requirement applied to those 54 or younger. The new rule, which went into effect in November, also applies to parents of children 14 or older. And it removed exemptions for veterans, people experiencing homelessness, and young adults who’ve aged out of foster care.
Proponents of work requirements argue that they incentivize people who are “work-ready” to seek and keep jobs, reducing dependence on government assistance and upholding the “.”
Rhonda Rogombé serves as health and safety net policy analyst for the . She and her colleagues have studied the effects of SNAP work rules and found that requiring recipients to work does not lower an area’s unemployment rate.
Previous work requirements were suspended nationwide during the covid pandemic and reinstated in fall 2023. The researchers found that the average number of people employed in Mingo County each month actually went down after the requirement was reimposed.
A 2018 federal research project that examined several data sources, including SNAP data from nine states, found that work requirements “have no impact on labor force participation and the number of hours worked.”
There are a number of possible explanations, Rogombé said, “but when people are hungry, they’re not able to support themselves. When people are hungry, it’s harder to focus at work. It’s harder to engage in work activity, and we think that that’s part of it.”
Jobs are scarce in this southern West Virginia county. Lilly Hall found work at a Delbarton restaurant. But it’s unpaid until a waitress position opens — enough to preserve her benefits, but far from ideal.
On that mild Wednesday in late March, House of Hope provided chicken, eggs, bread, potatoes, fresh fruit and vegetables, and milk.
Among those in line were older residents and “some young people that have lost their way and they can’t get work and they just need help,” said Timothy Treleven, who operates the pantry with his wife, Christine, and Gail Lendearo.

House of Hope’s scheduled distribution day is the last Saturday of each month — supplemented by occasional weekday Facing Hunger visits — as money from monthly checks begins to run out and cupboards go bare.
On a typical Saturday, pantry staff and volunteers hand out up to 400 boxes of food.
“It’s an honor to do this,” Lendearo said. “It’s a blessing.”
Perry Hall’s cancer is now in remission, but for a while his treatment required that he and Lilly travel back and forth, 4½ hours each way, to Morgantown. The couple’s van couldn’t make the trip, so they paid a friend for rides.
Mingo’s population is just under 22,000, down from around 27,000 in 2010. It once flourished, fueled by coal. Williamson, the county seat, was home to an opera house and businesses operated by immigrants from Italy, Russia, and Syria. The region is still referred to as “the coalfields,” but little is mined here these days. .
Rogombé and her colleagues found that Mingo County residents face significant barriers to securing what few jobs are available. These include unreported physical and mental impairments, housing insecurity, and a lack of high school diplomas and identification documents.

Filing the paperwork to receive benefits or to confirm compliance is difficult for many residents. The West Virginia Center on Budget and Policy’s research found that about 1 in 4 lack reliable internet access.
Additional changes lie ahead for the SNAP program. Currently, the federal government and the states share administrative costs equally, but in October states will assume 75% of those costs. And beginning in October 2027, they’ll be required to pay additional costs based on .
Kentucky, like West Virginia, is among the poorer states that will be most affected by the new requirements and costs. The Kentucky Center for Economic Policy estimates that with the expanded work requirements.
Jessica Klein, a researcher with the center, worries about the consequences. “We know SNAP has an impact on health, and not just because it decreases food insecurity,” she said. It worsens blood pressure rates, obesity, medication adherence, and more.
With the additional financial burden placed on states, “I think what we’ll see is some states changing rules that impact participation in order to have a smaller, more affordable program,” Klein said. “My fear is that some states will choose not to operate SNAP at all.”
In Mingo County, folks are stepping up. At least eight food pantries offer groceries to those in need.
Janet Gibson runs the Blessing Barn pantry in the Ben Creek community. “I can go from one end of the creek to the other” and tell you everyone’s name and a little something about them, she said. She takes pride in feeding her people.

Gibson said it can be hard to find even volunteer opportunities in the county, largely because of transportation challenges. A look at a local map can be misleading: A couple of dozen miles into a holler or up a ridge could take an hour or more.
“Whether you’re working full-time or not, you’re still spinning out gas to get to work,” Gibson said, “and gas ain’t cheap now.”
A single mother of three, Trista Shankle of Paducah, Kentucky, isn’t subject to the new SNAP requirements, but she worries about the fragility of the social safety net. She overcame challenges, is earning a master’s degree in social work, and works for an organization that connects community college students with benefits. Her family receives SNAP, Medicaid, housing support, and assistance from the USDA’s . If any one of those is cut, she said, she may have to drop out of school.
Shankle is certain she wouldn’t have advanced to where she is today without the benefits she and her family have received: “They bring a sense of calm and comfort. I know that my kids aren’t going to go hungry.”
The first week in April, Lilly Hall reported for work at Black Bear Trails Restaurant. She’s grateful for the opportunity. And when a waitress slot opens, “I’ll snag that position so quick it’ll make your head flip.”
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/food-stamps-snap-work-requirements-hunger-west-virginia-foodbanks/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228111&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But Republican lawmakers in some states think the new rules — part of the GOP’s One Big Beautiful Bill Act, signed last July by President Donald Trump — don’t go far enough.
Indiana is leading that charge, with a new law that requires applicants to prove they’ve been working or participating in a similar activity for three consecutive months to get benefits.
Meanwhile, residents in many other states will have to show they’ve been working just one month, the least cumbersome option under Trump’s signature tax-and-domestic-spending law. It instructs states to decide whether to require one, two, or three months of work history.
As in Indiana, Republican Idaho lawmakers approved a three-month requirement, and the state’s governor signed the bill into law on April 10.
The efforts, along with similar moves in Arizona, Missouri, and Kentucky, are aimed at restricting flexibility to implement the federal law at the state level.
“Normally, you would not see state legislators weighing in on these decisions,” said Lucy Dagneau, a senior official with the American Cancer Society’s advocacy arm.
The nonpartisan Congressional Budget Office estimated 18.5 million adults will be subject to the new rules, which will be enforced across 42 states and the District of Columbia. In Indiana, work rules will target about 33% of the state’s Medicaid population. The rules generally wouldn’t apply to children, people 65 or older, or people with disabilities or serious health issues.
Typically, state administrators — not lawmakers — detail how they plan to comply with new federal standards, and they often look to federal regulators for guidance. But officials at the Centers for Medicare & Medicaid Services have yet to tell states how to comply with many aspects of the sweeping budget law, leaving state lawmakers to intervene.
Gov. Mike Braun, a Republican, signed the Indiana bill into law on March 4, making his state the first to set the Medicaid work requirement at three months — the longest period allowed under the federal law.
Republican state Sen. Chris Garten introduced a bill in January, saying it was needed to “align” state law with the new federal Medicaid rules. He also pitched the bill as a way to crack down on “waste, fraud, and abuse” in public programs.
When ineligible people get enrolled, it robs “the truly vulnerable Hoosier who actually needs the help,” Garten said during a January committee hearing.
Democratic state Sen. Fady Qaddoura expressed skepticism during the hearing and questioned the necessity of the legislation. Qaddoura asked Indiana Family and Social Services Administration Secretary Mitch Roob to provide an estimate of the number of ineligible people who enrolled in Medicaid in the state.
“I think very few,” Roob replied. “It’ll never be none.”
After hearing Roob’s answer, Qaddoura said there is no evidence of a widespread problem in Indiana. He accused Republicans of using waste, fraud, and abuse as justification to deny health benefits and food aid to vulnerable Hoosiers.
Garten later called Qaddoura’s accusation a “fundamental mischaracterization” of the bill.
Republicans have said imposing these limits protects the Medicaid program’s longevity.
“We believe in a safety net for our most vulnerable, not a hammock for able-bodied adults that choose not to work,” Garten said. “By tightening these screws, we ensure that our safety net remains sustainable.”
Indiana’s Medicaid enrollment is expected to decrease because of Garten’s legislation, according to an analysis from Indiana’s nonpartisan Legislative Services Agency.
Medicaid helps keep people healthy, so they can continue to work, said Adam Mueller, executive director of the Indiana Justice Project, a nonpartisan legal advocacy organization focusing on health, housing, and food insecurity.
Mueller worries that people will struggle to prove their work history, especially those with nontraditional jobs.
“If the point is to get people engaged, the one month would do it,” Mueller said.
Ultimately, he fears the law will harm Hoosiers with the greatest need for assistance. “They’re going to get tripped up by the bureaucratic hurdles.”
An analysis by the Center on Budget and Policy Priorities predicted that work rules will and that how states choose to implement the rules will “significantly affect the number of people who lose coverage.” State policy decisions will determine just “how intense the burden is,” the left-leaning think tank found, and opting for a shorter look-back period “will enable more people to enroll.”
Lawmakers in multiple states considered limits. And the same right-leaning lobbying group, the Foundation for Government Accountability, testified in favor of these measures in Arizona, Indiana, and Missouri.
In Missouri, FGA lobbyist James Harris said the measure intends to “move people from dependency and give them back that dignity and pride of work.”
Missouri state Rep. Darin Chappell proposed requiring a three-month look-back period like the measure in Indiana. But the latest version of the bill he sponsored would require applicants to show they were working for only one month before enrolling.
Chappell, a Republican, said his initiative would encourage a “working mindset.”
Anna Meyer, owner of a small bakery in Columbia, Missouri, said the implication is that she and others on Medicaid are lazy. “I have been working since I was 15 years old,” she said. “I’m 43 now.”
Meyer, who voiced her opposition, said she previously had problems submitting information to the state Medicaid agency. She fears new reporting requirements will put her and others at risk of losing coverage, even if they meet the work rule.
She has fibromyalgia, a chronic condition that increases overall sensitivity to pain. She also has food allergies. Medicaid helps pay for medications and doctor visits that keep her healthy and allow her to keep working.
“I work very hard,” Meyer said.
In St. Louis, Jessica Norton, an OB-GYN, treats many Medicaid patients at an Affinia Healthcare clinic. She said they struggle to remain insured even though Missouri extends a full year of Medicaid coverage to eligible women after they give birth. Some of her patients are inexplicably kicked off that coverage by the time of their checkups six weeks after birth. She fears red tape from the new work requirements will make it harder to hang on to insurance, even though pregnant women and new mothers are supposed to be exempt.
Norton criticized lawmakers for the message this policy sends to vulnerable patients. They are saying, “Oh, actually, health care is a privilege, and you have to earn it,” she said.

of adults ages 19 to 64 on Medicaid already work, according to KFF. The reason many of the remaining adults on Medicaid are not working is that they are retired, serving as a caregiver, or too sick, KFF has found.
Some states are not only setting the strictest requirements but also blocking out the optional leniency built into the federal rules.
For example, states may adopt additional exemptions from work rules, such as allowing people to claim a “short-term hardship,” designed to provide continued Medicaid coverage to people with medical conditions that prevent them from working.
Missouri lawmakers are seeking a constitutional amendment to bar their state from offering such optional exemptions. But patient advocates warn these limits would harm the state’s vulnerable residents when they need coverage the most, particularly Missouri’s rural cancer patients.
Often, rural Missouri patients must travel to Kansas City or St. Louis for treatment, disrupting their ability to work, Emily Kalmer, a lobbyist for the American Cancer Society’s advocacy arm, testified at the January hearing. Recognizing this, the federal law provides certain exemptions for this kind of scenario.
But this short-term hardship exemption would be off the table in Missouri.
Time is “very important in the life of a cancer patient or a cancer survivor,” Kalmer said.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/federal-medicaid-work-rules-one-three-months-indiana-missouri/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228139&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>HAY SPRINGS, Neb.— The sun was just warming the horizon as Mark Pieper left his house near his cattle ranch on a crisp February morning.
It’s not unusual for the rancher to wake up early to tend to livestock, but at 5:45 a.m. this day his cattle wouldn’t come first. For the past 3½ years, three days a week, Pieper has made an early-morning commute to get dialysis at the nearest hospital.
Pieper lives outside Hay Springs, which has 599 residents, according to a sign at the edge of town. He makes sure not to forget his chocolate-brown cowboy hat before starting up his pickup truck for the half-hour drive to Chadron.
That February morning was one of his last dialysis sessions there before the hospital shuttered the service at the end of March.
“I guess I’ll just bloat up and die in a month,” Pieper remembered thinking when he learned the center was closing, eliminating the only option near his home.
He needs dialysis to survive after cancer treatment damaged his kidneys.
Pieper and 16 other patients relied on Chadron Hospital for the life-sustaining therapy that filters waste and fluid from their blood — a job their failing kidneys could no longer do. Treatment lasts about four hours.

The closure is just one example of the long decline of health care services in rural America, where people have higher rates of many chronic conditions but less access to care than elsewhere.
The Trump administration promised to address this problem, when it launched the $50 billion federal Rural Health Transformation Program in September. It may not be enough to stop the trend.
“[President Donald] Trump says he is going to help the rural health care,” Pieper said. Dialysis “is one thing that we really need here.”
Some patients have moved to live closer to care, including several nursing home residents. Their new facilities may be farther from their families.
Others are making long drives to dialysis centers. Pieper eventually found treatment in Scottsbluff, which, with about 14,000 residents, is the biggest city in the rural Panhandle region of western Nebraska. The hour-and-a-half drive will triple his time on the road to more than nine hours each week.
Jim Wright and his wife reduced their drive time — but are spending more money — by renting a small home near Rapid City, South Dakota, and living there on weekdays so he can get dialysis. Wright said he understands that rural hospitals face financial challenges.
“But we’re talking about something that’s lifesaving. It’s not a matter of, ‘Oh, I would like to be there’” getting treatment, he said. “It’s a case that if you don’t, you die.”

An Influx of Money That’s Out of Reach
Jon Reiners, CEO of the independent, nonprofit Chadron Hospital, wrestled with the decision to end dialysis services. He and several patients said that the closure was announced as the $219 million the state will receive in first-year funding from the .
But the five-year program is aimed at exploring new, creative ways to improve rural health, not to help existing services stay afloat. States can use only up to 15% of their funding to pay providers for patient care.
At least 11 states — Nebraska is not among them — have mentioned using funding for rural dialysis programs, according to a Ñî¹óåú´«Ã½Ò•îl Health News review of applications. Their ideas include starting a mobile dialysis unit and helping people get treatment at home or in long-term care facilities.
Reiners said Chadron Hospital lost $1 million a year on its dialysis service due to low reimbursement rates that didn’t cover operational costs.

The facility is a critical access hospital, a designation that allows certain small, mostly rural hospitals to get increased reimbursement rates for their Medicare patients. While most of the affected patients were on Medicare, the critical access program doesn’t cover outpatient dialysis, Reiners said.
Reiners said the hospital worked for more than a year to find solutions, such as reaching out to four private companies to potentially take over the center. But he said they all passed after realizing they would lose money.
Nephrologist Mark Unruh said the dialysis closure in Chadron reflects a wider trend of staffing and funding challenges.
“You do end up in situations where you have people who are displaced like this, and it’s just sad,” said Unruh, chair of the Internal Medicine Department at the University of New Mexico.
People in rural America face significant disparities in kidney health and treatment, published in 2024 in the American Journal of Nephrology. They’re and face after diagnosis, according to data from the National Institutes of Health.
The best way to address this is to focus on prevention, Unruh said. He pointed to a that helps primary care doctors in rural and other underserved areas prevent end-stage renal failure.
Another idea, Unruh said, is boosting the rate of kidney transplantation for rural patients. He’s looking at whether it’s helpful to “fast-track” tests patients need to get approved for a transplant by scheduling all of them over a couple of days to limit travel time.
Unruh said the U.S. health system also needs to recruit more staff who can train patients and their caregivers to administer dialysis at home.
Exploring the Option of Home Dialysis
Rural dialysis patients are more likely than urban ones to get home dialysis, according to . In 2023, the rate was nearly 18% for rural patients and about 14% for urban ones.
One type of home dialysis requires surgery to get a catheter placed in the abdomen and . The other kind requires . The nearest facility to Chadron that offers training for the first option is in Scottsbluff. The nearest that offers training for the latter kind is three hours away in Cheyenne, Wyoming.
Pieper said doctors told him he’s not a candidate for home dialysis or a transplant. The Panhandle has a nonprofit, rural transit system, but its schedule won’t work for Pieper. He said that leaves him with no choice but to get treatment in Scottsbluff, a 200-mile round trip.
It takes Linda Simonson even longer — more than four hours round trip — to drive her husband, Alan, from their ranch to his treatment in Scottsbluff.
Linda sat in the waiting room with a yellow legal pad during one of Alan’s final treatments in Chadron. The paper was scrawled with phone numbers of politicians to call and driving distances to dialysis centers in the region. She said facilities closer to their ranch either don’t have room for new patients or lack good spots along the route to take a driving break in bad weather.
“It’s just unreal,” she said.
She said even if Alan took a bus, she’d have to ride along to support him during the trip and his treatment.
Jim and Carol Wright, the couple staying near Rapid City on weekdays, said they can’t afford to rent a second home forever. Their weekly commute is already taking a physical and emotional toll. They said they’ll eventually have to move to a bigger city, giving up the house they love in the scenic Nebraska National Forest.
Carol said she feels for the dialysis staffers in Chadron, who are wonderful.
“It just doesn’t seem right to sacrifice one unit that’s so vital,” she said while standing next to a pile of moving boxes stacked inside their rental.

The Wrights wrote letters to politicians and hospital leaders to share their concerns and ideas for keeping the unit open, including using the federal rural health funding.
Simonson said she spoke with aides for the governor and her state representatives but none of the leaders called her back.
“It feels like they don’t know that we exist at this end of the state,” she said.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/dialysis-unit-closes-rural-transformation-health-fund-nebraska/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178069&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The federal government doesn’t track how many children have entered foster care because of immigration enforcement actions, leaving it unclear how often it happens. In Oregon, as of February two children had been placed in foster care after being separated from their parents in immigration detention cases, according to Jake Sunderland, a spokesperson for the Oregon Department of Human Services.
“Before fall 2025, this simply had never happened before,” Sunderland said.
As of mid-February, nearly by Immigration and Customs Enforcement. The record 73,000 people in detention in January represented an compared with one year before. According to , parents of 11,000 children who are U.S. citizens were detained from the beginning of Trump’s term through August.
The news outlet NOTUS that at least 32 children of detained or deported parents had been placed in foster care in seven states.
Sandy Santana, executive director of Children’s Rights, a legal advocacy organization, said he thinks the actual number is much higher.
“That, to us, seems really, really low,” he said.
Separation from a parent is deeply traumatic for children and can lead to , including post-traumatic stress disorder. Prolonged, intense stress can lead to more-frequent infections in children and developmental issues. That “toxic stress” is also associated with responsible for learning and memory, according to KFF.
, and amended existing laws during Trump’s first term to allow guardians to be granted temporary parental rights for immigration enforcement reasons. Now the enforcement surge that began after Trump returned to office last year has prompted a new wave of state responses.
In New Jersey, lawmakers are considering to amend a state law that allows parents to nominate standby, or temporary, guardians in the cases of death, incapacity, or debilitation. The bill would add separation due to federal immigration enforcement as another allowable reason.
Nevada and California passed laws last year to protect families separated by immigration enforcement actions. California’s law, called the , allows parents to nominate guardians and share custodial rights, instead of having them suspended, while they’re detained. They regain their full parental rights if they are released and are able to reunite with their children.
There are significant legal barriers to reunification once a child is placed in state custody, said Juan Guzman, director of children’s court and guardianship at the Alliance for Children’s Rights, a legal advocacy organization in Los Angeles.
If a parent’s child is placed in foster care and the parent cannot participate in required court proceedings because they are in detention or have been deported, it’s less likely they will be able to reunite with their child, Guzman said.
are U.S. citizens who live with a parent or family member who does not have legal immigration status, according to research from the Brookings Institution, a Washington, D.C.-based think tank. Within that group, 2.6 million children have two parents lacking legal status.
Santana said he expects the number of family separation cases to grow as the Trump administration continues its immigration enforcement campaign, putting more children at risk of being placed in foster care.
the agency to make efforts to facilitate detained parents’ participation in family court, child welfare, or guardianship proceedings, but Santana said it’s uncertain whether ICE is complying with those rules.
ICE officials did not respond to requests for comment for this report.
Before the change in California’s law, the only way a parent could share custodial rights with another guardian was if the parent was terminally ill, Guzman said.
If parents create a preparedness plan and identify an individual to assume guardianship of their children, the state child welfare agency can begin the process of placing the children with that individual without opening a formal foster care case, he added.
While Nevada lawmakers expanded an existing guardianship law last year to include immigration enforcement, the measure requires the parents to take the additional step of filing notarized paperwork with the secretary of state’s office, said Cristian Gonzalez-Perez, an attorney at Make the Road Nevada, a nonprofit that provides resources to immigrant communities.
Gonzalez-Perez said some immigrants are still hesitant to fill out government forms, out of fear that ICE might access their information and target them. He reassures community members that the state forms are secure and can be accessed only by hospitals and courts.
The Trump administration has taken through the Centers for Medicare & Medicaid Services, the IRS, the Supplemental Nutrition Assistance Program, the Department of Housing and Urban Development, and other entities.
Gonzalez-Perez and Guzman said that not enough immigrant parents know their rights. Nominating a temporary guardian and creating a plan for their families is one way they can prevent feelings of helplessness, Gonzalez-Perez said.
“Folks don’t want to talk about it, right?” Guzman said. “The parent having to speak to a child about the possibility of separation, it’s scary. It’s not something anybody wants to do.”
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/immigrants-ice-arrests-family-separation-children-foster-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178906&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Researchers say the children at about a mile away pay the price. They discovered the students there and at other elementary schools near major pollution sites in Pennsylvania had than other children in the state.
Residents and environmental advocates saw reason for hope and relief in the form of a designed to tamp down on coke oven plant pollution. But even before it took effect, President Donald Trump granted in the U.S. — including the one in Clairton — a from the standards.
Trump and Republicans have sought to align themselves with the Make America Healthy Again movement’s populist ideals, such as improving Americans’ food choices and reducing corporate harm to the environment. But the administration is ratcheting up its attacks on the very environmental protections that MAHA followers hold dear.
Taken together, these anti-environmental initiatives will lead to more pollution-related illnesses and higher health care spending, health researchers say. They could also have political ramifications, eroding MAHA’s support for GOP candidates in the November midterm elections if followers believe the party is more beholden to industry than to the movement’s agenda.
, including about a quarter of Republicans, support rolling back environmental regulations, according to a poll by the Energy Policy Institute at the University of Chicago and The Associated Press-NORC Center for Public Affairs Research.
Some MAHA supporters believe voters will support Republicans because the Trump administration is delivering on other goals important to the movement.
“MAHA has a pretty diverse set of policy goals, ranging from medical freedom to food and the environment,” said David Mansdoerfer, who served in Health and Human Services leadership during Trump’s first term. “In totality, the Trump administration has strongly delivered on much of the MAHA agenda.”
While MAHA voters have been upset at some of the administration’s actions that promote industry, it’s hard to know how that may play out in the midterms, said Christopher Bosso, a professor of public policy and politics at Northeastern University. Many were disillusioned by a Trump they viewed as promoting glyphosate, which HHS Secretary Robert F. Kennedy Jr. has .
“The glyphosate thing really ticks off a lot of them; they’re really upset,” Bosso said. “Kennedy said it was poison. If it is a poison, why aren’t we regulating it? That’s where the tension plays out.”
The situation with the Clairton coke plant and the others granted exemptions from regulations underscores the potential public health risks. Six of the 11 factories had “high priority” violations of the Clean Air Act as of last May, according to a Ñî¹óåú´«Ã½Ò•îl Health News analysis. Five coke oven plants logged major violations every quarter for at least three years straight.
“Poisoning continues to some of the most vulnerable residents of Allegheny County,” , who had lived in nearby Glassport, Pennsylvania, said at a about the coke plant.
Environmental Protection Agency spokesperson Brigit Hirsch said the president gave companies extra time because the technology needed to meet a new standard isn’t ready yet.
“Forcing plants to comply before the tools exist doesn’t make the air cleaner, it just shuts down facilities and kills jobs with nothing to show for it,” Hirsch said.
But environmental groups disagree that the plants were unable to comply at a reasonable cost, and they say the exemption from the EPA requirements shows the Trump administration is prioritizing the coal industry at the expense of public health.
“The Trump administration’s relentless actions to dismantle lifesaving environmental protections are a gut punch to the administration’s own promise to Make America Healthy Again,” said Cathleen Kelly, a senior fellow at the Center for American Progress, a liberal think tank.
Hard Times in Clairton
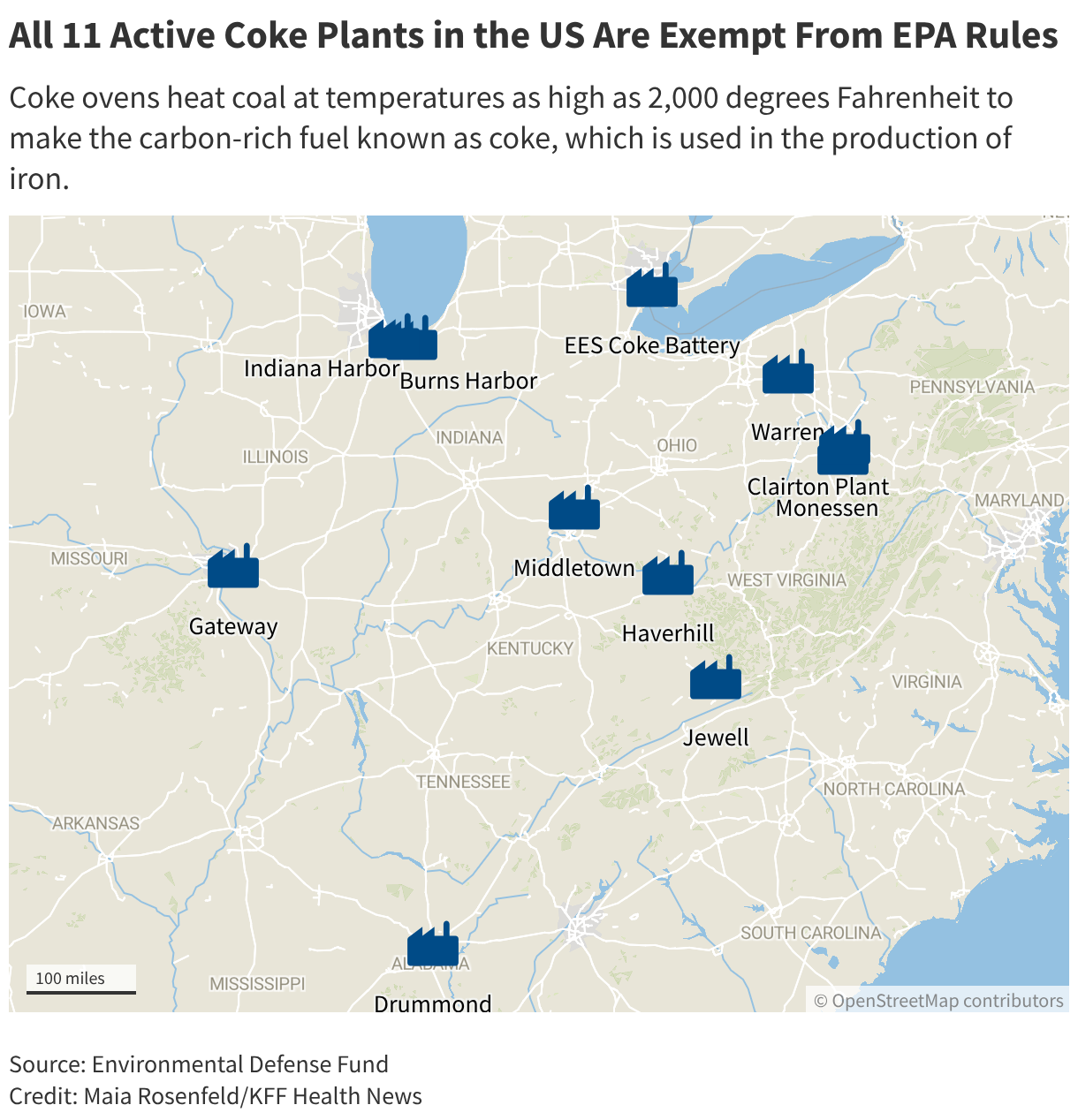
Sprawled across , the Clairton plant operates ovens in which coal is heated to as much as 2,000 degrees Fahrenheit to make up to 4.3 million tons annually of the carbon-rich fuel known as coke. The product is used in blast furnaces to produce iron.
It’s a dirty operation. The process leads to hazardous emissions of that the Centers for Disease Control and Prevention says can lead to anemia and leukemia, as well as , which can trigger severe asthma.
The Clairton operation has had repeated problems with its emissions and operations, including and of toxic chemicals. The plant has received more than from the Allegheny County Health Department since 2022, stemming largely from a fire in 2018 that led to high emissions, and violated the Clean Air Act in each of the last , with the last compliance monitoring in July 2025, according to the EPA.
Nippon Steel Corp. last year acquired U.S. Steel, which now operates as a subsidiary. The company didn’t respond to an email seeking comment. U.S. Steel said it spends $100 million annually on environmental compliance at Clairton.
“Environmental stewardship is a core value at U. S. Steel, and we remain committed to the safety of our communities,” spokesperson Andrew Fulton said in a written statement.
Clairton was once bustling with movie theaters, a mix of grocery stores, and riverside parks, with a dance pavilion and . But the decline of steel hit hard. The town’s population dwindled from more than in the mid-20th century to as of 2024. until they were razed and replaced with signs saying to keep out. The 1978 movie , which depicts a hardscrabble industrial town, is partly set there. Today, about 33% of residents live in poverty.

While the plant brings jobs and revenue, residents of the town and the surrounding areas have long complained about health problems they attribute to its emissions.
“My parents are gone. My mom had cancer, my dad,” , a Clairton resident, said at a 2025 County Council meeting. “I lost a lot of loved ones and seen other ones pass because of this mill.”
Pediatric allergist looked into asthma rates among 1,200 children who attended school near major pollution sites in the area — including students at Clairton Elementary School. They had nearly triple the national rate of asthma, with the highest rate among African American youth, according to she led.
“We were shocked,” she said. “It was double or triple what we expected. The people are proud of their industrial background. We need steel, but they’re not running a good enough operation.”
A found children with asthma living near the coke plant had an 80% higher chance of missing school when sulfur dioxide pollution was elevated.
Allegheny County, which includes Clairton and Pittsburgh, is home to a number of industrial plants, and to increased deaths, chronic heart disease, and adverse birth outcomes. It was ranked in the top 1% of counties in the nation for cancer risk from stationary industrial air pollutants in a 2018 .
Clairton has an age-adjusted cancer death rate of 170 per 100,000 people, higher than the broader county’s rate of 150 deaths per 100,000 people, based on a Ñî¹óåú´«Ã½Ò•îl Health News analysis of .
The American Lung Association in 2025 gave the county an F rating for its particle pollution levels. PennEnvironment, an environmental group that was party to a settlement with U.S. Steel involving the Clairton plant, says the coke operation caused of toxic releases in 2021, which amounted to 60% of all such releases in the county that year.
From 2020 through 2025, the Clairton plant racked up more in fines from Clean Air Act penalties than any other coke oven facility nationwide, costing U.S. Steel over $10 million, according to EPA facility reports.
“We are deeply concerned with exemptions, which allow air toxics to affect public health,” Allegheny County Health Department spokesperson Ronnie Das said in a statement.
The Clairton plant provides and hundreds of millions of dollars in tax revenue to the area. The jobs help generate nearly $3 billion in annual economic output, according to estimates from the Pennsylvania Manufacturers’ Association.
Some community members and advocacy groups hoped air quality would improve after the coke plant was sold. has pledged to upgrade facilities in the Monongahela River Valley.
Politics, Waivers, and Environmental Concerns
Under the Biden-era rule, coke plants were supposed to start meeting from the lids and doors of ovens that heat coal. They would also have had to monitor for benzene at their property lines and take steps to lower emissions of the carcinogen if they exceeded certain levels. Compliance deadlines were set for July 2025.
The Trump administration, which has sought to revive the coal industry, intervened. Last year, it , including coke plants such as Clairton’s, to seek from issued in 2024 by the EPA.
Then Trump in November went further, granting all coke plants a two-year compliance break.
The reprieve was necessary, the EPA spokesperson Hirsch said, because the requirements would have meant extra costs for the industry when standards already in effect work “extremely well” at reducing pollution.
Hirsch also said the agency under Trump is protecting the environment, pointing to action the administration has taken to called PFAS, prevent lead poisoning, strengthen chemical safety, and protect Americans’ food and water supply.
“We are building a future where the next generation of Americans is the healthiest in our nation’s history, and they inherit the cleanest air, land and water in the world,” Hirsch said.
However, the administration has taken several steps that environmental advocates say weaken health protections.
The president’s executive order on glyphosate, an herbicide the World Health Organization has linked to cancer, which touched off a who said they felt betrayed. The EPA has decided to stop considering the of reducing pollution when making policy decisions, instead focusing on the cost to industry of complying with rules. The agency also rescinded the legal and scientific basis that had long established as dangerous to public health.
The actions have rankled some MAHA enthusiasts who counted on the administration to tackle chronic disease, especially among children. A petition to Trump on with more than 15,000 signatures called for the removal of EPA Administrator Lee Zeldin, it said supported corporations over MAHA goals.
Some MAHA enthusiasts have sounded off on social media.
“No one should believe that MAHA is being upheld at the EPA at this point,” , a leader of American Regeneration, which focuses on a conservation approach to farming, said Feb. 8 on X.
, host of a , also aired her concerns on X, saying “there is something really freaking spooky going on at the EPA and I refuse to let the American people be gaslit into thinking they’re upholding the MAHA agenda.”
“A significant number of people who supported Trump are worried these rollbacks are going to hurt their health,” said , a Democratic strategist and the founder of the communications firm Third Degree Strategies. “The MAHA voters, especially women, are very sensitive to this. Republicans have put themselves in a bind.”
MAHA supporters shouldn’t be surprised by a Trump administration that doesn’t prioritize environmental protections over industry, because the president has always championed fossil fuels, said Kyle Kondik, managing editor of Sabato’s Crystal Ball, a nonpartisan election forecasting newsletter published by the University of Virginia Center for Politics.
The coke plant exemptions have disappointed some community members, environmental groups, and regulators concerned about public health and emissions.
Nearly 300,000 people live within 3 miles of the 11 active coke plants across the U.S., according to EPA data compiled by the Environmental Defense Fund.
Weakening environmental rules has helped boost Trump with the U.S. coal industry. In February, mining industry executives and lobbyists gathered at the White House, .
Coal miners, including some in white hard hats bedecked with American flags, with a bronze-colored trophy emblazoned “The Undisputed Champion of Beautiful Clean Coal.”
At the event, Trump praised their work. “We love clean, beautiful coal,” he said.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/clairton-pennsylvania-us-steel-make-america-healthy-again-maha-coal-coke/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178095&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>That monthly total is $200 higher than what he paid last year, due in part to the expiration in December of covid pandemic-era premium tax credits. But the self-employed St. Louis property manager isn’t in any hurry to investigate a new type of coverage that might be cheaper than his marketplace plan: farm bureau health plans.
“Although I’m not a fan of rising costs, I’m not going to sacrifice coverage for my kids to save a buck,” Carlton said.
Carlton finds himself among a growing number of Americans who have confronted difficult choices because of rising Affordable Care Act premiums and other affordability issues. For instance, a found that many returning marketplace enrollees reported higher costs this year.
In addition, most expressed worry about affording routine and unexpected medical care, as well as the cost of prescription drugs. Worries were greater among those with lower incomes and chronic health conditions. And about 5% of respondents said they had switched to some type of non-ACA coverage.
Health policy experts say such concerns are giving new legs to alternative forms of coverage — for instance, farm bureau plans.
As of this year, that allow health coverage through state farm bureaus, grassroots membership organizations that advocate for the agricultural industry and rural interests. An annual membership in the bureau typically costs $30 to $50, and in many of the states anyone can join. With membership comes the option of buying into the health plan.
Plan details vary by state, but they typically share many features of marketplace plans, including coverage of a wide range of services, a broad practitioner network, and a way to file complaints.
But because states have passed laws exempting from health insurance requirements, they don’t offer many of the coverage protections provided by insurance. That means their benefits and coverage rules may be less generous or predictable than Obamacare plans.
Crucially, farm bureau plans don’t have to accept everyone who applies for coverage. People must pass underwriting first, a process in which plans evaluate applicants’ medical history and health conditions and decide whether to offer them coverage. This practice was routine before the ACA passed, and people were often rejected due to preexisting medical conditions.
Because farm bureau plans can turn down people with expensive chronic conditions or a history of cancer or other medical issues, farm bureau plans may be than unsubsidized marketplace plans, plan managers say.
As people struggle to keep family farms afloat, they may face Obamacare premiums totaling thousands of dollars a month, leading some to forgo coverage, said Missouri Farm Bureau president Garrett Hawkins.
“We’re trying to present another option,” he said.
Sowing Choices
In 2026, with the expiration of enhanced premium tax credits, average ACA premium payments were estimated to for subsidized enrollees who retained their marketplace plan, according to KFF.
Last year, was one of four states that passed laws permitting farm bureau health plans. The others were , , and .
Although the number of states offering them has ticked up in recent years, farm bureau health plans aren’t new. Tennessee has been offering the coverage . Tennessee’s Farm Bureau Health Plans administers the plans in 10 of the 14 states that permit them.
In Missouri, the farm bureau offers with varying deductibles, copayments, and annual limits on out-of-pocket spending. Many of the benefits and cost-sharing amounts look like the coverage someone might get on the state health insurance exchanges or through an employer. They include emergency care and hospitalization, physician office visits, prescription drugs, free preventive care, and dental and vision services. Members have access to providers through the UnitedHealthcare Choice Plus national network.
Hawkins said he’s pleased with the interest the plans are generating. People could apply for coverage through the website starting Jan. 1, and by mid-March, 520 people had submitted applications, he said.
It’s uncertain how many of those people will clear the underwriting hurdle and buy a farm bureau plan, however. Farm bureau health plans can deny coverage for any reason. Even if coverage is offered, plans in Missouri don’t cover any for at least six or 12 months. In addition, plans may exclude coverage of any benefits related to a “known risk” for two to seven years, depending on the issue. So people with a range of conditions, such as diabetes, high cholesterol, heart problems, or successfully treated cancer, may be turned down or have to pay out-of-pocket for any related care for at least a year and possibly as long as seven years.
“People don’t like that we underwrite, but if we did everything like the ACA, we’d be just like an ACA plan,” said , general counsel and chief compliance and privacy officer at Tennessee’s Farm Bureau Health Plans. “We’re trying to be an option for folks that would otherwise not have coverage.”
Staying Rooted in Coverage
Under the Missouri law, once someone is covered by a farm bureau plan, they can’t be kicked off or charged a higher rate if they get sick. That’s also true for the nine other states where Tennessee administers the plans, Beard said.
“We do not contractually have the right to raise premiums or cancel plans based on [an individual’s] health experience,” he said.
And yet, “it can be really confusing to people” because the plans look like insurance products, but they don’t have the same protections, said , principal for policy development, access to, and quality of care at the American Cancer Society Cancer Action Network.
Someone with a history of cancer would be unlikely to get approved for a farm bureau plan in the first place, Howard said. If they were accepted, the services they might need would likely be excluded from coverage, she said.
“We’re just concerned that there’s going to be more people enrolled in these plans now because there’s so many more states that are allowing them,” Howard said.
Carlton, the self-employed property manager, knows firsthand how underwriting can limit coverage options. Before the Affordable Care Act required that anyone be accepted regardless of health status, Carlton, who has diabetes, had to buy coverage through his state’s high-risk pool, which was often the only option for people with preexisting conditions.
Meanwhile, policy experts share Howard’s concerns.
Insurance companies in the ACA marketplaces “have to offer maternity coverage, and they have to give you benefits on day one for a preexisting condition, and they can’t charge you more because you have that condition,” said , vice president for health policy at the Center on Budget and Policy Priorities. This creates an uneven playing field for insurers and drives up premiums for the people who can’t get into farm bureau plans.
Farm bureau plans “get to use, you know, the standard market as a high-risk pool, essentially, if they want to,” Lueck said.
Still, with the huge jump in premiums that many people are facing for ACA coverage, it’s easy to understand the appeal of farm bureau plans.
“I’m not saying it’s a good thing that states have abdicated their regulatory responsibility here,” said , co-director of the Center on Health Insurance Reforms at Georgetown University. “I’m just saying that there are a lot of people out there who are struggling, who need health care, and simply can’t afford the premiums in these ACA marketplaces anymore.”
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here to contact Ñî¹óåú´«Ã½Ò•îl Health News and share your story.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/farm-bureau-plans-less-pricey-alternative-aca-coverage-tradeoffs/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174986&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>MARQUETTE, Mich. — Providing abortions was the last thing Shawn Brown thought she’d be doing when she opened an urgent care clinic in this remote town in Michigan’s Upper Peninsula.
But she also wasn’t expecting the Planned Parenthood in Marquette to shut down last spring. Roughly 1,100 patients relied on that clinic each year for cancer screenings, IUD insertions, and medication abortions. Now the area has no other in-person resource for abortions. “It’s a 500-mile stretch of no access,” Brown said.
So the doctor, who describes herself as “individually pro-life,” added medication abortions to Marquette Medical Urgent Care’s already busy practice, which treats a steady flow of kids with the flu, college students with migraines, and tourists with skiing injuries.
At least 38 abortion clinics shut down last year in states where they’re still legal, according to data collected by , a project supported by a number of nonprofits that helps people find abortion options. Even states that recently protecting abortion rights, such as Michigan, have had clinics close since the U.S. Supreme Court overturned Roe v. Wade in 2022. And as shutter , patients are losing access to pregnancy care. “You cannot have a high-risk pregnancy up here,” Brown said. “It’s a scary place.”
Now communities are coming up with alternatives, such as Brown’s urgent care.
The idea that urgent cares “could be an untapped solution to closures for abortion clinics across the country is really exciting,” said Kimi Chernoby, the chief operating and legal officer at , a national nonprofit that works to improve professional training and patient outcomes for women in emergency medicine.
One patient at the Marquette urgent care on a recent day was a woman whom Ñî¹óåú´«Ã½Ò•îl Health News agreed to identify by only her first initial, “A,” to protect her medical privacy. She drove more than an hour on snowy backroads while her kids were in day care to get to her appointment.
Her youngest is still a baby, A said, and she got pregnant again while taking the progestin-only birth control pill, which is less likely to interfere with breast milk production but slightly less effective than the regular pill.
“Financials, housing, vehicles — it’s a lot,” she said. And another baby is “just not something that we could really do even at this time.”
She said she was making the long round trip because receiving abortion care in an office felt more secure than being treated by “someone that I’ve never met, or receiving meds that were just shipped to me.”

Face-to-Face Care
In one of the urgent care’s exam rooms, A sat in a chair against the wall, waiting quietly for the doctor. Viktoria Koskenoja, an emergency medicine physician, knocked on the door and then greeted her warmly, pulling up a stool across from her.
“Are you confident in your decision that you want to go ahead? Or do you want to talk about options?” she said.
“No, I’m pretty set on it,” A said.
Koskenoja previously worked at Planned Parenthood. When she learned its Marquette clinic was closing, she started crying and making calls. She recalled asking everyone she knew in health care in Marquette: “What are we going to do?”
One of her first calls was to Brown, a friend and fellow emergency medicine doctor. Their families harvest maple syrup together each spring.
In the wake of the Planned Parenthood closure, Koskenoja convened a community meeting downtown at the Women’s Federated Clubhouse, an 1880s-era building where guests sip from gold-rimmed china teacups on lace tablecloths. The goal: brainstorm new ways to provide abortion access in the Upper Peninsula.
officials said that growing financial challenges and the Trump administration’s cuts to funding, including for the public insurance program Medicaid, had prompted the closures of some brick-and-mortar clinics in the state.
Plus, the availability of pills by mail exploded after the 2022 Dobbs v. Jackson Women’s Health Organization decision overturned Roe. As abortion became illegal in many states, telehealth abortions went from 5% of all abortions provided to 25% by the end of 2024, , a national reporting project that tracks shifts in abortion volume.
Planned Parenthood of Michigan’s telehealth appointments increased 13% for patients in the Upper Peninsula after the Marquette location closed, said Paula Thornton Greear, president and CEO of Planned Parenthood in the state.
All the abortion patients Koskenoja sees at the urgent care have one thing in common: They want to talk to someone in person.
“I had a patient order the pills online and then get scared to use them because they felt like they were going to screw it up, or they weren’t sure they could rely on the pills,” she said. “So they literally came in here with the pills in their hand.”
Others have medical complications or need an ultrasound to determine how far along they are with the pregnancy.
“It annoys me that telehealth is considered an acceptable thing in rural areas,” Koskenoja said. “As though we’re not the human beings that like talking to human beings and looking someone in the eye, especially when something serious is going on.”


The Urgent Care Option
The options presented at that community clubhouse meeting were limited. The few family medicine doctors and OB-GYNs in the area were either already putting patients on months-long waitlists or were too “rightward leaning,” Brown said.
But urgent cares are designed to fill gaps in the system, she said, ready to take walk-ins who aren’t already patients.
Brown knew from her years in the emergency room that medication abortions aren’t that complicated. The for first-trimester and are essentially the same: one dose of mifepristone, followed by misoprostol after 24 to 48 hours.
“Clinically, I was never worried about it,” she said.
The biggest hurdle was getting medical malpractice insurance, Brown said. At first, insurers balked, demanding “onerous and unrealistic” documentation and additional training, she said. Then they quoted a $60,000 annual premium for medication abortions — about three times the cost of insuring the entire urgent care. Ultimately, Brown said, the urgent care’s broker pushed back, providing data that medication abortions didn’t add “significant liability.”
The company agreed to a premium of about $6,000 per year, she said.
The community pitched in, too. A local donor covered an ultrasound machine. And supporters started a nonprofit to help pay for the costs of the medication and additional staffing, bringing the price for patients down from about $450 to an average of about $225, based on a sliding scale.
Word spread quickly once Marquette Medical began offering medication abortions, Brown said. Now the office provides as many as four per week, with patients traveling from as far away as Louisiana. The clinic is on track to match the volume of abortion patients treated at the local Planned Parenthood office before its closure, Brown said.
As pills by mail become the next major target for abortion opponents, Chernoby said, it will be critical to offer more care in more brick-and-mortar places. Brown said the Marquette clinic has already fielded questions from a large academic medical center that plans to start providing medication abortion at its own urgent cares later this year.
“It’s a wonderful idea, but it’s potentially got major pitfalls,” said David Cohen, a professor at the Drexel University Kline School of Law who studies abortion access.
Urgent cares that provide medication abortion would have to abide by state-specific laws — some mandate 24-hour waiting periods or facility structural requirements — and federal regulations, such as the FDA’s requirement that mifepristone prescribers be certified by the drug’s distributors and obtain signed patient agreements.
If abortion access isn’t a core part of a health organization’s mission, “do you want to be on that list? I don’t know if you do,” Cohen said. “There’s just a very particular regulatory environment” around abortion.

Making a Choice
In the exam room, Koskenoja listened as A talked about why she decided to seek an abortion. She has four kids at home, including the baby.
“You OK if we do an ultrasound, just confirm how far along you are, make sure it’s not an ectopic pregnancy?” Koskenoja asked.
“Yeah,” A said.
Koskenoja noted A’s reaction to the question. “OK. You’re making a face?”
“Yeah, I just don’t — yeah, it’s fine. I just don’t want to see it.”
“Oh, you don’t have to see it,” Koskenoja said.
“I just don’t want to hear a heartbeat or anything like that,” A said.
“Definitely not,” Koskenoja said.
After the ultrasound, Koskenoja stepped out into the hall to give A time to call her partner.
When A said she was ready, Koskenoja stepped in and asked her how she was feeling. A had made up her mind. She said that her partner would be supportive of whatever she decided and that she didn’t want to have another baby right now.
“As much as I know this baby would be loved no matter what, it’s just not a good time,” A said quietly, her hands in her lap.
“Most people who get abortions love babies,” Koskenoja said. And you can still have more in the future, she assured A.
This kicked off a long conversation about the mental load of parenting and the pros and cons of various birth control options. A said she wanted to get her tubes tied, but Koskenoja suggested her partner consider a vasectomy instead. It’s a much less invasive procedure, she said. “You’ve had a lot of kids. I feel like it could be his turn to take some responsibility.”
Koskenoja handed her a small, handsewn “comfort bag” that all medication abortion patients receive. It was filled with the pills, reminders about when to take them, a handwritten note of support from local community members, pain meds, comfortable socks, and a heating pad.
“Call us if you need anything,” she told A. “Any questions?”
“No,” A said.
“OK. Good luck,” Koskenoja said before A walked out past the waiting room, filled with sick babies and other patients, to drive back to her kids.
This <a target="_blank" href="/health-care-costs/abortion-providers-clinics-closing-urgent-care-michigan-upper-peninsula/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174428&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>A mom of seven, Pipe is a doula on the reservation who supports new and expectant parents. She does that work free, around her day job. That’s because in this town of about 2,000 people, the closest hospital that delivers babies is 100 miles away.
“Women need this help,” Pipe said.
Doulas ready parents for childbirth, support their deliveries, and can be a steady presence in a baby’s first months. their work with lower rates of costly birth and postpartum complications — especially in hard-to-reach places like Lame Deer.
But that help can be scarce. As Pipe put it: “Doula doesn’t pay the bills around here.”
Things were supposed to change this year. Montana was set to join that reimburse doulas through their Medicaid programs to ease gaps in care. Montana lawmakers approved the payments last year, authorizing up to $1,600 per pregnancy. Pipe hoped that money would give her the chance to leave her post office job one day to help more parents.
But the state Department of Public Health and Human Services postponed adding doula services to its Medicaid program in late March, citing a budget shortfall driven in part by higher-than-expected Medicaid costs.
“DPHHS will not be moving forward with the implementation of doula services in the Montana Medicaid benefit package at this time,” department spokesperson Holly Matkin told Ñî¹óåú´«Ã½Ò•îl Health News.
The news caught Pipe by surprise — she hadn’t heard any updates in a while, but the state had finalized its licensing rules for doulas in January. Last year, she supported three people through their deliveries. She doesn’t have time for much more. That weighs on her. the people on the Northern Cheyenne Indian Reservation , and the people she helps usually can’t afford to pay a doula.
“I was looking forward to serving more people,” Pipe said. “Now that’s not going to happen anytime soon.”


Charlie Brereton, who heads the health department, told state lawmakers in March that the agency projected a $146.3 million shortfall in federal Medicaid funds for this year. Health officials predict another deficit next year as states feel the effects of Republicans’ massive tax-and-spending law, the One Big Beautiful Bill Act. Signed last year, that law is projected to reduce federal Medicaid spending by nearly $1 trillion over 10 years.
Matkin said it’s “unclear” whether the agency can authorize doula coverage this year. The deficit will lead the department to seek supplemental funding from state lawmakers. When an agency makes that kind of request for the first year of the state’s two-year budget cycle, requires it to create a plan to reduce its spending.
Around the country, optional Medicaid services — such as doula support, home health care, and dental work — are at risk of losing funding as states brace for federal Medicaid cuts to hit their bottom lines. Already, lawmakers in Idaho are considering their own reductions to Medicaid to balance the state’s budget. cutting tens of millions of dollars in services for people with disabilities.
In Montana, doula services are unlikely to be the only Medicaid cutbacks announced. “All options are on the table,” Brereton told lawmakers in March.
Stephanie Morton, executive director of Healthy Mothers, Healthy Babies-The Montana Coalition, said more than half of Montana’s counties are designated as maternity care deserts.
“Budget cuts will continue to diminish the limited services families rely upon in these counties,” said Morton, whose nonprofit had advocated for doula Medicaid reimbursement. “This decision feels like the first of many rollbacks and cuts Montanans will face.”
Laboring Alone
At the check-in just outside town, Pipe handed a waking newborn to his mother and unwrapped a new swaddle for the child. This would have to be a quick visit — she was already late for work.
The mother, Britney WolfVoice, held her newborn son as her three young daughters stood close by. Pipe has been with WolfVoice and her husband for the birth of their newborn son and youngest daughter.
She helped them create delivery plans. For the birth of WolfVoice’s youngest daughter a few years ago, Pipe brought cedar oil, a sacred plant used for prayer, and calmed WolfVoice through her contractions. For the recent birth of her son, when hospital backlogs delayed WolfVoice’s induction, Pipe encouraged her to advocate for an earlier appointment by routinely calling the hospital. Doctors had recommended the procedure to avoid complications.
“Misty is one person who I can count on to be my voice,” WolfVoice said.
If someone needs a ride to a doctor’s appointment, Pipe takes time off work to drive them. If a client goes into labor when Pipe’s at the post office, she texts two other free doulas she knows of on the reservation to see if they have time to help until her shift ends. But they also have day jobs.
Pipe herself has ridden that 100-mile stretch between home and the hospital in labor and in the back of an ambulance. Twice, she gave birth in emergency rooms along the way. In one of her pregnancies, she miscarried at home and couldn’t get a doctor appointment for days.
The long distance to receive care often meant her husband had to stay behind to tend to their other children at home.
“I labored alone so many times,” Pipe said. “I just want to make sure no one’s alone.”

Rural maternity care deserts are a , especially as labor and delivery units continue to shutter. In many tribal communities, a lack of care coincides with long-standing inequities caused by centuries of .
Predominantly Indigenous communities face the longest distances to obstetric facilities compared with all other racial and ethnic groups, according to a 2024 report from the March of Dimes. That’s part of the reason Indigenous women are far more likely to get sick from pregnancy and as white women.
Indigenous patients are supposed to be guaranteed access to health care through the federal Indian Health Service. But the chronically underfunded agency has severe gaps. A small fraction of its hospitals and clinics offer labor and delivery. As of 2024, only seven states had either an IHS or tribal birth facility, . To help fill in those shortfalls, Medicaid is the for many Native Americans, according to KFF.
Even where care exists, Native women can experience a distrust of health systems, according to Pipe and other health workers. The U.S. government has a long history of removing children from tribal homes and forcing Native American women to undergo sterilization.
of the Pacific Institute for Research and Evaluation’s Southwest center has studied premature deaths among Native Americans. A member of the Fort Sill-Chiricahua-Warm Springs-Apache Tribe, Haozous said data on maternal health disparities in pregnancy and postpartum often misses a key point.
“It’s not that women are just not taking care of themselves,” Haozous said. “The system is set up for them to not have access to care.”

On top of funding cuts, the One Big Beautiful Bill Act will add more frequent eligibility checks and work requirements to access Medicaid. Those changes, when they take effect later this year and next, will lead an estimated 5.3 million people to lose their coverage by 2034.
Native Americans are exempt from some of the law’s new rules, such as the work requirements. Even so, tribal patients can get tangled in administrative hurdles. That includes struggling to enroll in the first place or to prove their tribal status. A full-time college student, WolfVoice said that when she got pregnant, it took about six months to enroll in the state’s Medicaid program.
Despite Montana’s long struggle with a backlogged Medicaid system, state officials aim to implement work requirements this summer, well before the federal deadline.
‘Moccasins on the Ground’
As Pipe pulled into her driveway one day after a full shift at the post office, her kids ran to her. She was also greeted by Felicia Blindman, a 63-year-old public health nurse who used to work for the tribe. The two sat in lawn chairs into the night and brainstormed ways to connect more women to services — such as free prenatal classes.
Pipe’s four youngest children played around them. Her 14-year-old daughter is already certified as an Indigenous doula. Her 8-year-old daughter has begun helping Pipe pick up prescriptions for moms without a car who live out of town. Pipe hopes one day they could do that work full-time, if they want to.
Because of the lost Medicaid payment, Pipe said, she will continue to balance her job with her birth work, even if it means persuading more people to become doulas, such as family and respected community members, to cover more ground.
“It’s not going to stop me from training more birth workers, more young people, more aunties,” Pipe said. “For now, I guess it’s more about grassroots, moccasins on the ground, helping each other.”
She said that means telling pregnant people who walk into the post office she’s there to help if they need support. At least, as long as she’s not at her day job.

This <a target="_blank" href="/health-care-costs/doula-care-indigenous-health-medicaid-cuts-montana-tribe/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2176418&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>More changes lie ahead that make it important for those getting subsidies in 2026 to track their income and take steps to protect against that kind of financial hit.
First, the basics of how the subsidies work.
Enrollees pay a percentage of their household income toward their health insurance premiums based on a sliding scale, ranging in 2025 from nothing for very low-income people to 8.5% at higher income levels. Subsidies, usually paid directly to insurers, cover the rest.
The income calculation done during open enrollment is an estimate of what a household thinks it will earn in the coming year. At tax time, ACA enrollees must reconcile what they received in subsidies with what they actually earned. If their income rose, they might owe some of the subsidies back.
But don’t skip filing! People who get ACA subsidies must file tax returns no matter their income, and that is becoming even more important: The Trump administration people from subsidy eligibility if they have gone two consecutive years without filing, and it is proposing lowering that to one year.
Beware Surprise Tax Bills
All enrollees who received subsidies for ACA coverage in 2025 — — need to include a special form, the , with their tax filings. That form is used to reconcile a person’s actual income with the amount of subsidies they received, information the IRS mails them on a separate, . Subsidy amounts are based in part on the income projections they made when they enrolled in their ACA plans.
And that can lead to surprises. Some may find they get money back if their income was less than they estimated. But, if their income went above their initial or updated estimates, they probably qualify for less in assistance and will have to pay money back.
Groups that help people file their taxes say it’s not always easy for people to accurately estimate their income for the year ahead, especially those who run their own businesses, work multiple jobs, or have work that comes with varying hours.
Clients will say, “I can make anywhere between $20,000 and $45,000 next year. I just don’t know,” said Katie Alexander, director of training and volunteers for the health and economic opportunity program at Pisgah Legal Services, a western North Carolina nonprofit that provides free tax and health insurance help to people with low incomes.
Still, for taxes being filed now for the 2025 tax year, on what many people must repay.
That cap is $375 for a single individual who earned less than $31,300 in 2025, or . The maximum owed under that sliding scale for people whose income is on the higher end of the range is $1,625 for an individual and $3,250 for a family.
There is no repayment cap for people earning more than four times the federal poverty level — totaling $62,600 in 2025 for an individual or $106,600 for a family of three — so they could owe back all amounts that exceeded their eligibility.
“The amount is just so staggering for folks,” Alexander said.
One woman whom Pisgah staff helped with pulling together her taxes for 2025 made just above $50,000, which was more than she initially estimated. Her repayment was capped at $1,625, Alexander said. Without that cap, she would have owed $4,000, a substantial chunk of her annual income.
Plan Ahead: The Rules Will Be Tougher Next Tax Season
Congressional Republicans’ One Big Beautiful Bill Act, signed into law by President Donald Trump last summer, . That means come next year’s tax season, there will be no sliding-scale limit to how much people could owe back in subsidies for 2026 if their income exceeds their projections.
“That’s just going to be absolutely devastating,” Alexander said.
There are at least two other things to keep in mind, both stemming from covid-era enhanced tax credits, which expired at the end of last year because Congress did not extend them. One is that the amount of household income people must pay toward their premiums this year before subsidies kick in has risen to just over 2% on the low end of the income scale and up to nearly 10% for higher-income earners.
The second is that households earning over four times the federal poverty level no longer qualify for ACA subsidies.
The biggest financial hit could be felt by enrollees whose income rises enough during the year to exceed four times the poverty level. In that case, they would owe back all the subsidies they receive in 2026.
And that could be a lot.
In 2025, for example, the average monthly premium for ACA coverage was $619, but the average enrollee received subsidies worth enough to offset all but $74 of that, according to the .
There’s another twist for some. Because the enhanced credits were not extended, people are paying, on average, double the amount toward their premiums this year, so they may be looking to add to their incomes to cover the cost. A found that 43% of people who remained enrolled in coverage this year are planning to work more hours or get additional work to cover those costs.
“That makes sense, but it can also present a risk of being eligible for less subsidy money than they thought, or even mean they would have to repay the entire tax credit,” said Cynthia Cox, senior vice president and director of the Program on the ACA at KFF, a health information nonprofit that includes Ñî¹óåú´«Ã½Ò•îl Health News.
People can update their projected income at the marketplace website as it changes during the year.
Pisgah staff are calling people they’ve worked with and saying, “Please, please, please, if your income changes, call us so we can adjust your income through the marketplace,” Alexander said.
As much as possible, keep track of income during the year. This isn’t easy, especially for workers who don’t have a job with regular paychecks.
“If you’re meeting with a CPA to talk about taxes, have a conversation to make sure you’re making enough money to afford your costs, but not too much to lose eligibility for a subsidy,” Cox said. “Contributing toward a retirement plan or a health savings account can lower part of your income that counts toward subsidy eligibility.”
Others might choose to dial back their work hours or forgo a new client contract.
“If taking that extra shift means putting you over the line of 400% of the federal poverty level and that’s going to cost you $10,000 in repayments, maybe don’t take that shift,” said Jason Levitis, a senior fellow at the Urban Institute who follows ACA and tax policy issues.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here to contact Ñî¹óåú´«Ã½Ò•îl Health News and share your story.
Ñî¹óåú´«Ã½Ò•îl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/tax-tips-aca-affordable-care-act-obamacare-subsidies-income-owing/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174385&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>