More than 80 of his customers who were enrolled in the same Medicare supplemental plan from the insurer Chubb got hit last August with a 45% increase.
“In my 49 years of doing biz as a broker, I’ve never seen a premium increase be effective immediately on everyone, instead of on their policy anniversary,” said Jaggi, whose brokerage scrambled to find more affordable options for clients. The policies pick up deductibles and other costs not covered in traditional Medicare, and without one there is no upper limit on how much a consumer might owe each year.
While 45% was an unusually big jump, Jaggi and other brokers say double-digit premium increases for Medicare supplemental, or Medigap, policies are becoming the norm.
A Chubb spokesperson did not respond to requests for comment on the increase.
More than 12 million people т of those in traditional Medicare т buy a Medigap policy. Others rely on some sort of retiree employer coverage or a different backup. About 13% of people in traditional Medicare don’t have supplemental coverage, according to KFF, meaning they could be vulnerable to large costs if they have a serious illness.
In the supplemental market, following big increases last year, rates appear to be rising again. In early 2026 filings with state insurance commissioners from Aetna, Blue Cross Blue Shield, Cigna, Humana, Mutual of Omaha, and UnitedHealthcare, rate increases for Plan G policies т the most commonly purchased supplement type т ranged from just in the first quarter, according to Nebraska-based consulting firm Telos Actuarial.
“While this is a small dataset across a select number of states, it’s an indication that carriers are looking to correct their premium rates in light of upward pressure on their claims experience,” said Brett Mushett, a consulting actuary with Telos.
Climbing Numbers
Premium rates vary based on the type of coverage chosen, where a beneficiary lives, and their age. For Plan G coverage, beneficiaries paid an in 2023, according to KFF. That amount has likely risen since.
“In some states, like Ohio, Medicare supplements for years would have a 3% to 5% year-over-year increase. Now it’s 10% to 15%,” said Amanda Brewton, owner of Medicare Answers Now, a marketing organization whose clients are sales agents.
In Alaska, Premera Blue Cross raised the premiums on its Plan G policies by nearly 12% for this year, according to rate sheets provided to бюЙѓхњДЋУНвюl Health News by insurance agent Patricia Mack, who said another insurer raised rates by nearly 13%.
For example, a 65-year-old woman who last year would have been charged $172 a month for a Plan G policy would now face a monthly rate of $192, said Mack, who owns Alaska Insurance Benefits in Wasilla.
Premera spokesperson Courtney Wallace said in an email that Medicare makes changes to deductible and copayment rates each year, which affects supplemental plans that cover those increasing amounts.
Wallace also noted that the insurer saw higher medical service use among its members, “which further drove claims costs and ultimately impacted premiums.”
Agents and policy experts blame a range of factors for rising premiums: an increase in the use of medical services by beneficiaries; the aging of the population; increases in labor and medical costs; rules in some states governing Medigap plans; and people’s enrolling in т or getting out of т private Medicare Advantage plans.
“Five years ago, it was exceedingly uncommon to have a carrier with a rate increase of more than 10%. Now it’s very uncommon to see a rate increase below 10%, and it’s not uncommon to see it over 20%,” said Chalen Jackson, vice president for government affairs at Integrity, a Dallas-based company that sells life and health insurance.
Jaggi, who co-owns Jaggi Petry Insurance & Investments in Forsyth, Illinois, along with his daughter, said he eventually found other options for many of those 80-plus clients with the large increase, which came from an insurer that had previously been the lowest-cost option. But it wasn’t easy т and continuing increases are expected.
“These are unbelievable increases,” said Jaggi, who said he is seeing premium hikes exceeding 15% this year across a range of insurers.
Policy experts have outlined possible solutions, including for Congress to cap out-of-pocket costs for Medicare beneficiaries or subsidize the purchase of Medigap coverage.
“Traditional Medicare is the only federal health insurance program without an out-of-pocket cap,” Sen. Ron Wyden (D-Ore.) wrote in an email, adding that the program “needs to be updated and strengthened to protect the Medicare guarantee for American seniors.”
But making changes to Medicare that require congressional approval is unlikely in the current legislative environment, especially because adding an out-of-pocket cap would add costs to the federal budget.
How This Plays Out
People generally qualify for Medicare when they turn 65. Beneficiaries after they initially enroll in the traditional fee-for-service program to purchase a Medigap plan at standard rates without having to answer health-related questions.
Strict rules then kick in around when beneficiaries can enroll in or switch Medigap coverage and options become much more limited, with each one generally involving trade-offs or tough choices.
have what’s known as a “birthday rule,” which requires insurers once a year to allow people enrolled in a Medigap plan to change to different supplemental coverage т usually around their birthdays т without being medically underwritten. Those rules can help consumers, including those with health conditions, to switch.
An additional т Connecticut, Massachusetts, Maine, and New York т require insurers to offer at least one Medigap policy to all applicants either year-round or during an annual enrollment period, depending on the state. Changes are allowed no matter the person’s health.
Another option for those facing high Medigap costs is to leave traditional Medicare and enroll in a private-sector Medicare Advantage plan, which have out-of-pocket caps. But joining one means beneficiaries must generally rely on a set of in-network doctors and hospitals. And if they change their mind and want to go back to traditional Medicare, they have only a 12-month window in which to purchase a Medigap plan without passing health questions. After that, it can be more difficult.
“A lot of people don’t know that if they are in Medicare Advantage for a year, they can get turned down by a Medigap plan or charged really high premiums because of a preexisting condition, which for many people effectively traps them in MA plans,” said , a research associate at the liberal Center for American Progress and co-author of a on the issue.
There are some exceptions. For example, if a Medicare Advantage plan withdraws from a market or leaves the Medicare program, its enrollees can qualify for a supplemental plan without being asked health questions or charged more for having preexisting conditions.
For this year alone, about 2.6 million people when their insurer pulled out of their markets, according to KFF, and more than a million lost coverage for 2025. Many switched to other MA plans, but “somewhere around 440,000 of those people did go to a Medicare supplement policy,” sometimes because there was no other MA plan in their area, said George Dippel, president of Deft Research, a Minneapolis-based market research organization focused on insurance for older people. Deft is part of Integrity, the Dallas company.
Some Medicare experts note that anytime insurers enroll people whose health status they can’t consider т whether because of birthday rules or because their Medicare Advantage plan left the market and thus qualified them for an exemption from medical underwriting т it potentially exposes them to more health care utilization and higher costs, making them more likely to increase premiums across the board to offset the possible financial hit.
Another option mentioned by brokers for people looking to lower their costs is to consider one of the two types of Medigap plans that come with a deductible, which is currently just under $3,000 for a year. Those plans charge far lower monthly premiums than Medigap plans that pick up a much larger portion of annual amounts people must pay toward their Medicare services.
Still, “a lot of people are not comfortable with a $3,000 deductible,” Mack said.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicare/medigap-medicare-advantage-premiums-rate-increase-few-alternatives/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228699&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The lawsuit, settled on confidential terms last year, blamed not only the managers of City Creek Post-Acute and Assisted Living but also the building’s owner, a real estate investment trust, or REIT.
In the year Darby died, City Creek paid CareTrust REIT more than $1 million in rent, while the Sacramento, California, nursing home ran a deficit, court records show.
Federal tax rules ban REITs from running health care facilities, but CareTrust was not an absentee landlord either, according to internal records filed in the case. It chose the nursing home’s management company and required through the lease that the home keep at least 80% of beds occupied. CareTrust granularly tracked how well the home kept to its financial plan, down to the money spent monthly on nurses and food, the records said. And the documents showed that the real estate company kept tabs on government safety inspection findings and Medicare quality ratings.

Both CareTrust and the nursing home operator denied liability for Darby’s death. CareTrust officials said in court papers that it is not involved in day-to-day nursing home decisions or patient care, and that it monitors facilities to ensure nothing jeopardizes rent payments. In a written statement, CareTrust Corporate Counsel Joseph Layne told бюЙѓхњДЋУНвюl Health News: “We are the property owners, not the operators.”
Landlords With Influence
Over the past decade, real estate investment trusts have bought thousands of buildings that house nursing homes, hospitals, assisted living facilities, and medical offices. A бюЙѓхњДЋУНвюl Health News examination of court filings and corporate records shows that these landlords have more influence than the health care facilities publicly acknowledge.
The documents reveal REITs often select the management who oversee the operations and leave them in place even when they are aware of threadbare staffing, floundering governance, repeated safety violations, or other problems that hamper quality of care. A California jury in March awarded $92 million in punitive damages against a former REIT over the death of a 100-year-old resident with dementia who froze to death outside her assisted living facility.
“The REITs are in charge,” said Laraclay Parker, one of the lawyers who represent Darby’s daughter.
Absence of Oversight
Despite their ubiquity, REITs remain invisible to state and federal health regulators. Hospitals and nursing homes are not required to disclose rent payments or landlord identities in the annual reports they submit to Medicare.
Under President Donald Trump, the Centers for Medicare & Medicaid Services a Biden-era requirement that nursing homes . Catherine Howden, a CMS spokesperson, said in a statement that the agency does not regulate facilities based on their tax status or corporate form and instead focuses on the quality of the care they provide.
REITs now of the nation’s senior housing, which includes assisted living, memory care, and independent living, according to an industry analysis. REITs also hold investments in nursing homes. Publicly traded REITs that focus on health care are now worth nearly a quarter of a trillion dollars, according to Nareit, an industry association.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/real-estate-investment-trusts-senior-housing-nursing-homes-profit/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228343&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This year, executives from nearly every major health insurance company made the same declaration in calls with Wall Street analysts: Using artificial intelligence to make coverage decisions would help save them money.
Even the Trump administration is testing AI’s usefulness in managing the prior authorization process for the Medicare program, as well as seeking to override AI regulation by states.
But class action lawsuits have accused insurers of using AI to wrongfully withhold treatment. And outlines the risks of training AI on a current system rife with wrongful denials.
“There is a world in which using AI could make that worse, or at least replicate a bad human system, because the data that it would be training on is from that bad human system,” said Michelle Mello, a co-author of the study.
Although, Mello said, the research team found “real positives alongside the risks.”
In this video produced by бюЙѓхњДЋУНвюl Health News’ Hannah Norman, Darius Tahir, a correspondent covering health technology, explains.
You can read Tahir’s recent coverage of AI’s use by health insurers below:
- “Red and Blue States Alike Want To Limit AI in Insurance. Trump Wants To Limit the States,” by Darius Tahir and Lauren Sausser.
- “AI Will Soon Have a Say in Approving or Denying Medicare Treatments,” by Lauren Sausser and Darius Tahir.
This <a target="_blank" href="/courts/watch-ai-artificial-intelligence-prior-authorization-insurance-coverage-decisions/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2181021&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
At the Trump administration’s request, a federal judge in Louisiana this week agreed to delay a ruling affecting the continued availability of the abortion drug mifepristone. That angered anti-abortion groups that want the drug, if not banned, at least more strictly controlled. But the administration clearly wants to avoid big abortion fights in the run-up to November’s midterm elections.
Meanwhile, the administration’s proposed budget for fiscal year 2027 calls for more than $15 billion in cuts to programs at the Department of Health and Human Services. It’s a significant number, but less drastic than cuts it proposed for fiscal 2026.
This week’s panelists are Julie Rovner of бюЙѓхњДЋУНвюl Health News, Lauren Weber of The Washington Post, Alice Miranda Ollstein of Politico, and Maya Goldman of Axios.
Panelists



Among the takeaways from this week’s episode:
- The Trump administration says it is conducting a thorough scientific review of the abortion pill mifepristone at the Food and Drug Administration. Yet advocates on both sides of the abortion debate think the administration is just trying to buy time to avoid a controversial decision about medication abortion before November’s midterm elections.
- It’s budget time on Capitol Hill. With the unveiling of the president’s spending plan for fiscal 2027, Cabinet secretaries will make their annual tour of congressional committee hearings. HHS Secretary Robert F. Kennedy Jr., whose Hill appearances have been few during his tenure, is scheduled to testify before six separate House and Senate committees before the end of the month.
- Back at HHS, Kennedy appears to be trying to reconstitute the Advisory Committee on Immunization Practices in a way that will enable him to restock it with vaccine skeptics without running afoul of a March court ruling that he violated federal procedures with his replacements last year.
- Continuing his efforts to promote his Make America Healthy Again agenda, Kennedy announced this week that he will launch his own biweekly podcast. He also announced efforts to combat microplastics in the water supply and to get hospitals to stop serving ultraprocessed food to patients.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: The Atlantic’s “,” by Katherine J. Wu.
Maya Goldman: бюЙѓхњДЋУНвюl Health News’ “Trump’s Personnel Agency Is Asking for Federal Workers’ Medical Records,” by Amanda Seitz and Maia Rosenfeld.
Lauren Weber: CNN’s “,” by Holly Yan.
Alice Miranda Ollstein: Politico’s “,” by Simon J. Levien.
Also mentioned in this week’s podcast:
- JAMA Internal Medicine’s “,” by Lauren J. Ralph, C. Finley Baba, Katherine Ehrenreich, et al.
- бюЙѓхњДЋУНвюl Health News’ “Immigrant Seniors Lose Medicare Coverage Despite Paying for It,” by Vanessa G. Sánchez, El Tímpano.
- The New York Times’ “,” by Ellen Barry.
- Stateline’s “,” by Nada Hassanein.
- The Washington Post’s “,” by Lena H. Sun.
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, from бюЙѓхњДЋУНвюl Health News and WAMU Public Radio in Washington, D.C. Welcome to What the Health? I’m Julie Rovner, chief Washington correspondent for бюЙѓхњДЋУНвюl Health News, and I’m joined by some of the best and smartest health reporters covering Washington. We’re taping this week on Thursday, April 9, at 9:30 a.m. As always, news happens fast, and things might have changed by the time you hear this. So here we go.
Today, we are joined via video conference by Lauren Weber of The Washington Post.
Lauren Weber: Hello, hello.
Rovner: Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Hi, everybody.
Rovner: And my fellow Michigan Wolverine this national championship week, Maya Goldman of Axios. Go, Blue!
Maya Goldman: Go, Blue.
Rovner: No interview this week, but plenty of news. So let’s get right to it. We’re going to start with reproductive health. On Tuesday, a federal judge in Louisiana ruled for the Trump administration and against anti-abortion forces in a lawsuit over the availability of the abortion pill mifepristone. Wait, what? Please explain, Alice, how the administration and anti-abortion groups ended up on opposite sides of an abortion pill lawsuit.
Ollstein: Yeah. So this has been building for a while, and it is not the only lawsuit of its kind out there. There are several. A bunch of different state attorneys general, who are very conservative and anti-abortion, have been suing the FDA in an attempt to either completely get rid of the availability of the abortion pill mifepristone or reimpose previous restrictions on it. So right now, at least according to federal rules, not according to every state’s rules, you can get it via telehealth. You can get it delivered by mail. You can pick it up at a retail pharmacy. You don’t have to get it in person handed to you from a doctor like you used to. So these lawsuits are attempting to bring back those restrictions or get the kind of national ban that a lot of groups want. And so you have other ones pending: Florida, Texas, Missouri, you have a bunch of ones. So this is the Louisiana version. And the Trump administration, it’s important to note, they are not defending the FDA or the abortion pill on the merits. They are saying, we don’t want this lawsuit and this court to force us to do something. We want to go through our own careful process and do our own internal review of the safety of mifepristone, and then we may decide to impose restrictions. But they’re asking courts to give them the time and space to complete that process and saying, you know, This is our power we should have in the executive branch. And so, in this case, the judge, in ruling for the Trump administration, basically just hit pause. This doesn’t get rid of the case. It just puts a stay on it for now, and that’s important. In some of these other cases, the Trump administration has asked the courts to throw out the case, but that was not the situation here. So this doesn’t mean that abortion pills are going to be available forever. This doesn’t mean nothing’s going to happen, and they’re going to be banned. This just means, you know, we’re kicking the can down the road.
Rovner: I was saying, just to be clear. I mean, we know that this FDA quote-unquote “study” т whether it is or isn’t going on т is part of, kind of, a delaying tactic by the administration, because they don’t want to really make abortion a big front-and-center issue in the midterms. So they’re trying to sort of run the clock out here. Is that not sort of the interpretation that’s going on right now?
Ollstein: That’s what people on both sides assume is going on. It’s really been fascinating how everyone is being kept in the dark about what’s happening inside the FDA т and if this review is even happening, if it’s real, if it’s in good faith, what is it based on? And so it’s become this sort of Rorschach test, where people on the left are saying, you know, They’re laying the groundwork to do a national ban. This is just political cover. They just want to wait until after the midterms, and then they’re going to go for it. And people on the right are saying, you know, The administration is cowardly, and they aren’t really doing anything, and they’re just trying to get us to shut up and be patient. We don’t know if either of those interpretations or neither of them are true.
Rovner: Lauren, you want to add something?
Weber: I just think it’s pretty clear this is also just on a [Health and Human Services Secretary Robert F.] Kennedy [Jr.] priority. I mean, let’s go back. The man тІ comes from one of the top Democratic political families originally. You know, there’s obviously been a lot of chatter around his anti-abortion beliefs. Now, obviously, he’s on a Republican ticket. I think some of that plays into this as well. And he already has his hand on the stove on so many other hot issues that, [if] I had to guess, I don’t think that they’re trying to rock the boat on this one. тІ I think, some background context too, to some of what’s going on.
Rovner: We’ll get to some of those hotter issues. But, meanwhile, the Journal of the American Medical Association [Internal Medicine] has a suggesting that medication abortion is so safe that it could be provided over the counter т that’s without any consultation with a medical professional, either in person or online. This doesn’t feel like it’s going to happen anytime soon, though, right? While we’re still debating the existence of medication abortion in general.
Ollstein: That’s right. I mean, there are a lot of people who can’t get this medication prescribed by a valid doctor right now, let alone over the counter. I will say it is common in a lot of parts of the world to get it over the counter, whereas in the United States, the most common way to have a medication abortion is with a two-pill combination, mifepristone and misoprostol. In a lot of parts of the world, people just use misoprostol alone, and it is effective and it is largely safe. It’s slightly less safe than using both pills together. And so I think there’s a lot of international data out there, and people point to that and advocate for this. And I will say there are activist groups in the United States who are setting up networks, underground networks, to get these pills to people with no doctor’s involvement. And so that is already going on. I think that a lot of people would prefer to get it from a doctor if they could. But because of bans and restrictions, they can’t. And so people are turning to these activist groups.
Rovner: I will point out, as a person who covered the entirety of the fight to have emergency contraception т which is not the abortion pill т made over the counter, it took like, 15 years. It shortened my life covering that story. Lauren, did you want to add something?
Weber: Yeah, I just wanted to say I find it really interesting. Obviously, reproductive issues end up taking 15 years, as you pointed out, to make it over the counter. But there are a lot of things that are considered potentially more dangerous that you can order up in a pretty basic telehealth visit or even just buy in not-so-sketchy ways that the administration is also even looking to deregulate. So I think the differences of access of this compared to other less studied, potentially more unsafe medication is quite striking.
Goldman: Part of [President Donald] Trump’s “Great Healthcare Plan” is making more medications available over the counter. So this is certainly something that they have said they want to do, in general. This is a political nightmare, though, to do that for abortion.
Ollstein: Yeah, and people have been pointing to this and a lot of other policies for a while to argue about something they call abortion exceptionalism, in which people apply a different standard to anything related to abortion, a different safety standard, a different standard of scrutiny than they do to medications for lots of other purposes. And you’ve seen that, and that comes up in lawsuits and political arguments about this. And I think, you know, people can point to this as another example.
Rovner: So last week, we talked about the federal family planning program Title X, which finally got funded after months of delays. But Alice, you warned us that the administration was planning to make some big changes to the program, and now those have finally been announced. Tell us what the plan is for a program that’s provided birth control and other types of primary and preventive care since the early 1970s.
Ollstein: Well, the changes have sort of been announced. They’ve more been teased. What we are still waiting for is an actual rule, like we saw in the first Trump administration, that would impose conditions on the program. And so what we saw recently, it was part of a wonky document called a “Notice of Funding Opportunity,” or NOFO, for those in the D.C. lingo. And basically it was signaling that when groups reapply т they just got this year’s money, but when they reapply for next year’s money т it sets up sort of new priorities and a new focus for the entire program. And what was really striking to me is, you know, this is a family planning program. It was created in the 1970s and it is primarily about delivering contraception to people who can’t afford it around the country, providing it to millions of people who depend on this program, and the word “contraception” did not appear in the entire 70-page document other than an assertion that it is overprescribed and has bad side effects. And instead, they signaled that they want to shift the program to focus on, quote, “family formation.” So this is really striking to me. I think we saw some signs that something like this was coming. You know, about a year ago, there was some Title X money approved to focus on helping people struggling with infertility. But that was sort of just a subset of the program, and now it looks like they want to make that, you know, an overriding focus of the program. So I think when the actual rule to this effect drops, and we don’t know when that will be т will they wait till after the midterms to, you know, avoid blowback? Who knows? I think there will certainly be lawsuits then. But I think right now, this is just sort of a sign of where they want to go in the future. And it’s important to note that it came very quickly on the heels of a big backlash from the anti-abortion movement over the approval of this year’s funding going out to all of the clinics that got it before, including Planned Parenthood clinics. The anti-abortion groups were agitating for Planned Parenthood to be cut off at once, you know, not in the future, right now.
Rovner: Just to remind people that the ban on Planned Parenthood funding from last year was for Medicaid, not for the Title X program.
Ollstein: Right.
Rovner: And that’s why Planned Parenthood got money.
Ollstein: Yes, and Planned Parenthood is not allowed to use any Medicaid or Title X money for abortions, but the anti-abortion groups say it functions like a backdoor subsidy, and so they wanted it to be cut off. So they were very pissed that this money went out to Planned Parenthood. And so very quickly after, the administration put out this document, saying, Look, we are taking things in another direction, and it is not the direction of Planned Parenthood.
Rovner: Lauren, you want to add something?
Weber: Oh, I just wanted to say Alice has really been owning the beat on all the Title X coverage, so тІ
Rovner: Absolutely.
Weber: тІ glad we are able to have her explain it to us. But just wanted to throw out a kudos for breaking all the news on that front.
Goldman: Yeah, great coverage.
Rovner: Yes. Very happy to have you for this. Turning to the budget, which is normally the major activity for Congress in the spring, we finally got President Trump’s spending blueprint last week. It does propose cuts to discretionary spending at the Department of Health and Human Services to the tune of about $15 billion, but those cuts are far less deep than those proposed last year. And, as we have noted, Congress didn’t actually cut the HHS budget last year by much at all. And many programs, like the National Institutes of Health, actually got small increases. Is this budget a reflection of the fact that the administration is recognizing that cuts to Health and Human Services programs aren’t actually popular with the public or with Congress, for that matter, going into a midterm election?
Weber: I think it’s that last little piece you mentioned there, Julie. I think it’s the “going into the midterm election.” I think you hit the nail on the head there. Cuts are also not good economically for many Republicans. You know, we saw Katie Britt be one of the т the Alabama Republican senator т be one of the most outspoken senators in general about some of the cuts that were floated for the budget for HHS last year. So I think what you’re hinting at, and what we’re getting at, is that it’s not politically popular, it can be economically problematic, on top of the scientific advances that are not found. So I suspect you are right on that.
Ollstein: The administration knows that this is “hopes and dreams” and will not become reality. It did not become reality last year. It almost never becomes reality. And I think you can see the sort of acknowledgement that this is about sending a message more than actually making policy in things like Title X, because at the same time they put out this guidance from HHS about the future of Title X, moving away from contraception, in the president’s budget he proposed completely getting rid of Title X, completely defunding it, which he has in the past as well. And so why would they put out guidance for a program that doesn’t exist?
Goldman: I think, also, this is the second budget that they’re putting out in this administration, right? So now they are just a little more used to what’s going on, and they have more of their feet under them.
Weber: As a preview for listeners, too, I’m sure we will have Kennedy asked about this budget when he appears in a series of so many hearings next week and the week after. And there were a lot of fireworks last year with him and various members of Congress about the budget. So I am sure that we will hear a lot more on this front in the weeks to come.
Rovner: Yeah, I would say that’s one thing that the budget process does, is when the president finally puts out a budget, the Cabinet secretaries travel to all of the various committees on Capitol Hill to, quote, “defend the president’s budget,” which is sometimes or, I guess in the case of Kennedy, one of the few chances that they get to actually have him in person to ask him questions. But in the meantime, you know, we have the budget, then we have the president himself, who at an Easter lunch last week т that was supposed to be private, but ended up being live-streamed т said, and I quote, “It’s not possible for us to take care of day care, Medicare, Medicaid, all these individual things.” The president went on to say that states should take over all that social spending, and the only thing the federal government should fund is, quote, “military protection.” Did I just hear a thousand Democratic campaign ads bloom?
Goldman: I think this is a prime example of when you should take Trump seriously, but not literally. I don’t think that there’s any world, at least in the foreseeable future, where the federal government isn’t funding Medicare. But, you know, you certainly have to watch at the margins. It’s like, it’s not a secret that this is something that they’re interested in cutting back spending on. It’s super politically difficult to do that, and they know that, and that’s part of why, which I’m sure we’ll talk about in a little bit, they bumped up the payment rate for 2027 to Medicare Advantage plans.
Rovner: Which we will get to.
Goldman: Yeah, so I mean, it’s certainly an eye-opening statement, and you should remember it. But I don’t think that we’re in immediate jeopardy here.
Rovner: This is the president who ran in 2024, you know, saying that he was going to protect Medicare and Medicaid. I mean, it’s been, you know, against some of the recommendations of his own administration. I was just sort of shocked to see these words come out of his mouth. Lauren, you wanted to say something?
Weber: I mean, it’s not that surprising, though. I mean, look at what the One Big Beautiful Bill [Act] did to Medicaid. He’s already pushed through massive Medicaid cuts, which are essentially being offloaded to the states. So, I mean, I think this ideology has already borne out and will continue to bear out, and obviously it’s happening amid the backdrop of a war. So that plays into, obviously, the commentary as well.
Rovner: Well, meanwhile, Republicans are still talking about doing another budget reconciliation bill, the 2.0 version of last year’s Big Beautiful Bill, except this time it’s essentially just to fund the military and ICE [Immigration and Customs Enforcement] and border control, because Democrats won’t vote for those things, at least they won’t vote for additional military spending. What are the prospects for that to actually happen? And would Republicans really be able to do it if those programs are paid for with more cuts to Medicare and/or Medicaid, as some have suggested?
Goldman: You know, my co-worker Peter Sullivan wrote about this last week, and there was a lot of blowback from politicos, from advocates, from, you know, kind of across the spectrum of groups there. I think that it would be extremely politically unpopular, especially going into the midterms, to use health care as an offset. But I would say that Republicans are pretty good at rhetoric, right? That’s one of the things that they’re known for right now, and there’s always a way to spin it.
Rovner: Alice and I spoke to a group earlier this week, and I went out on a limb and predicted that I didn’t think Republicans could get the votes for another big budget reconciliation this year. I mean, look at how close it was last year. The idea of cutting any deeper seems to me unlikely, just given the margins that they have.
Goldman: And I think that is something that you do in between election years. That’s not something you do in an election year.
Rovner: That’s true, yes тІ you do tend to see these bigger bills in the odd-numbered years rather than the even-numbered years, but тІ
Ollstein: And I think it’s important to remember that the reason Republicans are in this bind and that they feel like they have to keep reconciliation nearly focused on funding immigration enforcement is because Democrats refuse to fund immigration enforcement. And so they feel pressured to put all their effort and political capital towards that, and don’t want to mess that up by adding a bunch of other health care things that could cause fights and lose them votes.
Goldman: The money has got to come from somewhere.
Rovner: And health care is where all the money is. Speaking of Medicare and Medicaid, where most of the money is, there is news on those fronts, too. Maya, as you hinted on Medicare, the administration is out with its payment rule for private Medicare Advantage plans for next year. And remember, we talked about how HHS was going to really go after overbilling in Medicare Advantage and cut reimbursement dramatically? Well, you can forget all that. The final rule will provide plans with a 2.48% pay bump next year. That’s compared to the less than 1% increase in the proposed rule. That’s a difference of about $13 billion. The final rule also eliminated many of the safeguards that were intended to prevent overbilling. What happened to the crackdown on Medicare Advantage? Are their lobbyists really that good?
Goldman: Their lobbyists are pretty good. This was a year where there were т I think CMS [the Centers for Medicare & Medicaid Services] said there were a record number of public comments on their proposed rate, flat rate increase, flat rate update. But I think it’s also not that surprising. Historically, the final rate announcement for Medicare Advantage is almost always a little higher than the proposed because they incorporate additional data from the end of the previous year that wasn’t available when first rate is proposed, the initial rate is proposed. But certainly they backed away from a big change to risk adjustment, or, like, the way to adjust payment based on how sick a plan’s enrollees are. You get more pay тІ
Rovner: Because that’s where the overbilling was happening, that we’d seen a lot of these wonderful stories that plans were basically, you know, inventing diagnoses for patients who didn’t necessarily have them or didn’t have a severe illness, and using that to get additional payments.
Goldman: Right. And they did move forward with a plan to prevent diagnoses that are not linked to information that’s in a patient’s medical chart from being used for risk adjustment. But a lot of plans had said, like, Yeah, this is, that’s the right thing to do, and it’s not going to be that impactful for us. You know, overall, this is a win for health insurance. I think one thing to note is that Chris Klomp, the director of Medicare, said, We’re still really focused on trying to right-size this program. That’s still a priority for us as an administration, but we also want to safeguard it. And so I think insurers are not off the hook entirely. There’s still going to be a lot of scrutiny, but their lobbyists are pretty good. And you know, no one wants to be seen as the candidate that cuts Medicare.
Rovner: And we have seen this before, that when Congress cuts “overfunding” for Medicare Advantage, the plans, seeing that they can’t make its big profits, drop out or they cut back on those extra benefits. And the beneficiaries complain because they’re losing their plans, or they’re losing their extra benefits, and they don’t really want to do that in an election year either, because there are a lot of people, many millions of people, who vote who are on these plans. So, in some ways, the plans have the administration over a political barrel, in addition to how good their lobbyists are.
Well, apparently, one group that HHS is still cracking down on are legal immigrants with Medicare. Most of the publicity around the health cuts in last year’s budget bill focused on the cuts to Medicaid. But we at бюЙѓхњДЋУНвюl Health News have a story this week about legal immigrants who’ve paid into the Medicare system with their payroll taxes for years and are now being cut off from their Medicare coverage. This is apparently the first time an entire category of beneficiaries are having their Medicare taken away. I’m surprised there hasn’t been more attention to this, or if it’s just too much all happening at once.
Ollstein: I mean, there’s a lot happening at once, and even just in the space of immigrants’ access to health care, there is so much happening at once. And so this is obviously having a huge impact on a lot of people, but so are 100 other things. And I think, you know, the zone has been flooded as promised. And really, state officials who are also dealing with a thousand other things, Medicaid cuts, you know, these federal changes, work requirements, are grappling with this as well.
Rovner: Lauren, you wanted to add something?
Weber: Yeah. I mean, I thought it was, there was a striking quote in the story from Michael Cannon, who basically said, The reason this isn’t resonating is because this won’t upset the Republican base. And I think that’s a striking quote to be considered.
Rovner: Michael Cannon, libertarian health policy expert, just kind of an observer to this one. But yeah, I think that’s true. I mean, or at least the perception is that these are not Republican voters, although, you know, as we’ve seen, you know, Congress has tried to take aim at people they think aren’t their voters, and it’s turned out that those are their voters. So we will see how this all plays out.
Well, at the same time that this is all going on, the folks over at the newsletter “Healthcare Dive” are reporting that the Centers for Medicare & Medicaid Services are trying to embark on all these new initiatives on fraud, and work requirements, and artificial intelligence with a diminished workforce. While CMS lost far fewer workers in the DOGE [Department of Government Efficiency] cuts last year than many other of the HHS agencies т it was in the hundreds rather than the thousands т CMS has long been understaffed, given the fact that it manages programs that provide health insurance to more than 160 million Americans through not just Medicare and Medicaid, but also the Children’s Health Insurance Program and the Affordable Care Act. I know last week, FDA Commissioner Marty Makary said he wants to hire more workers to replace the 3,000 who were RIF’ed or took early retirement there at the FDA. And CMS does have lots of job openings being advertised. But it’s hard to see how replacing trained and experienced workers with untrained, inexperienced ones are going to improve efficiency, right?
Goldman: Tangentially, I was talking to a health insurance executive yesterday who was saying that his team is so much bigger than CMS, and they cover a fraction of the market, and they’re often the ones coming to CMS and proposing ideas and working with CMS on it. I don’t, I think that is a dynamic that far predates this administration, but тІ
Rovner: Oh, absolutely.
Goldman: But it’s certainly interesting. And тІ CMS has very ambitious plans, and not that many people to carry them out. But, you know, I think one thing that I also want to note is that when I talk to trade associations and stakeholders about this CMS, they are generally like, pretty support- тІ like, they say that they think they’re being heard, and they think that CMS and the career staff are doing, you know, the same kind of caliber of work that they’ve been doing, which I think is notable.
Rovner: And as we have mentioned many times, you know, Dr. [Mehmet] Oz, the head of CMS, is very serious about his job and doing a lot of really interesting things. It’s just, it’s hard, you know, in the federal government, if you don’t have the resources that you want to тІ if you don’t have the resources to match your ambitions. Let’s put it that way.
Well, meanwhile, on the Medicaid front, we’re already seeing states cutting back, and some of the results of those cutbacks. on how psychiatric units are at risk of being shut down due to the Medicaid cuts, since they often serve a disproportionate number of low-income people and also tend to lose money. And The New York Times has a of an Idaho Medicaid cutback of a program that had provided home visits to people living in the community with severe mental illness, until those people who lost the services began to die or to end up back in more expensive institutional care. Now the state has resumed funding the program, but obviously will end up having to cut someplace else instead. I know when Republicans in Congress passed the cuts last year, they said that people on Medicaid who were not the able-bodied working-age populations wouldn’t see their services cut. But that’s not how this is playing out, right?
Weber: I just think the story by Ellen Barry, who you should always read on mental health issues in The New York Times, “,” is such an illustrative example of unintended consequences from these cuts. And the reason that they’re being reversed т by Republican legislators, no less т in Idaho, is because it’s more expensive to have cut the money from it than it is efficient. I mean, what they found was, is that after they cut the money to the schizophrenia program, they saw this massive uptick in law enforcement cases and hospitalizations, uninsured hospitalizations, that this avoided. And I think it’s a real canary in the coal mine situation, because we’re only starting to see these states cut these things off. And this was a pretty immediate multiple-death consequence. And I think we’re going to see a lot of stories like this, of a variety of programs that we all don’t even have any idea that exist in the safety net across the country that are being chipped away at.
Rovner: Well, turning to other news from the Department of Health and Human Services, we’re getting some more competition here at What the Health? Health secretary Kennedy has announced he’ll be unveiling his own podcast, called The Secretary Kennedy Podcast, next week. He promises to, according to the trailer posted online on Wednesday, quote, “name the names of the forces that obstruct the paths to public health.” OK then, we look forward to listening.
Meanwhile, in actual secretarial work, the secretary this week also unveiled changes to the charter of the Advisory Committee on [Immunization] Practices after a federal judge last month invalidated both the replacement members that he’d appointed last year and the changes made to the federally recommended vaccine schedule. So what’s going to happen here now? Will this get around the judge’s ruling by watering down the expertise that members of this advisory committee are supposed to have in vaccines? And why hasn’t the administration appealed the judge’s ruling yet?
Goldman: You know, I don’t have actual answers to this, but I do wonder and speculate that this is going to end up being some kind of legal whack-a-mole situation where the secretary and HHS says, OK, you don’t like it that way? We’ll do it this way, and then they’ll do it another way, and advocates will sue, and we’ll see how this plays out going forward in the courts. I think this is not the end of the story. Even though the judge’s decision was a big win for vaccine advocates, it’s just we’re in the midpoint, if that.
Rovner: And Lauren, speaking of vaccines, your colleague Lena H. Sun has on HHS and vaccine policy.
Weber: Yeah, Lena Sun is always delivering. She found out that the acting director of the CDC [Centers for Disease Control and Prevention] at the time delayed publication of a report showing that the covid-19 vaccine[s] cut the likelihood of emergency department visits and hospitalizations for healthy adults last winter by about half. So even though Kennedy is not talking more about vaccines, it appears that, based on this reporting, that some of his underlings are not necessarily touting the benefits of vaccine, so to speak. And I’m very curious, going back to Kennedy’s podcast, I found the rollout of that so interesting because the teaser was very leaning into the Kennedy that got elected, you know, someone who speaks about, you know, dark truths that are hidden from the public, and so on. And then the press team had these statements of, like, Kennedy will investigate the affordability of health costs and food and nutrition. And I think this dichotomy of who Kennedy is and who the White House and the press secretary and HHS want Kennedy to be before the midterms really could come to a head in this podcast. So I think we will all be listening to hear how that goes.
Rovner: Yeah, we keep hearing about how the secretary is being, you know, sort of put on a leash, if you will. And, you know, told to downplay some of his anti-vaccine views and things like this. And that seems quite at odds with him having his own podcast. Alice, do you want to тІ?
Weber: I guess, it depends on who’s editing the podcast and who they have on. I’m just very тІ you could even tell from the trailer to how his press secretary presented it, there was an interesting differential in framing, and I am curious how that plays out as we see guests on it.
Ollstein: I mean, it’s also worth noting that this is an administration of podcasters. I mean, you have Kash Patel, you have so many of these folks who have a history of podcasting, clearly have a passion for it, just can’t let it go while working a full-time, high-pressure government job.
Rovner: We shall see. Meanwhile, HHS, together with the Environmental Protection Agency, is waging war on microplastics, those nearly too impossible to detect bits of plastic that are getting into our lungs and stomachs and body tissues through air and water and food. The plan here seems to be to find ways to detect exactly how much microplastics we are all getting in our water and what the health impacts might be, since we don’t have enough information to regulate them yet. I would think this would be one of those things that pleases both MAHA [Make America Healthy Again] and the science community, right? Or is it just, as one MAHA supporter called it, theater?
Goldman: I think this is a great example of the, you know, part of the reason why MAHA is so interesting to such a wide swath of people. Like, there’s a lot of legitimate concern, not that other concerns aren’t necessarily legitimate, but there’s a lot of concern over, from the scientific community, over microplastics. I’m honestly surprised that we’re this far into the administration with this announcement. I would have thought that this is something they would have done sooner, but they obviously had other priorities as well.
Rovner: Well. Finally, this week, speaking of other priorities, HHS Secretary Kennedy and CMS Administrator Dr. Oz are declaring war on junk food in hospitals. Again, this seems like a popular and fairly harmless crusade; hospitals shouldn’t be serving their patients ultraprocessed food. Except, almost as soon as the announcement came out, I saw tons of pushback online from doctors and nurses who worried about patients for whom sugary food or drinks are actually medically indicated, or who, because of medications they’re taking, or illnesses they have, can only eat, or will only eat, highly palatable, often processed food. Nothing in health care is as simple as it seems, right?
Weber: I think what’s also interesting is one of my favorite examples in the memo they put out was they hope that every hospital, as an example, could serve quinoa and salmon. And I just am curious to see how fast that gets implemented. And it’s a very valid т a lot of people complain about hospital food. It’s a very valid thing to push for better food. But I also question, as I understand it, this seems more like a carrot than a stick when it comes to the regulation they put out.
Rovner: As it were.
Weber: As it were. And so I’m curious to see how it gets implemented. That said, there are hospitals that have taken it upon themselves т the Northwell [Health] example in New York is a good example т to really improve their hospital food. And frankly, it’s a money maker. If your food’s better, people come to your hospital, especially in an urban area where there is hospital competition. So you know, like most MAHA topics, there’s a lot of interesting points in there, and then there’s a lot of what’s the reality and what’ actually going to happen. And so I’ very curious to see how this continues to play.
Rovner: I did a big story, like, 10 years ago on a hospital chain that had its own gardens, that literally grew its own healthy food. So this is not completely new but, again, interesting.
All right, that is this week’s news. Now it’s time for our extra-credit segment. That’s where we each recognize a story we read this week we think you should read, too. Don’t worry if you miss it. We will post the links in our show notes on your phone or other mobile device. Alice, why don’t you start us off this week?
Ollstein: I have a piece from my co-worker Simon [J.] Levien, and it is called “.” This is about thousands of doctors around the country who are from other countries that are placed on, you know, a list by the Trump administration of places where they want to scrutinize and limit the number of immigrants coming from there. And so these are people who are already here, already practicing, have poured years into their training, have been living here, and, in some cases, are the only folks willing to work in certain areas that have a lot of medical shortages, and they just can’t practice because their paperwork isn’t getting processed in time. And so they’re sort of in this scary limbo, and that’s putting these hospitals and clinics that they work in in a really tough bind. And so they’re hammering the Trump administration to give them answers about what their fate is. You know, they’re not trying to deport them yet, but they’re not allowing them to continue working either.
Rovner: For an administration that’s been pushing really hard to improve rural health care, this does not seem to be a way to improve rural health care. Maya.
Goldman: My extra credit this week is called “Trump’s Personnel Agency Is Asking for Federal Workers’ Medical Records.” It’s a great KFF Health News scoop from Amanda Seitz and Maia Rosenfeld. It’s a really great example of the administration, you know, sort of moving in silence, doing these small regulatory announcements that could have big impact. Basically, the Office of Personnel Management is asking for personally identifiable medical information from health insurers, and its reasoning is to analyze costs and improve the health system, but they could get very detailed medical information from federal employees, including things like, did they get an abortion? Are they undergoing gender-affirming care? And, obviously, there is a strong concern that that could be used against them.
Rovner: Yeah тІ this was quite a scoop. Really, really interesting story. Lauren.
Weber: Mine was a pretty alarming story by Holly Yan at CNN: “.” And basically there’s this type of drug test that the scientists have found is not that effective, and it’s led to things like bird poop being scraped off a man’s car appearing on a drug test as cocaine, a great-grandmother’s medication testing positive for cocaine, and a toddler’s ashes registering as meth or ecstasy, and horrible legal and other consequences of this kind of misdiagnosis in the field. And the reason these drug tests are often done is because they’re cheaper. There’s a more expensive, more accurate version, but these are cheaper. They’re done in the field. But the potential side effects and horrible, wrongly accused effects are quite large, and so Colorado has passed this law to try and move away from this. And it’s curious to see if other states will follow suit.
Rovner: Yeah, this was something I knew nothing about until I read this story. My extra credit this week is from The Atlantic by Katherine [J.] Wu, and it’s called “.” And it’s about how some of the very top career officials from the NIH [National Institutes of Health], the CDC, and other agencies have, after having been put on leave more than a year ago, finally been reassigned to far-flung outposts of the Indian Health Service in the western United States. They got news of their proposed reassignments with little description of their new roles and only a couple of weeks to decide whether to move across the country or face termination. Now, if these officials’ skills matched those needed by the Indian Health Service, this all might make some sense. But what the IHS most needs are active clinicians: doctors and nurses and social workers and lab technicians. And those who are now being reassigned are largely managers, including т and here I’m reading from the story, quote т “the directors of several NIH institutes, leaders of several CDC centers, a top-ranking official from the FDA tobacco-products center, a bioethicist, a human-resources manager, a communications director, and a technology-information officer.” The Native populations who are ostensibly being helped here aren’t very happy about this, either. Former Biden administration Interior Secretary Deb Haaland, a Native American who’s now running for governor in New Mexico, called the reassignment proposals, quote, “shameful” and “disrespectful.” Also, and this is my addition, not a very efficient use of human capital.
OK, that’s this week’s show. Thanks this week to our fill-in editor, Mary-Ellen Deily, and our producer-engineer, Francis Ying. A reminder: What the Health? is now available on WAMU platforms, the NPR app, and wherever you get your podcasts т as well as, of course, kffhealthnews.org. Also, as always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can find me on X , or on Bluesky . Where do you guys hang these days? Maya.
Goldman: I am on LinkedIn under my first and last name, , and on X at .
Rovner: Alice.
Ollstein: I’m on Bluesky and on X .
Rovner: Lauren.
Weber: Still @LaurenWeberHP on both and .
ИщДЧБЙВдБ№Аљ:Ь§We will be back in your feed next week.Т Until then, be healthy.
Credits
Click here to find all our podcasts.
And subscribe to “What the Health? From бюЙѓхњДЋУНвюl Health News” on , , , , , or wherever you listen to podcasts.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/podcast/what-the-health-441-mifepristone-trump-budget-request-hhs-april-9-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2181013&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“The first time, it’ll ring interminably. Next time, it’ll go to a voicemail that just hangs up on you,” said the 48-year-old, who lives in Delaware. “Sometimes you’ll get a person who says they’re not the right one. They transfer you, and it hangs up. Sometimes, it picks up and there’s just nobody on the line.”
She spent months trying to figure out whether her Medicaid coverage had been renewed. As of late March, she hadn’t been reapproved for the year for the state-federal program, which provides health insurance for people with low incomes and disabilities.
Crouch, who suffered a debilitating brain aneurysm a decade ago, also has Medicare, which covers people who are 65 or older or have disabilities. Medicaid had been paying her monthly Medicare deductibles of $200, but she’d been on the hook for them for the past three months, straining her family’s fixed income, she said.
Crouch’s challenges with Delaware’s Medicaid call center aren’t unique. State Medicaid agencies can struggle to keep enough staff to help people sign up for benefits and field calls from enrollees with questions. A shortage of such workers can keep people from fully using their benefits, health policy researchers said.
Now, congressional Republicans’ One Big Beautiful Bill Act, which President Donald Trump signed into law last summer, will soon demand more from staff at state agencies in places where lawmakers expanded Medicaid to more low-income adults — nearly all states and the District of Columbia.
Under the law, which is expected to reduce Medicaid spending by almost $1 trillion over the next eight years, these staffers will have to not only determine whether millions of enrollees meet the program’s new work requirements but also verify more frequently that they qualify for the program — every six months instead of yearly.
бюЙѓхњДЋУНвюl Health News reached out to agencies that will need to stand up the work rules, and many said they’ll need additional staff.
The mandates will put extra strain on an already-stressed workforce, potentially making it harder for enrollees like Crouch to get basic customer service. And many could lose access to benefits they’re legally entitled to, said consumer advocates and health policy researchers, some of them with direct experience working at state agencies.
States are already “struggling significantly,” said Jennifer Wagner, the director of Medicaid eligibility and enrollment at the Center on Budget and Policy Priorities and a former associate director of the Illinois Department of Human Services. “There will be significant additional challenges caused by these changes.”
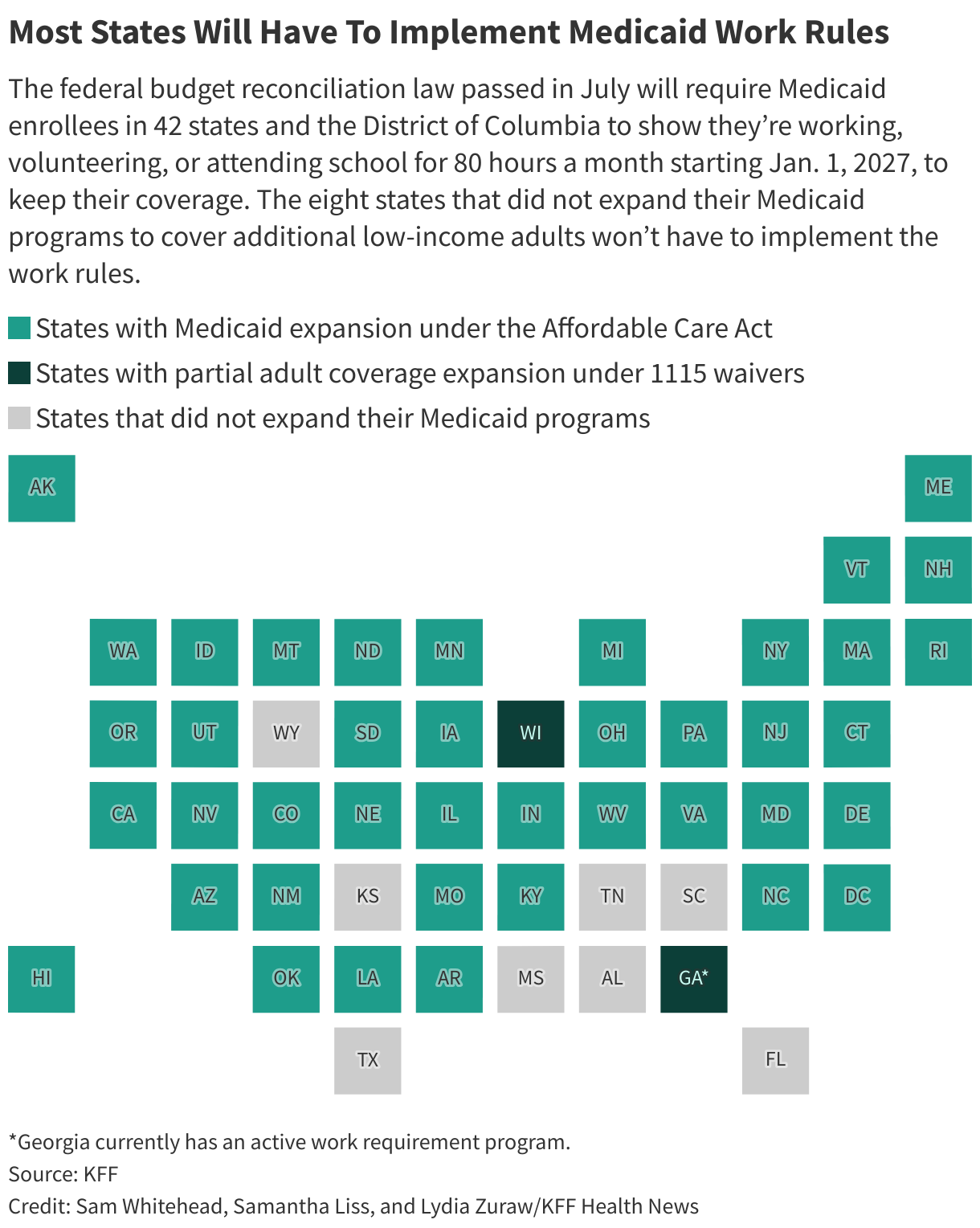
Long Wait Times for Help
Republicans argue the Medicaid changes, which will take effect Jan. 1, 2027, in most states, will encourage enrollees to find jobs. Research on other Medicaid work requirement programs has found little evidence they increase employment.
The Congressional Budget Office would cause more people to lose health coverage by 2034 than any other part of the GOP budget law. It said last year more than 5 million people could be affected.
Many states don’t have the staff to process Medicaid applications or renewals quickly, said consumer advocates and researchers.
The Centers for Medicare & Medicaid Services tracks whether states can handle the most common type of benefit application within a 45-day window.
In December, about 30% of all Medicaid and Children’s Health Insurance Program, or CHIP, applications in Washington, D.C., and Georgia to process. More than a quarter took that long in Wyoming. In Maine, 1 in 5 applications missed that deadline.
CMS began publicly sharing state Medicaid call center data in 2023, revealing a taxed system, researchers and consumer advocates said.
In Hawaii, people waited on the phone for more than three hours in December. They waited for nearly an hour in Oklahoma, and more than an hour in Nevada.
In 2023, state Medicaid agencies began making sure enrollees who were protected from being dropped from the program during the covid pandemic still qualified for coverage. That Medicaid unwinding process didn’t go well in many states, and lost their benefits.
Health policy researchers and consumer advocates say rolling out the new Medicaid rules will be a bigger challenge. The Medicaid work rules will require extensive IT system changes and training for workers verifying eligibility on a tight timeline.
“It is a much larger scale of administrative complexity,” said Sophia Tripoli, senior director of policy at Families USA, a health care consumer advocacy organization.
After months of trying to get someone on the phone, Crouch said, she finally got answers to questions about her Medicaid benefits after writing to the office of U.S. Rep. Sarah McBride (D-Del.). McBride’s office contacted the state’s Medicaid agency, which eventually called with an update, Crouch said.
Crouch didn’t qualify for Medicaid after all. She said that had never come up in two years of interactions with the state.
“It makes absolutely no sense” that the state never realized she shouldn’t have been on the program, Crouch said.
Delaware’s Medicaid agency didn’t respond to requests for comment on Crouch’s situation.
States Short-Staffed for Medicaid
Some states told бюЙѓхњДЋУНвюl Health News in late March that they’ll need more staff to roll out the work rules effectively.
Idaho said it has 40 eligibility worker vacancies. New York estimated it will need 80 new employees to handle the additional administrative work, at a cost of $6.2 million. Pennsylvania said it has nearly 400 open positions in county human services offices in the state. Indiana’s Medicaid agency has 94 open positions. Maine wants to hire 90 additional staffers, and Massachusetts wants to hire 70 more.
As of early March, Montana had filled 39 of 59 positions state officials projected it would need. The state still plans to roll out the rules early, starting July 1, despite its long struggle with system backlogs that applicants said have delayed benefits.
Missouri’s social services agency has been cutting staff and has 1,000 fewer front-line workers than it did roughly a decade ago — with more than double the number of enrollees in Medicaid and the Supplemental Nutrition Assistance Program, or SNAP, according to comments Jessica Bax, the agency director, made in November.
“The department thought that there would be a gain in efficiency due to eligibility system upgrades,” Bax said. “Many of those did not come to fruition.”
States could have a hard time finding people interested in taking those jobs, which require months-long training, can be emotionally challenging, and generally offer low pay, said Tricia Brooks, a researcher at the Georgetown University Center for Children and Families.
“They get yelled at a lot,” said Brooks, who formerly ran New Hampshire’s Medicaid and CHIP customer service program. “People are frustrated. They’re crying. They’re concerned. They’re losing access to health care, and so sometimes it’s not an easy job to take if it’s hard to help someone.”
States are paying government contractors millions of dollars to help them comply with the new federal law.
Maximus, a government services contractor, provides eligibility support, such as running call centers, in 17 states that expanded Medicaid and interacts with nearly 3 in 5 people enrolled in the program nationally, according to the company.
During a February earnings call, company leadership said Maximus can charge based on the number of transactions it completes for enrollees, independent of how many people are enrolled in a state’s Medicaid program.
Maximus has “no one-size-fits-all approach” to the services it offers or the way it charges for those services, spokesperson Marci Goldstein told бюЙѓхњДЋУНвюl Health News.
The company, which reported bringing in $1.76 billion in 2025 from the part of its business that includes Medicaid work, expects that revenue to continue to grow, even as people fall off the Medicaid rolls, “because of the additional transactions that will need to take place,” David Mutryn, Maximus’ chief financial officer and treasurer, said during the earnings call.
Losing Medicaid health coverage isn’t just an inconvenience, since many people enrolled in the program probably don’t make enough money to pay for health care on their own and may not qualify for financial help for Affordable Care Act coverage, said Elizabeth Edwards, a senior attorney with the National Health Law Program.
People could be unable to afford medications or get essential care, which could lead to “devastating” health impacts, she said.
“The human stakes of this are people’s lives,” she said.
бюЙѓхњДЋУНвюl Health News correspondents Katheryn Houghton and Samantha Liss contributed to this report.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-cuts-work-requirements-state-staff-shortages/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178951&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>OAKLAND, Calif. т Rosa María Carranza leaned forward to hold a 3-year-old’s back as the girl climbed a rock in the forested hills of northeast Oakland.
Dressed in hiking gear and beaded necklaces, Carranza, 67, maneuvered between trees and children on a sunny morning in December. “Hold on to that branch,” she said in Spanish. “You can do it, my love!”
Carranza, a child development professional who grew up swinging through trees and swimming in rivers in El Salvador, said she feels at home in the forest at the outdoor preschool she co-founded. She has worked with children and teens as a caregiver and educator for more than three decades, long enough to know when to lean in and when to step back to let her students find their own footing.
When she transitioned to working part-time last year, Carranza counted on getting Medicare and Social Security checks т benefits given to American workers and lawfully present immigrants when they retire, work history and age or disability requirements. She’s contributed tens of thousands of dollars into Medicare and Social Security over 24 years, according to her Social Security Administration earnings record, reviewed by El Tímpano and бюЙѓхњДЋУНвюl Health News. But Carranza and an estimated immigrants will soon be cut out of Medicare.
The GOP’s One Big Beautiful Bill Act, signed last July by President Donald Trump, barred certain categories of lawfully present immigrants т including temporary protected status holders, refugees, asylum-seekers, survivors of domestic violence, trafficking victims, and people with work visas т from Medicare.
Those already in the program, like Carranza, will be disenrolled by Jan. 4 т a move by Republican lawmakers to rein in Medicare spending, as they and Trump have argued that taxpayer dollars should not be used to pay for the health care of immigrants in the U.S. without authorization.
“The Democrats want Illegal Aliens, many of them VIOLENT CRIMINALS, to receive FREE Healthcare,” Trump two months after he signed the bill into law. “We cannot let this happen!”
However, the categories of immigrants now losing coverage do have legal status. Neither the White House nor the Department of Health and Human Services responded to a question about whether it was fair to disenroll legal residents from Medicare.

Immigrants without legal status were already ineligible for Medicare or most other federally funded public benefits.
Carranza is worried that she could also lose legal permission to live in the United States if the Trump administration ends temporary protected status for Salvadorans, as it sought to do during .
If that happened, Carranza would lose legal residency, risking time in an immigration detention center or deportation.
“This is like a horror movie, a complete nightmare,” Carranza said. “This is not how I imagined getting old.”
тUnder Constant Attack’
Carranza left El Salvador in 1991 during a brutal civil war, leaving behind three young children, to earn money to send home to her family. She overstayed her visa until 2001, when she qualified for temporary protected status, after two earthquakes struck El Salvador, and displacing 1.3 million.
Temporary protected status, or TPS, was passed by Congress and signed into law by Republican President George H.W. Bush in 1990.
It allows people such as Carranza, from select nations undergoing armed conflict, civil war, and climate disasters, to live and work in the United States if being in their home country poses a risk.
Carranza missed her youngest daughter’s graduation from kindergarten and first medal-winning performance in track. She worked overnight shifts babysitting newborns and later substitute-taught in public schools in the San Francisco Bay Area to pay for her children’s schooling in El Salvador, and for her own classes at City College of San Francisco, where she earned a degree in child development.
And she cared for dozens of 3-, 4-, and 5-year-olds who gazed in awe as they uncovered little treasures buried in the redwood forest of the Oakland park where she co-founded Escuelita del Bosque, a Spanish immersion preschool that teaches children outdoors.
The trade-off was supposed to be a peaceful retirement. But Congress narrowed Medicare eligibility to citizens, lawful permanent residents, Cuban and Haitian nationals, and people covered under the Compacts of Free Association, agreements between the United States and Pacific island nations.
The move followed Trump’s efforts to bar some lawfully present immigrants from Medicaid, marketplace insurance subsidies, and social support services, such as food assistance, housing subsidies, and medical visits in federally funded health centers. Altogether, 1.4 million lawfully present immigrants were projected to lose health insurance, according to KFF, a health information nonprofit that includes бюЙѓхњДЋУНвюl Health News.
A spokesperson for House Speaker Mike Johnson, Taylor Haulsee, did not respond to requests for comment.

Michael Cannon, director of health policy studies at the Cato Institute, a libertarian think tank, said Republicans wanted to enact tax cuts and eliminate health insurance for immigrants because it wouldn’t upset their base.
“They don’t want to turn the United States into a welfare magnet,” he said. “And they resent the government for making them pay for a welfare state.”
While data on lawfully present immigrants is not available, immigrants without legal status and $25.7 billion into Social Security in 2022, according to the Institute on Taxation and Economic Policy. The Congressional Budget Office estimated that the Medicare restrictions alone would reduce federal spending by 2034.
Health experts say eliminating coverage for immigrants with legal status .
“This is actually the first time that Congress has taken away Medicare from any group,” said Drishti Pillai, director of immigrant health policy at KFF. “This change is impacting immigrants who have lawful presence in the U.S., and many of whom have already worked and paid into the system for decades.”
As older adults like Carranza lose their Medicare coverage, clinicians anticipate that they will delay their care, leading to an increase in severely ill patients, especially in hospital emergency rooms.
Seniors can become sick suddenly and quickly, and they are more vulnerable to cardiovascular diseases such as heart disease and high blood pressure, especially if they put off routine care, said Theresa Cheng, an emergency physician at Zuckerberg San Francisco General Hospital and assistant clinical professor of emergency medicine at the University of California-San Francisco.
“It’s quite easy for them to fall off the cliff,” Cheng said.
Carranza hikes and considers herself healthy, but she acknowledges that she is aging and starting to struggle to keep up with the kids in the forest.
Late last year she was diagnosed with high blood pressure, and in January she woke up with a tight chest and went to urgent care because it had spiked to dangerous levels. A few weeks later, she tripped on a curb while walking and fell to the ground. She woke up the next day with a swollen foot. A doctor at the local hospital told her she had arthritis.
These were scary moments, she said, but she was grateful to have to pay only $10 for the urgent care visit and $5 to see her primary care doctor. However, that will change when she loses Medicare by early next year.
The stress of knowing she will lose health insurance coverage, and potentially her legal status, all while masked federal agents are detaining immigrants like her across the country, has taken a toll on her mental health, she said. She is searching for a therapist and acupuncture services to treat her insomnia and anxiety т and the feeling that she is “under constant attack.”

Nowhere To Turn
In California, home to the largest number of , Carranza could have enrolled in state-sponsored insurance, but this year the state for adults 19 and older who are a TPS holder, in the U.S. without authorization, or an asylum-seeker. Other states with Democratic governors such as have also scaled back their health programs for immigrants amid budget pressures.
In January, California Gov. Gavin Newsom proposed a state budget that would not backfill federal health care cuts to about 200,000 lawfully present immigrants, noting the $1.1 billion annual price tag and state budget shortfalls.
“Given these fiscal pressures, the administration cannot backfill for this change in federal policy,” California Department of Finance spokesperson H.D. Palmer said.
But some Democratic lawmakers and consumer advocates say the state should step in. State Assembly member Mia Bonta, who chairs the Assembly’s health committee, said she is working on a legislative budget solution to bring immigrants who will lose health coverage, including older adults, into Medi-Cal, the state’s version of Medicaid.
The East Bay Democrat is especially concerned for people like Carranza, “who have lived here for decades and contributed into this economy, who have given into our cultural fabric and into our communities and who built families and lives and who are now wanting to be able to retire with dignity and live with dignity and have the health care that they need.”

A Sign of the Future
Last April, Carranza got a glimpse of what losing her health coverage and retirement benefits could look like, after the Social Security Administration sent her a letter informing her that she no longer qualified for retirement benefits because she was not lawfully present in the U.S. т even though she was. Then Medicare stopped payments to her health plan, which disenrolled her as a result.
As a TPS holder with a work permit, she knew a mistake had been made. Yet, without her check, Carranza didn’t have money to pay her rent for a month. She worked off her rent by babysitting her landlords’ children. Last May, the office of U.S. Rep. Lateefah Simon, an Oakland Democrat, helped Carranza recover her retirement benefits, but it took months for her to get her health insurance back.
The experience left her reeling.
“It’s like getting slapped on the face after more than 30 years working for the system here,” Carranza said. “And in return, this is what we have now.”
She lies awake at night imagining the future: here, where she’s spent half her life, without health insurance and possibly Social Security benefits; or in El Salvador, where two of her three children remain. Her daughter, a green-card holder who lives in Texas, hopes to become a citizen so she can petition for permanent residency for Carranza, but the process can take years. Then there’s the possibility she fears most: indefinite detention or deportation.
On a recent morning in her basement studio in Oakland, Carranza pulled a box from the back of her closet. In it was a thick stack of identification cards that included old driver’s licenses, her Social Security card, and dozens of work IDs issued by the federal government.
“My life is in that box,” she said.
This article was produced in collaboration with , a civic media organization serving and covering the Bay Area’s Latino and Mayan immigrant communities.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/immigrant-seniors-medicare-california-big-beautiful-bill-eligibility-taxes/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2172022&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Recent polling finds that health costs are a top worry for much of the American public, while Republicans in Congress are considering still more cuts to federal health spending on programs such as Medicaid and the Affordable Care Act.
Meanwhile, the Supreme Court ruled that Colorado cannot ban mental health professionals from using “conversion therapy” to treat LGBTQ+ minors, a decision that’s likely to affect other states with similar laws.
This week’s panelists are Julie Rovner of бюЙѓхњДЋУНвюl Health News, Jessie Hellmann of CQ Roll Call, Alice Miranda Ollstein of Politico, and Sandhya Raman of Bloomberg Law.
Panelists



Among the takeaways from this week’s episode:
- Republicans reportedly are weighing still more cuts to federal health spending. With the war in Iran draining military coffers, GOP leaders in Congress are eying a drop in health funding т a decision that could exacerbate problems following the passage of legislation expected to lead to major reductions in Medicaid spending, as well as the expiration of enhanced ACA premium subsidies that were not renewed by lawmakers last year. And President Donald Trump’s budget could include another sizable reduction in funding to the National Institutes of Health.
- The Supreme Court this week struck down a Colorado law prohibiting licensed professionals from practicing a form of therapy that tries to change the sexual orientation or gender identity of LGBTQ+ minors. States have long had the power to regulate medical care, with the goal of restricting treatments that can be harmful. Also, the Idaho Legislature passed a bill requiring teachers and doctors to out transgender minors to their parents.
- Meanwhile, the Department of Health and Human Services is studying whether to make private Medicare Advantage plans the default option for seniors enrolling in Medicare, a change that would seem to conflict with the Trump administration’s scrutiny of overpayments to the private insurance plans. And a tech nonprofit’s lawsuit seeks to reveal more about the administration’s pilot program testing the use of artificial intelligence in prior authorization in Medicare.
Also this week, Rovner interviews бюЙѓхњДЋУНвюl Health News’ Elisabeth Rosenthal, who wrote the last two бюЙѓхњДЋУНвюl Health News “Bill of the Month” stories. If you have a medical bill that’s outrageous, infuriating, or just inscrutable, you can submit it to us here.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:Т
Julie Rovner: New York Magazine’s “,” by Helaine Olen.
Jessie Hellmann: The Texas Tribune’s “,” by Colleen DeGuzman, Stephen Simpson, Terri Langford, and Dan Keemahill.
Sandhya Raman: Science’s “,” by Jocelyn Kaiser.
Alice Miranda Ollstein: The New York Times’ “,” by Ed Augustin and Jack Nicas.
Also mentioned in this week’s podcast:
- бюЙѓхњДЋУНвюl Health News’ “States Pay Deloitte, Others Millions To Comply With Trump Law To Cut Medicaid Rolls,” by Samantha Liss and Rachana Pradhan.
- бюЙѓхњДЋУНвюl Health News’ “Trump’s Hunt for Undocumented Medicaid Enrollees Yields Few Violators,” by Phil Galewitz.
- The Colorado Sun’s “,” by John Ingold.
- Politico’s “,” by Alice Miranda Ollstein, Erin Doherty, Marcia Brown, and Carmen Paun.
- The New York Times Magazine’s “,” by Coralie Kraft.
- NOTUS’ “,” by Margaret Manto.
- The Dallas Morning News’ “,” by Emily Brindley.
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, from бюЙѓхњДЋУНвюl Health News and WAMU Public Radio in Washington, D.C. Welcome to What the Health? I’m Julie Rovner, chief Washington correspondent for бюЙѓхњДЋУНвюl Health News, and I’m joined by some of the best and smartest health reporters covering Washington. We’re taping this week on Thursday, April 2, at 10 a.m. As always, news happens fast, and things might have changed by the time you hear this. So here we go.
Today, we are joined via video conference by Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Hello.
Rovner: Jessie Hellmann of CQ Roll Call.
Jessie Hellmann: Thanks for having me.
Rovner: And Sandhya Raman, now at Bloomberg Law.
Sandhya Raman: Hello, everyone.
Rovner: Later in this episode, we’ll have my interview with бюЙѓхњДЋУНвюl Health News’ Elisabeth Rosenthal, who reported and wrote the last two бюЙѓхњДЋУНвюl Health News “Bills of the Month.” One is about a patient who got caught in the crossfire over prices between insurers and drug companies. The other is about a woman who, and this is not an April Fools’ joke, got her insurance canceled for failing to pay a bill for 1 cent. But first, this week’s news.
So Congress is on spring break, but when they come back, health policy will be waiting. A new Gallup poll out this week found 61% of those surveyed said they worry about the availability and affordability of health care, quote, “a great deal.” That was 10 percentage points more than the economy, inflation, and the federal budget deficit, and it topped a list of 15 domestic concerns. And while we are still waiting for final enrollment numbers for Affordable Care Act plans, we do know that the share of people paying more than $500 a month for their coverage doubled from last year to 2026. Yet Axios this week is reporting that Republicans are considering still more cuts to the Affordable Care Act to potentially pay for a $200 billion war supplemental. What exactly are they thinking? And it’s looking more like Republicans are going to try for another budget reconciliation bill this spring. Isn’t that, right, Jessie?
Hellmann: House Budget chair Jodey Arrington has kind of been pushing this idea really hard of going after what he says is fraud in mandatory programs like Medicare and Medicaid. He’s also talked about funding cost-sharing reductions, which is an idea that slipped out of the last reconciliation bill, and it’s a wonky kind of idea тІ
Rovner: But I think the best way to explain it is that it will raise premiums for many people. That’s how I’ve just been doing it.
Hellmann: Yeah, exactly.
Rovner: Let’s not get into the details.
Hellmann: It would reduce spending for the federal government but wouldn’t really help people who buy insurance on the marketplace. He hasn’t been very specific. He’s also talked about, like, site-neutral policies in Medicare, but it’s hard to see how all of this could make a serious dent in a $200 billion Iran supplemental. There’s also a new development. I think President [Donald] Trump threw a wrench in things yesterday when he said he wanted the reconciliation bill to focus on border spending and immigration spending to cover a three-year period, and now Senate Majority Leader John Thune is saying that there’s probably not room for much else in the bill. So, unclear what the path forward is for all of that.
Rovner: Yeah, and of course, that was part of the deal to free up the Department of Homeland Security’s budget in the appropriation. It’s all one sort of big, tied-up mess at this point. Alice, I see you’re nodding.
Ollstein: Yeah. I mean, what often happens with these reconciliation bills is it starts out with a tight focus and everyone’s unified, and then, because it can often be the only legislative train leaving the station, everybody gets desperate to get their pet issue on board, and then the more and more things get piled onto it, then they start losing votes, and people start disagreeing more. And so I think even though this is still in the ideas phase, you’re already seeing some signs of that happening. And when it comes to health care, it can be particularly fraught. And of course, you have lawmakers, especially in the House, with wildly different needs. Some of them need to fend off a primary from the right, and so they want to be as conservative as possible. Some are fighting to hang on in swing districts, and so they want to be more moderate. And these things are in conflict. And so these proposals to cut health spending, even more than the massive amount that was cut last year, are already, you know, raising some red flags among some moderate Republican members. And it’s very possible the whole thing falls apart.
Rovner: Well, along those lines, we’re supposed to get the president’s budget on Friday, which is only two months late. It was due in February. And while I haven’t seen much on it, Jessie, your colleagues at Roll Call are reporting that the budget will seek a 20% cut to the National Institutes of Health. That’s only half the cut that the administration proposed last year. But given that Congress actually boosted the agency’s budget slightly this year, that feels kind of unlikely.
Hellmann: Yeah, I don’t think that the appropriators are likely to go along with this. They have really strong advocates, and Sen. Susan Collins, who’s chair of the Senate Appropriations Committee. And, like you said, they rejected cuts last year. Kind of surprised. Twenty percent is not as deep as the Trump administration went last year. I was actually kind of surprised it wasn’t a bigger proposed cut. But either way, I don’t think Congress is going to go along with that.
Rovner: Meanwhile, I saw a late headline that FDA is looking to hire back people after DOGE [Department of Government Efficiency] cut thousands of people last year. Sandhya, HHS [Department of Health and Human Services] is just in this sort of personnel churn at this point, isn’t it?
Raman: Yeah, I think that HHS is kind of getting bit in the foot from, you know, we’ve had so many of these layoffs, and we’ve also had a lot of people just flee the various agencies over the past year because of some of this instability and all of these changes. And as we’re getting closer and closer to, you know, deadlines of things that they need to get done, they’re realizing that they do need more personnel to get some of those things done, as we’ve been passing deadlines. So I don’t think it’s something that’s unique to just FDA. But I think the way to solve this т it’s not an overnight thing for the federal government to staff up. It’s a longer process, but it’s really showing in a lot of areas right now.
Rovner: Yeah, I would say this is not like TSA [Transportation Security Administration], where you can, you know, hire new people and train them up in a couple of months. These are тІ many of them scientists who’ve got years and years of training and experience at doing some of these jobs that, you know, the federal government is ordered to do by legislation.
Raman: Yeah, those statutes are things that, you know, if they don’t meet those deadlines, those are things that are going to be challenged, and just further tie things up in litigation. And we already see so many of those right now that are making things more complicated.
Rovner: Well, in news that is not from Congress or the administration, the Supreme Court this week said Colorado could not ban licensed mental health professionals from using so-called conversion therapy aimed at LGBTQ individuals, at least not on minors. What’s the practical impact here? It goes well beyond Colorado, I would think.
Ollstein: Interesting, because a lot of people think of this as regulating health care, restricting providers from providing health care that is not helpful and maybe actively harmful to the health of the patients.
Rovner: And that’s тІ I would say that’s been a state тІ
Ollstein: Power.
Rovner: тІ power. For generations.
Ollstein: Absolutely. Right, I mean, you don’t want people selling sketchy snake oil pills on the street, etc. So many people view this as akin to that. But it has morphed in the hands of conservative courts into a free speech issue, and that, you know, these laws are restricting the speech of mental health workers who are against people transitioning. And so, yes, it definitely has national implications. And of course, we are in a national wave right now of both state and federal entities, you know, moving in the direction of rolling back trans rights in the health care space and beyond.
Rovner: Yeah. In related news, regarding Colorado and minors and gender, that Children’s Hospital Colorado has not yet resumed providing gender-affirming care for transgender youth. That’s despite a federal judge in Oregon having struck down an HHS declaration that would have punished hospitals for providing such services. Apparently, the hospital in Colorado is concerned that the judge’s ruling doesn’t provide it with enough legal cover for them to resume that care. I’m wondering, is this the administration’s strategy here to get organizations to do what they want, even if they might lack the legal authority to do it? Just by making them worry that they might come after them?
Raman: I think the chilling effect is definitely a big part of this broader issue. I mean, we’ve seen it in other issues in the past, but just that if there is this worry that it’s a) going to stop on the provider side, new folks taking part in providing care, and also just it’s going to make patients, even if there are opportunities, even less likely to want to go because of the fears there. I mean, it goes broader than that. We’ve had FTC [Federal Trade Commission] complaints, where they have gone and investigated different places that provide gender-affirming care or endorse it. So I think it’s broader than this, and really part of that chilling effect.
Rovner: And Alice, as you were saying, I mean, the subject of transgender rights, or lack thereof, remains a political hot topic. The Idaho Legislature this week passed a bill that now goes to the governor that would require teachers and doctors to out transgender minors to their parents. Parents could sue teachers, doctors, and child care providers who, quote, “facilitate the social transformation of the minor student.” That includes using pronouns or titles that don’t align with their sex at birth. I don’t know about teachers, but that definitely seems to violate patient privacy when it comes to doctors, right?
Ollstein: There’s definitely patient privacy issues there. I also think, you know, it’s interesting that this kind of nonmedical transitioning is now coming under attack. Because, you know, you would think that there would be some support for letting a kid, you know, go by a different name for a few weeks, test it out, see how it feels. Maybe it’s a phase, then they discover that they don’t want to actually pursue taking medications and going through a medical transition. But this is sort of shutting down that avenue as well. You can’t even change your appearance, change how you present in the world, at a time when kids are really trying to figure out who they are. So I think the broad acceptance of hostility to medical transitioning for youth is now spilling over into this kind of social transitioning, and I wonder if we’re going to see more of that in the future.
Rovner: Yeah, I feel like we started with minors shouldn’t have surgery. They shouldn’t do anything that’s not easily reversible. And now we’ve gotten down to, in the Idaho law, there’s actually mention of nicknames. You can’t тІ a kid can’t change his or her nickname. It feels like we’ve sort of reduced this way, way, way down.
Ollstein: And I think we’ve seen these laws, laws related to bathrooms. We’ve seen these have negative impacts on people who are not trans at all, people who just are a tomboy or not looking like people’s stereotypes of what different genders may look like. And so there’s a lot of policing of people who are not trans in any way. You know, there’s media reports of people being confronted by law enforcement for going into a bathroom that does align with their biological sex. And so it’s important to keep in mind that these laws have an effect that’s much broader than just the very small percentage of people who do consider themselves trans.
Rovner: Yeah, it’s kind of the opposite of not being woke. All right, we’re going to take a quick break. We will be right back.
So while we’ve had lots of news out of the Department of Health and Human Services the past few weeks, it’s been mostly public health-related. But there’s a lot going on in the Medicare and Medicaid programs too. Item A: Stat News is reporting that HHS is studying whether to make the private Medicare Advantage program the default for seniors when they qualify for Medicare. Right now, you get the traditional fee-for-service plan that allows you to go to any doctor or hospital that accepts Medicare, which is most of them. You have to affirmatively opt into Medicare Advantage, which often provides extra benefits but also much narrower networks. What would it mean to make Medicare Advantage the default, that people would go into private plans instead of the government plan, unless they affirmatively opted for the traditional fee-for-service?
Hellmann: Someone’s experience with тІ can vary greatly between being on traditional Medicare and Medicare Advantage. If you’re in Medicare Advantage, you could be exposed to narrow networks. You can only see certain doctors that are covered by your plan. You can be exposed to higher cost sharing. A lot of people are kind of fine with their plans until they have a medical issue and need to go to the hospital or they need skilled nursing care. So making this the default could definitely be a challenge for some people, especially people that have complex health needs. Some people on the early side of their Medicare eligibility are fine with Medicare Advantage, and then they get older and they’re not fine with it anymore. So it’s interesting that the administration would kind of float this idea because they’ve been critical of Medicare Advantage.
Rovner: Thank you. That’s exactly what I was thinking.
Hellmann: Yeah, they’ve talked about the federal government pays these plans too much, and it’s not for better quality in a lot of cases, and they’ve talked about reforms in that area. So I was a little surprised to see that.
Rovner: Yeah, Republicans have been super ambivalent. I mean, Medicare Advantage was their creation. They overpaid them at the beginning when they, you know, sort of redid the program in 2003. And they purposely overpaid them to get people into Medicare Advantage. And then the Democrats pointed out that this is wasting money because we’re overpaying them. And now the Republicans seem to have joined a lot of their т at least some Republicans т seem to have joined a lot of the Democrats in saying, Yes, we’re overpaying them. We’re paying them too much. And you know, they talk about the big, powerful insurance companies, and yet they’re now floating this idea to make Medicare Advantage the default. So pick a side, guys.
All right, well, in other Medicare news, the Electronic Frontier Foundation is suing Medicare officials to learn more about the pilot program that’s using artificial intelligence to oversee prior authorization requests in the traditional Medicare fee-for-service program. The idea here is to cut down on, quote, “low-value services,” things that doctors might be prescribing that aren’t either particularly necessary or shown to actually work. But the fear, of course, is that needed care for patients will be delayed or denied, which is what we’ve seen with prior authorization in Medicare Advantage. This is the perennial push-pull of our health care system, right? If you do everything that doctors say, it’s going to be too expensive, and if you second-guess them, it’s going to be, you know, it might turn out to be too constraining.
Hellmann: Well, I was just going to say this is another issue that was kind of a little surprising to me, because there’s been so much criticism of the use of prior authorization and Medicare Advantage. And CMS [Centers for Medicare & Medicaid Services] looked at that and said, Oh, what if we did it in traditional Medicare? Like it was never going to go over well politically, and I think there are even some Republican members of Congress who are not in support of this, but they haven’t really made a huge stink about it. Yeah, this wasn’t something I really expected to see.
Rovner: Yeah, we’ll see how this one plays out too. Well, meanwhile, regarding Medicaid, two really good stories this week from my бюЙѓхњДЋУНвюl Health News colleagues Phil Galewitz, Rachana Pradhan, and Samantha Liss. Phil’s story found that efforts in multiple states to find enrollees who were not eligible for the program due to their immigration status turned up very few violators. While Samantha and Rachana detailed the hundreds of millions of dollars states and the federal government are spending to set up computer programs to track Medicaid’s new work requirement, despite the fact that we already know that most people on Medicaid either already work or they are exempt from the requirements under the new law. Is it just me, or are we spending lots of time and effort on both of these policies that are going to have not a very big return?
Ollstein: Well, that’s what we’ve seen in the few states that have gone ahead and attempted this before, that it costs a lot, and you insure fewer people. And that’s not because those people got great jobs with great health care. You insure fewer people, and the level of employment does not meaningfully change.
Rovner: I would say you insure fewer people who may well still be eligible. They just get caught in the bureaucratic red tape of all of this.
Ollstein: Exactly. These tech systems that are being set up are challenging to navigate, if people even have a means to do it, if they even have a smartphone or a computer or access to Wi-Fi. There are not that many physical offices they can go to to work it out if they need to. And some of those are very far from where they live. And so you see some of these tech vendors, you know, are set to make off very well out of this system, and people who need the care not so much. And then, of course, you know, it’s not just the patients who will feel the impact. You have these hospitals around the country that are on the brink of closure. And if they have people who used to be insured т they used to be able to bill and get reimbursed for their services, suddenly they’re uninsured т and they’re coming in for emergency care that they can’t pay for, that the hospital has to throw out-of-pocket for, that puts the strain that some of these facilities can barely cope with. And so you’re seeing a lot of state hospital associations sounding the alarm as well.
Raman: I would also say the timing is interesting. You know, we spent so much time and energy last year going through the reconciliation process to tighten these areas, to get in the work requirements, to reduce immigrant eligibility for Medicaid. And then, you know, as they’re gearing up to possibly do this again, to defer their crackdown on health care as part of that, instead of it saving money т that it’s not having as much of an effect and costing so much, in the case of the work requirements, where we’re not expected to see the return of it.
Rovner: Yeah, that may be, although I guess the return is that people will not have insurance anymore, and so the federal government, the states, won’t be spending money for their medical care. They’ll be spending money on other things. All right, of course, there’s more news from HHS than just Medicare and Medicaid this week. We also have a lot of news about the Make America Healthy Again movement, which is a sentence that 2023 me would definitely not recognize. about a new poll that finds the MAHA vote isn’t necessarily locked in with Republicans. Tell us about it.
Ollstein: Yeah, that’s right. So Politico did our own polling on this, because we hadn’t really seen good data out there on who identifies as MAHA and what do they even believe about the different parties and about different issues. And so we found that, OK, yes, most people associate MAHA with the Republican Party т most, but not all. But a lot of voters who identify as MAHA, and a lot of voters who voted for Trump in 2024 don’t think that the Trump administration has done a good job making America healthy again. And they rank the Democratic Party above the Republican Party on a lot of their top priority issues, like standing up to influence from the food industry and the pharmaceutical industry. They rank Democrats as caring more about health. So, you know, we found this very fascinating, and it supports what we’ve been hearing anecdotally, where Democratic candidates, a handful of them, and Democratic electoral groups, are really seeing a lot of opportunity to go after MAHA voters and win them over for this November. And you know, we should remember that even if you don’t see a big swing of people voting for Democrats, even if MAHA voters are disillusioned and stay home, that alone could decide races. You know, midterms are decided by very narrow margins.
Rovner: Well, two other really interesting MAHA takes this week. . It’s about the tension in and among medical groups, about how to deal with HHS Secretary [Robert F.] Kennedy [Jr.] and the MAHA movement. The American Medical Association seems to be trying to play nice, at least on things it agrees with the secretary about, lest it risk things like its giant contract to supply the CPT billing codes to Medicare. On the other hand, the American Academy of Pediatrics and the American College of Physicians have been more confrontational to the point of going to court. The other story, from pushing MAHA. One thing I noticed is that all of the teens in the story seem to suffer from physical problems that are not well understood by the mainstream medical community, and so they turned online to seek advice instead, which is understandable in each individual case. But then they turn around and try to influence others. And you can see how easily misinformation can spread. It makes me not so much wonder т it makes me see how, oh, this is how this stuff sort of gets out there, because you see so much тІ and Alice, this goes back to what you were saying about MAHA is not a movement that’s allied with one particular political party. It’s more of sort of a mindset that doesn’t trust expertise.
Ollstein: I think it spans people who identify as Democrats, identify as Republicans. And, you know, we’re not really interested in politics until the rise of Robert F Kennedy Jr., and so I think it does show a lot of malleability. And there is a fight for this, for this cohort right now, on the airwaves, on the internet, etc.
Rovner: And, as The New York Times pointed out, you know, we’ve thought of this as being sort of a young men cohort. It’s now also a young woman cohort, too. So there’s lots of people out there to go and get, for these people who are pursuing votes.
Well, turning to reproductive health, we have a couple of follow-ups to things we covered earlier. The big one is Title X, the federal family planning program, whose grants were set to end as of April 1. Sandhya, it looks like the federal government is going to fund the program after all?
Raman: Yeah, the family planning grantees in this space have been on edge for so long, you know, waiting to see would they finally just issue the grant applications. And then it was such a short timeline for them to get them done. And then everyone that I talked to in the lead-up was expecting some sort of delay, just because it was such a short timeframe before they were set to run out of money. And so I think that they were all pleasantly surprised that HHS was able to turn things around when they confirmed that the money is going to go out the day before the deadline. It does take a couple of days to go through the process and get that done. But I think the new worry now is also that in the statements that the White House and HHS have made is just that they are still at work on getting Title X rulemaking out so that a lot of these groups would be ineligible if they also provide abortions. Or we also don’t know what will be in the rule т if it will be broader than what was under the last Trump administration, if it encompasses other restrictions. So a little bit of both there.
Rovner: Yeah. And I also was gonna say, I mean, we know that anti-abortion groups are unhappy with the administration, so this would be one place where they could presumably throw them a bone, yes?
Ollstein: So people on both sides have been a little mystified why we haven’t seen a new Title X rule yet. They were expecting that near the beginning of last year, especially if the administration was just planning to reimpose his 2019 version, that would be pretty straightforward and simple. And yet, here we are, more than a year into the administration, and we haven’t really seen this yet. The administration did confirm to me т we put this in our newsletter т that a new rule is coming. And they said it will align with pro-life values. And the White House’s comments to some conservative media outlets were very explicit that this will be the last time Planned Parenthood can get funding. Now I wonder if that statement will come back to bite them in court, because the rule previously was very careful not to name Planned Parenthood or name any specific organization. It just imposed criteria that applied to a lot of Planned Parenthood facilities, and in order to make them ineligible for Title X funding. And so I wonder if that will help Planned Parenthood sue later on. But we’ll put a pin in that and come back to it. But we have confirmed that some sort of new rule is coming, but we don’t know when, and we don’t know what it would entail. There’s a lot of speculation that this could go way beyond an attempt to kick Planned Parenthood out. There’s speculation it could involve restrictions on particular forms of birth control. There’s speculation that it could entail restrictions on gender-affirming care. There’s speculation that it could involve rules around parental consent, stricter parental consent requirements, which are currently something that’s not part of Title X. And so we just don’t know, you know, in order to mollify the anti-abortion groups that are upset, they are saying, Don’t worry, new rule is coming. But again, we don’t know when, and we don’t know what’s going to be in it.
Rovner: Well, we’ll be here when it happens. Another topic we’ve talked about at some length is crisis pregnancy centers, which are anti-abortion organizations that sometimes offer some medical services. who was told after an ultrasound at a crisis pregnancy center that she had a normal pregnancy, and three days later, ended up in emergency surgery because the pregnancy was not normal, but rather ectopic т in other words, implanted in her fallopian tube rather than her uterus, which could have been fatal if not caught. This is not the first such case, but it again raises this question of whether these centers should be treated as medical facilities, which we’ve talked about many states do.
Raman: And I think a lot of the rationale that people have for trying to do some of these mandatory ultrasounds, you know, encouraging people to go to this is because the talking point is that you don’t know if you have an ectopic pregnancy, you don’t have another complication, so you should go here to instead of just taking a medication abortion. So тІ we’re coming full circle here, where this is also not helping the case, if you’re not finding the full information there. So I think that was an interesting point to me тІ
Rovner: Yeah, it’s going on both sides basically. It is fraught, and we will continue to cover it.
All right, that is this week’s news. Now we’ll play my interview with Elisabeth Rosenthal at бюЙѓхњДЋУНвюl Health News, and then we will come back and do our extra credits.
I am pleased to welcome back to the podcast бюЙѓхњДЋУНвюl Health News’ Elisabeth Rosenthal, who reported and wrote the last two “Bills of the Month.” Libby, thanks for coming back.
Elisabeth Rosenthal: Thanks for having me.
Rovner: So let’s start with our drug copay card patient. Before we get into the particulars, what’s a drug copay card?
Rosenthal: Well, copay cards, or copayment programs, are things that the drug companies give patients. You know, when it says you could pay as little as $0, where they pay your copayment, which is usually pretty big т when you see a copay card, it means the price is big, and they’ll bill your insurance for the rest. So for patients, it sounds like a good deal, and it is a good deal when they work.
Rovner: So tell us about this patient, and what drug did he need that cost so much that he required a copay card?
Rosenthal: Well, the funny thing is т his name is Jayant Mishra, and he has a psoriatic arthritis. And the doctor told him, you know, there’s this drug called Otezla that would really help you. And he was, he was a little cautious, because he knew it could be expensive, so he did wait a few months, and his symptoms, his joint pain, in particular, got worse. He was like, OK, I’ll start it. So he started it the first month, and it worked really well.
Rovner: “It” the drug, or “it” the copay card, or both?
Rosenthal: Both seemed to work very well. So the copay card covered his copay of over $5,000 and he was like, Oh, this is great. And then what happened was, the next month, he tried to fill it, and it was like, Wait, the copay card didn’t work! And really what happens is copay cards, they are often limited in time and in the amount of money that’s on them. So depending on how much the copay is, they can run out, basically expire. You used all the money, and you have a drug that you’ve used that is working really well for you, and then suddenly you’re hit with a big bill. So they kind of get people addicted to drugs, which they then can’t afford.
Rovner: And what happened in this case was the insurance company charged more than expected, right?
Rosenthal: Well, Otezla, you know, there’s so many things about this, and many “Bill of the Month” stories that, you know, are eye-rollers. Otezla т there are biosimilars that were approved by the FDA in тІ 2021? тІ which everyone’s talking about, faster approval of biosimilars. Well, this was approved, but the drugmaker filed multiple suits and patent infringement, and so in the U.S., it won’t be on the market, the biosimilar, until 2028, so that’s a problem too.
Rovner: So if you want this drug, it’s going to be expensive.
Rosenthal: It’s going to be expensive. And the other problem is copay cards. Insurers used to say, OK, that will count towards your deductible, right? So you didn’t really feel it, right? Because you got a $5,000 copay card, and you had a $5,000 deductible if you had a high-deductible plan. And everything was good. Now, insurers kind of said, Whoa, we’re not sure we like these things. So yeah, you can use them, but it won’t count towards your deductibles. So they’re not nearly as useful as they might have been in the past. But patients are really stuck, because these are really expensive drugs that most people couldn’t afford without copay cards.
Rovner: So what eventually happened to this patient, and how can other people avoid falling into the copay card trap?
Rosenthal: So basically, because he had used up the amount on the copay card, which was $9,400 for the year, by the second month, he tried for the third month to kind of ration his drugs to take half as much, and his symptoms came back. And then the lucky thing for him was then it was January, right, copay cards are usually done for the year. So he got a new copay card for another $9,400 and he was good for January, and he paid with his health savings account for the first month’s copay, with the copay card the second month, with the copay card and his health savings account. And when this went to press, he wasn’t sure how he was going to pay for the rest of the year. And for him, it’s not a huge problem, because he has a very well-funded health savings account, which few of us do, but he was really up in the air for the rest of the year when we wrote about this.
Rovner: So sort of moral of this story, be careful if you want to take an expensive drug, and the theory that when the drugmaker promises, Oh, you can have this for as little as $0 copay.
Rosenthal: Well, I think it’s you have to understand what a particular card does. You have to understand what’s the limit on how much is on the copay card. You have to understand how many months it’s good for. You have to understand, from your insurer’s point of view, if that will count as your deductible or not. And then, man, you know, you’re kind of on your own, right? Sometimes your copay card will work great for you, and at other times it will work for a shorter amount of time. And you got to figure out what to do. I think the third, bigger lesson is getting biosimilars, which are these very expensive drugs approved, is not really the big problem in our country. The problem is the patent thickets that surround so many of these drugs that prevent them from getting to the patients who need them.
Rovner: In other words, you can make a copy of this drug, but you might not be able to get it onto the market.
Rosenthal: Right. You can make a copy this drug т it [a generic] was approved in 2021 т but that won’t help patients until 2028, which is really terrible. You know, it’s available in other countries, but not here.
Rovner: So moving on, our March patient had insurance through the Affordable Care Act exchange and was benefiting from one of those zero-premium plans until she got caught in a literally Kafkaesque mess over a 1-cent bill that turned into a 5-cent bill. Who is she and what happened here?
Rosenthal: Yeah, her name in this wonderful, terrible story is Lorena Alvarado Hill. And what happened here is she was on one of these $0 insurance plans through the Obamacare exchanges with that great subsidy, the Biden-era subsidy, and she and her mother were on the same plan, and her mother went on to Medicare, turned 65. So Lorena didn’t need the family coverage and told the insurer that. And the insurance, of course, automatically recalculates your subsidy, and her premium went from being zero to 1 cent. Now, no human would make that, you know, would say, Oh, that makes sense. And to Lorena, it didn’t really make sense either. She was like, I’m not sure how to pay 1 cent, like, will it work on my credit card? And some of the bills said, you know, you understand that this could impact the continuation of your insurance, but, you know, she was like, 1 cent, I don’t think so. And then she kept going to doctors, and the insurance still worked, and then at some point, four months later, she got a letter in November saying, Oh, your insurance was canceled in July, and you owe money for all these bills.
Rovner: And what happened with this case?
Rosenthal: Well, you know, like many of our “Bill of the Month” patients, I celebrate them for being real fighters, because her bill, since her premium was 1 cent a month, went from 1 cent to 2 cents to 3 cents to 4 cents to 5 cents, when they sent her the note saying your insurance has been canceled for the last four months. And what turns out, which is really interesting, is this is a known glitch in the way the subsidies were calculated, were administered. There’s a recalculation of subsidies every time there’s a life event, a kid goes off the plan, you change jobs, get married, you get divorced. So the recalculation happens automatically. And the Biden administration, understanding that this glitch could exist, they gave the insurers the option not to cancel insurance if the amount owed was less than $10. And there were apparently 180,000 people caught in this situation where their insurance could have been canceled for under $10 of a recalculated premium. The Trump administration revoked that rule because their feeling was, you owe something, you pay something. So it’s part of their “stamp out fraud and abuse,” and this was, in their view, abuse of a system when people didn’t pay what they owed.
Rovner: One cent.
Rosenthal: One cent, right. So what happened with her is, you know, a good bill-paying citizen sending her daughter to college with loans. She wrote her insurers, she wrote to the state, she wrote to everyone. And as a last resort, of course, someone said, Well, there’s this thing called Bill of the Month you could write to. So when we looked into this, at first HealthFirst, which was her insurer in Florida, said, Oh, she’s not insured through us. And I was like, Yeah, because you canceled her insurance. And then I gave them her insurance number, and they said, Well, yes, according to law, we did the right thing. She didn’t pay, so it was canceled. Somehow, through all of this, word got back to the hospital and the insurer, and they worked together, and her bills were suddenly zero on her portal. So that’s the good news for Lorena Alvarado Hill. It doesn’t really help all those other people whose insurance may have been canceled for premiums that were under $10.
Rovner: So, basically, if you get a bill for 5 cents, you should pay it.
Rosenthal: Yeah, you know, it was funny when this story went up, many people were sympathetic, but other commenters said, Well, she should have just paid $1 because you can pay that. And maybe there was a way to pay 1 cent. And I’m kind of with her, like, if I got a bill for 1 cent, life is busy. This is a woman who is a teacher’s aide and works on weekends at a store to help pay for her daughter’s college. Life is busy. You just can’t sweat over 1-cent bills and spend a lot of time figuring out how to pay them. And I guess the lesson is, what’s the worst that can happen in a very dysfunctional system where so much is automated now? The worst that can happen is always really bad. Your insurance could be canceled.
Rovner: So basically, stay on top of it, I guess, is the message for both of these stories this month. Elisabeth Rosenthal, thank you so much.
Rosenthal: Thanks, Julie, for having me.
Rovner: OK, we are back. It’s time for our extra-credit segment. That’s where we each recognize a story we read this week we think you should read, too. Don’t worry if you miss it. We will post the links in our show notes on your phone or other mobile device. Jessie, why don’t you go first this week?
Hellmann: My story is from The Texas Tribune, from a group of reporters who I can’t name individually. There’s too many of them. But it is in Texas after the governor issued an executive order a few years ago requiring that hospitals check patients’ citizenship. So the story found that hospital visits by undocumented people dropped by about a third, and the story also got into how this is bleeding into other types of health care at other facilities, free vaccine clinics are not being attended as widely anymore. People aren’t attending their preventive care appointments, like cancer screenings or prenatal care checkups. Some of these other health facilities are required to check citizenship status, but it’s definitely a chilling effect over the broader health care landscape in Texas.
Rovner: Yeah. There have been a lot of good stories about that. Sandhya.
Raman: My extra credit is from Science, and it’s by Jocelyn Kaiser, and the story is “.” In her story, she talks about how last year, you know, the administration cut a lot of staff at the Agency for Healthcare Research and Quality. They’ve canceled all of the open grants, but Congress still appropriated $345 million for the agency this year, and so supporters kind of want to revive what should be going on at the agency, which hasn’t been issuing any of the grants since the start of the fiscal year, and just kind of make progress on some of the things that this agency does do, like running the U.S. Preventive Services Task Force, which has been, you know, something that has been talked about this year. So thought it was an interesting piece.
Rovner: Yeah, I’m old enough to remember when AHRQ was bipartisan. Alice.
Ollstein: So a very harrowing story in The New York Times titled “.” And I will say, since this piece ran, we have seen that an oil shipment from Russia is going through to the island, but I don’t think that will be sufficient to completely wipe away all of the upsetting conditions that this piece really gets into, what is happening as a result of the ramped-up U.S. embargo and blockade of the island. People can’t get food, they can’t get medicine, they can’t get electricity, and that is having a devastating effect on health care. The Cuban health care system has been really miraculous over the years, just the pride of the government. It has meant, prior to this blockade, that their life expectancy was better than ours, and a lot of their outcomes were better. And so this has been really devastating. There’s, you know, harrowing scenes of people on ventilators having to be hand-pumped when the electricity cuts out, babies in incubators, you know, losing power. You know, people having to skip medications, etc. And so this is really shining a light on a foreign policy situation that this administration is behind.
Rovner: Yeah, that’s really been an under-covered story, too, I think, you know, right off our shores. My extra credit this week is one I simply could not resist. It’s from New York Magazine, and it’s called “,” by Helaine Olen. And as the headline rather vividly points out, we are witnessing the rise of pet medical tourism, along with human medical tourism, which has been a thing for a couple of decades now. It seems that veterinary medicine is getting nearly as expensive as human medicine, and that one way to find cheaper care is to cross the border, which is obviously easier if you live near the border. I’m not sure how much cheaper veterinary care is in Canada, but as the owner of two corgis, I may have to do some investigating of my own.
OK, that is this week’s show. As always, thanks to our editor, Emmarie Huetteman, and our producer-engineer, Francis Ying. A reminder: What the Health? is now available on WAMU platforms, the NPR app, and wherever you get your podcasts т as well as, of course, kffhealthnews.org. Also, as always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can find me still on X , or on Bluesky . Where are you folks hanging these days? Sandhya.
Raman: On and on .
Rovner: Alice.
Ollstein: On Bluesky and on X .
Rovner: Jessie.
Hellmann: I’m on LinkedIn under Jessie Hellmann and on X .
Rovner: We’ll be back in your feed next week. Until then, be healthy.
Credits
Click here to find all our podcasts.
And subscribe to “What the Health? From бюЙѓхњДЋУНвюl Health News” on , , , , , or wherever you listen to podcasts.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/podcast/what-the-health-440-gop-health-cuts-iran-april-2-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2177532&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
The Trump administration this week missed a deadline to nominate a new director for the Centers for Disease Control and Prevention. Without a nominee, current acting Director Jay Bhattacharya т who is also the director of the National Institutes of Health т has to give up that title, leaving no one at the helm of the nation’s primary public health agency.
Meanwhile, a week after one federal judge blocked changes to the childhood vaccine schedule made by the Department of Health and Human Services, another blocked a proposed ban on gender-affirming care for minors.
This week’s panelists are Julie Rovner of бюЙѓхњДЋУНвюl Health News, Rachel Cohrs Zhang of Bloomberg News, Lizzy Lawrence of Stat, and Shefali Luthra of The 19th.
Panelists



Among the takeaways from this week’s episode:
- A federal judge ruled against the Trump administration’s declaration intended to limit trans care for minors, though the ruling’s practical effects will depend on whether hospitals resume such care. And a key member of the remade federal vaccine advisory panel resigned as the panel’s activities т and even membership т remain in legal limbo.
- Two senior administration health posts remain unfilled, after President Donald Trump missed a deadline to fill the top job at the Centers for Disease Control and Prevention т and the Senate made little progress on confirming his nominee for surgeon general.
- The percentage of international graduates from foreign medical schools who match into U.S. residency positions has dropped to a five-year low. That’s notable given immigrants represent a quarter of physicians, many of them in critical but lower-paid specialties such as primary care т particularly in rural areas. Meanwhile, new surveys show that more than a quarter of labs funded by the National Institutes of Health have laid off workers and that federal research funding cuts have had a disproportionate effect on women and early-career scientists.
- And new data shows the number of abortions in the United States stayed relatively stable last year, for the second straight year т largely due to telehealth access to abortion care. And a vocal opponent of abortion in the Senate, with his eyes on a presidential run, introduced legislation to effectively rescind federal approval for the abortion pill mifepristone.
Also this week, Rovner interviews Georgetown Law Center’s Katie Keith about the state of the Affordable Care Act on its 16th anniversary.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: Stat’s “,” by John Wilkerson.
Shefali Luthra: NPR’s “,” by Tara Haelle.
Lizzy Lawrence: The Atlantic’s “,” by Nicholas Florko.
Rachel Cohrs Zhang: The Boston Globe’s “,” by Tal Kopan.
Also mentioned in this week’s podcast:
- Stat’s “,’” by Jonathan Wosen.
- бюЙѓхњДЋУНвюl Health News’ “Rising Health Costs Push Some Middle-Aged Adults To Skip the Doc Until Medicare,” by Sam Whitehead.
- Guttmacher’s “,” by Isaac Maddow-Zimet and Kimya Forouzan.
- United for Medical Research’s “.”
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, from бюЙѓхњДЋУНвюl Health News and WAMU Public Radio in Washington, D.C. Welcome to What the Health? I’m Julie Rovner, chief Washington correspondent for бюЙѓхњДЋУНвюl Health News, and I’m joined by some of the best and smartest reporters covering Washington. We’re taping this week on Thursday, March 26, at 10 a.m. As always, news happens fast, and things might have changed by the time you hear this. So, here we go.
Today, we are joined via video conference by Rachel Cohrs Zhang of Bloomberg News.
Rachel Cohrs Zhang: Hi, everybody.
Rovner: Shefali Luthra of The 19th.
Shefali Luthra: Hello.
Rovner: And Lizzy Lawrence of Stat News.
Lizzy Lawrence: Hello.
Rovner: Later in this episode we’ll have my interview with Katie Keith of Georgetown University about the state of the Affordable Care Act as it turns 16 т old enough to drive in most states. But first, this week’s news.
So, it has been another busy week at the Department of Health and Human Services. Last week, a federal judge in Massachusetts blocked the department’s vaccine policy, ruling it had violated federal administrative procedures regarding advisory committees. This week, a federal judge in Portland, Oregon, ruled the department also didn’t follow the required process to block federal reimbursement for transgender-related medical treatment. The case was brought by 21 Democratic-led states. Where does this leave the hot-button issue of care for transgender teens? Shefali, you’ve been following this.
Luthra: I mean, I think it’s still really up in the air. A lot of this depends on how hospitals now respond т whether they feel confident in the court’s decision, having staying power enough to actually resume offering services. Because a lot of them stopped. And so that’s something we’re still waiting to actually see how this plays out in practice. Obviously, it’s very symbolic, very legally meaningful, but whether this will translate into changes in practical health care access, I think, is an open question still.
Rovner: Yeah, we will definitely have to see how this one plays out т and, obviously, if and when the administration appeals it. Well, speaking of that vaccine ruling from last week т which, apparently, the administration has not yet appealed, but is going to т one of the most contentious members of that very contentious Advisory Committee on Immunization Practices has resigned. Dr. Robert Malone, a physician and biochemist, said he didn’t want to be part of the “drama,” air quotes. But he caused a lot of the drama, didn’t he?
Cohrs Zhang: He has been pretty outspoken, and I think he isn’t like a Washington person necessarily т isn’t somebody who’s used to, like, being on a public stage and having your social media posts appear in large publications. So I think it’s questionable, like, whether he had a position to resign from. I think his nomination was stayed, too. But I think it is тІ the back-and-forth, I think, there is a good point that this limbo can be frustrating for people when meetings are canceled at the last minute, and people have travel plans, and it does тІ just changes the calculus for kind of making it worth it to serve on one of these advisory committees.
Rovner: And I’m not sure whether we mentioned it last week, but the judge’s ruling not only said that the people were incorrectly appointed to ACIP, but it also stayed any meetings of the advisory committee until there is further court action, until basically, the case is done or it’s overruled by a higher court. So тІ vaccine policy definitely is in limbo.
Well, meanwhile, yesterday was the deadline for the administration to nominate someone to head the Centers for Disease Control and Prevention since Susan Monarez was abruptly dismissed, let go, resigned, whatever, late last summer. Now that that deadline has passed, it means that acting Director Jay Bhattacharya, who had added that title to his day job as head of the National Institutes of Health, can no longer remain acting director of CDC. Apparently, though he’s going to sort of remain in charge, according to HHS spokespeople, with some authorities reverting to [Health and Human Services] Secretary [Robert F.] Kennedy [Jr.]. What’s taking so long to find a CDC director?
To quote D.C. cardiologist and frequent cable TV health policy commentator , “The problem here is that there’s no candidate who’s qualified, MAHA acceptable, and Senate confirmable. Those job requirements are mutually exclusive.” That feels kind of accurate to me. Is that actually the problem? Rachel, I see you smiling.
Cohrs Zhang: Yeah. I think it is tough to find somebody who checks all of those boxes. And though it has been 210 days since the clock has started, I would just point out that there has been a significant leadership shake-up at HHS, like among the people who are kind of running this search, and they came in, you know, not that long ago. It’s only been, you know, a month and a half or so. So I think there certainly have been some new faces in the room who might have different opinions. But I think it isn’t a good look for them to miss this deadline when they have this much notice. But I think there’s also, like, legal experts that I’ve spoken with don’t think that there’s going to be a huge day-to-day impact on the operations of the CDC. It kind of reminds me of that office where there’s, like, an “assistant to the regional manager vibe” going on, where, like, Dr. Bhattacharya is now acting in the capacity of CDC director, even though he isn’t acting CDC director anymore. So, I think I don’t know that it’ll have a huge day-to-day impact, but it is kind of hanging over HHS at this point, as they are already struggling with the surgeon general nomination, to get that through the Senate. So it just creates this backlog of nominations.
Rovner: I’ve assumed they’ve floated some names, let us say, one of which is Ernie Fletcher, the former governor of Kentucky, also a former member of the House Energy and Commerce health subcommittee, with some certainly medical chops, if not public health chops. I think the head of the health department in Mississippi. There was one other who I’ve forgotten, who it is among the names that have been floated тІ
Cohrs Zhang: Joseph Marine. He’s a cardiologist at Johns Hopkins, who has т is kind of like in the kind of Vinay Prasad world of critics of the FDA and, like, CDC’s covid booster strategy.
Rovner: And yet, apparently, none of them could pass, I guess, all three tests. Do we think it might still be one of them? Or do we think there are other names that are yet to come?
Cohrs Zhang: Our understanding is that there are other candidates whose names have not become public, and I think there’s also a possibility they don’t choose any of these candidates and just drag it on for a while because, at this point, like, I don’t know what the rush is, now that the deadline is passed.
Lawrence: Yeah, is there another deadline to miss?
Cohrs Zhang: I don’t think so.
Lawrence: I think this was the only one.
Cohrs Zhang: This was the big one that they now have. It’s vacant, but it was vacant before as well. Like, I think, earlier in the administration, when Susan Monarez was nominated.
Rovner: But she, well тІ that’s right, she was the “acting,” and then once she was nominated, she couldn’t be the acting anymore.
Cohrs Zhang: Yeah.
Rovner: So I guess it was vacant while she was being considered.
Cohrs Zhang: It was. So it’s not an unprecedented situation, even in this administration. It’s just not a good look, I guess. And I think there is value in having a leader that can interface with the White House and with different leaders, and just having a direction for the agency, especially because it’s in Atlanta, it’s a little bit more removed from the everyday goings-on at HHS in general. So I think there’s definitely a desire for some stability over there.
Rovner: And we have measles spreading in lots more states. I mean, every time I тІ open up my news feeds, it’s like, oh, now we have measles, you know, in Utah, I think, in Montana. Washtenaw County, Michigan, had its first measles case recently. So this is something that the CDC should be on top of, and yet there is no one on top of the CDC. Well, Rachel, you already alluded to this, but it is also apparently hard to find a surgeon general who’s both acceptable to MAHA and Senate confirmable, which is my way of saying that the Casey Means nomination still appears to lack the votes to move out of the Senate, Health, Education, Labor & Pensions Committee. Do we have any latest update on that?
Cohrs Zhang: I think the latest update, I mean, my colleagues at Bloomberg Government just kind of had an update this week that they’re still not to “yes” т like, there are some key senators that still haven’t announced their positions publicly. So I think a lot of the same things that we’ve been hearing тІ like Sens. Susan Collins and Lisa Murkowski and Bill Cassidy obviously have not stated their positions publicly on the nomination. Sen. Thom Tillis, who you know is kind of in a lame-duck scenario and doesn’t really have anything to lose, has, you know, said he’s not really made a decision. So I think they’re kind of in this weird limbo where they, like, don’t have the votes to advance her, but they also have not made a decision to pull the nomination at this time. So either, I think, they have to push harder on some of these senators, and I think senators see this as a leverage point that I don’t know that a lot of т that all of the complaints are about Dr. Means specifically, but anytime that there is frustration with the wider department, then this is an opportunity for senators to have their voice heard, to тІ potentially extract some concessions. And so there’s a question right now, are they going to change course again for this position, or are they going to, you know, sit down at the bargaining table and really cut some deals to advance her nomination? I just don’t think we know the answer to that yet.
Rovner: Yeah, it’s worth reminding that, frequently, nominations get held up for reasons that are totally disconnected from the person involved. We went т I should go back and look this up т we went, like, four years in two different administrations without a confirmed head of the Centers for Medicare & Medicaid Services because members of Congress were angry about other things, not because of any of the people who had actually been nominated to fill that position. But in this case, it does seem to be, I think, both Casey Means and, you know, her connection to MAHA, and the fact that among those who haven’t declared their positions yet, it’s the chairman of the committee, Bill Cassidy, who’s in this very tight primary to keep his seat. So we will keep on that one.
Also, meanwhile, HHS continues to push its Make America Healthy Again priority. Secretary Kennedy hinted on the Joe Rogan podcast last month that the FDA will soon take unspecified action to make customized peptides easier to obtain from compounding pharmacies. These mini-proteins are part of a biohacking trend that many MAHA adherents say can benefit health, despite their not having been shown to be safe and effective in the normal FDA approval process. The FDA has also formally pulled a proposed rule that would have banned teens from using tanning beds. We know that the secretary is a fan of tanning salons, even though that has been shown to cause potential health problems, like skin cancer. Lizzy, is Kennedy just going to push as much MAHA as he can until the courts or the White House stops him?
Lawrence: I guess so. I mean, we do have this new structure at HHS now that’s trying to т clearly тІ there are warring factions with the MAHA agenda and the White House really trying to focus more on affordability and less on тІ vaccine scrutiny and the medical freedom movement that is really popular among Kennedy’s supporters. тІ I’m very curious about what’s going to happen with peptides, because it’s a sign of Kennedy’s regulatory philosophy, where there’s some products that are good and some that are bad. It’s very atypical, of course, for тІ
Rovner: And that he gets to decide rather than the scientists, because he doesn’t trust the scientists.
Lawrence: Right. Right. But there has been, I mean, the FDA has kind of been pretty severe on GLP-1 compounders Hims & Hers, so it’ll be interesting to see, you know, how much Kennedy is able to exert his will here, and how much FDA regulators will be able to push back and make their voices heard.
Rovner: My favorite piece of FDA trivia this week is that FDA is posting the jobs that are about to be vacant at the vaccine center, and one of the things that it actually says in the job description is that you don’t have to be immunized. I don’t know if that’s a signal or what.
Lawrence: Yeah, I think it said no telework, which Vinay Prasad famously was teleworking from San Francisco. So, yeah, I don’t know. But this was, I think it was for his deputy, although I’m sure, I mean, they do need a CBER [Center for Biologics Evaluation and Research] director as well.
Rovner: Yeah, there’s a lot of openings right now at HHS. All right, we’re gonna take a quick break. We will be right back.
So Monday was the 16th anniversary of the signing of the Affordable Care Act, which we will hear more about in my interview with Katie Keith. But I wanted to highlight a story by my KFF Health News colleague Sam Whitehead about older Americans nearing Medicare eligibility putting off preventive and other care until they qualify for federal coverage that will let them afford it. For those who listened to my interview last week with Drew Altman, this hearkens back to one of the big problems with our health system. There are so many quote-unquote “savings” that are actually just cost-shifting, and often that cost-shifting raises costs overall. In this case, because those older people can no longer afford their insurance or their deductibles, they put off care until it becomes more expensive to treat. At that point, because they’re on Medicare, the federal taxpayer will foot a bill that’s even bigger than the bill that would have been paid by the insurance company. So the savings taxpayers gained by Congress cutting back the Affordable Care Act subsidies are lost on the Medicare end. Is this cost-shifting the inevitable outcome of addressing everything in our health care system except the actual prices of medical care?
Cohrs Zhang: I think it’s just another example of how people’s behavior responds to these weird incentives. And I think we’re seeing this problem, certainly among early retirees, exacerbated by the expiration of the Affordable Care Act subsidies that we’ve talked about very often on this podcast, because it affects these higher earners, and it can dramatically increase costs for coverage. And I think people just hope that they can hold on. But again, these statutory deadlines that lawmakers make up sometimes, not with a lot of forethought or rational reasoning, they have consequences. And obviously, the Medicare program continues to pay beyond age 65 as well. And I think it’s just another symptom of what the administration talks about when they talk about emphasizing, you know, preventative care and addressing chronic conditions т like, that is a real problem. And, yeah, I think we’re going to see these problems in this population continue to get worse as more people forgo care, as it becomes more expensive on the individual markets.
Luthra: I think you also make a good point, though, Julie, because the increase in costs and cost sharing is not limited to people with marketplace plans, right? Also, people with employer-sponsored health care are seeing their out-of-pocket costs go up. Employers are seeing what they pay for insurance go up as well. And there absolutely is something to be said about it’s been 16 years since the Affordable Care Act passed, we haven’t really had meaningful intervention on the key source of health care prices, right? Hospitals, providers, physicians. And it does seem, just thinking about where the public is and the politics are, that there is possibly appetite around this. You see a lot of talk about affordability, but a lot of this feels, at least as an observer, very focused on insurance, which makes sense. Insurance is a very easy villain to cast. But I think you’ve raised a really good point: that addressing these really potent burdens on individuals and eventually on the public just requires something more systemic and more serious if we actually want to yield better outcomes.
Rovner: Yeah, there’s just, there’s so much passing the hat that, you know, I don’t want to do this, so you have to do this. You know, inevitably, people need health care. Somebody has to pay for it. And I think that’s sort of the bottom line that nobody really seems to want to address.
Well, the other theme of 2026 that I feel like I keep repeating is what funding cutbacks and other changes are doing to the future of the nation’s biomedical and medical workforces. Last week was Match Day. That’s when graduating medical school seniors find out if and where they will do their residency training. One big headline from this year’s match is that the percentage of non-U.S. citizen graduates of foreign medical schools matching to a U.S. residency position fell to a five-year low of 56.4%. That compares to a 93.5% matching rate for U.S. citizen graduates of U.S. medical schools. Why does that matter? Well, a quarter of the U.S. physician workforce are immigrants, and they are disproportionately represented, both in lower-paid primary care specialties, particularly in rural areas, both of which U.S. doctors tend to find less desirable. This would seem to be the result of a combination of new fees for visas for foreign professionals that we’ve talked about, a general reduction in visa approvals, and some people likely not wanting to even come to the U.S. to practice. But that rural health fund that Republicans say will revitalize rural health care doesn’t seem like it’s really going to work without an adequate number of doctors and nurses, I would humbly suggest.
Lawrence: Yeah, absolutely. I mean, it’s patients that suffer, right? I mean, you need the people doing the work. And so I think that the impacts will start being felt sooner rather than later. That is something that hopefully people will start to feel the pain from.
Rovner: I feel like when people think about the immigrant workforce, they think about lower-skilled, lower-paid jobs that immigrants do, and they don’t think about the fact that some of the most highly skilled, highly paid jobs that we have, like being doctors, are actually filled by immigrants, and that if we cut that back, we’re just going to exacerbate shortages that we already know we have.
Luthra: And training doctors takes, famously, a very long time. And so if you are disincentivizing people from coming here to practice, cutting off this key source of supply, it’s not as if you can immediately go out and say, Here, let’s find some new people and make them doctors. It will take years to make that tenable, make that attractive, and make that a reality. And it just seems, to Lizzy’s point, that even in the scenario where that was possible т which I would be somewhat doubtful; medicine is a hard and difficult career; it’s not like you can make someone want to do that overnight т patients will absolutely see the consequences. I don’t know if it’s enough to change how people think about immigration policy and ways in which we recruit and engage with immigrant workers, but it’s absolutely something that should be part of our discussion.
Rovner: Yeah, and I think it’s been left out. Well, meanwhile, over at the National Institutes of Health, a , Lizzy, found that more than a quarter have laid off laboratory workers. More than 2 in 5 have canceled research, and two-thirds have counseled students to consider careers outside of academic research. A separate study published this week found that women and early-career scientists have been disproportionately affected by the NIH cuts, even though most of the money goes to men and to later-career scientists. As I keep saying, this isn’t just about the future of science. Biomedical research is a huge piece of the U.S. economy. Earlier this month, the group United for Medical Research , finding that every dollar invested produced $2.57 for the economy. Concerned members of Congress from both parties last week at an appropriations hearing got NIH Director Jay Bhattacharya to again promise to push all the money that they appropriated out the door. But it’s not clear whether it’s going to continue to compromise the future workforce. I feel like, you know, we talk about all these missing people and nomination stuff, but we’re not really talking a lot about what’s going on at the National Institutes of Health, which is a, you know, almost $50 billion-a-year enterprise.
Lawrence: Right. In some labs, the damage has already been done. You know, even if Dr. Bhattacharya [follows through], try spending all the money that has been appropriated. There are young researchers that have been shut out and people that have had to choose alternative career paths. And I think this is one of those things that’s difficult politically or, you know, in the public consciousness, because it is hard to see the immediate impacts it’s measured. And I think my colleague Jonathan wrote [that] breakthroughs are not discovered things, you know. So it’s hard to know what is being missed. But the immediate impact of the workforce and not missing this whole generation of scientists that has decided to go to another country or go to do something else, those impacts will be felt for years to come.
Rovner: Yeah, this is another one where you can’t just turn the spigot back on and have it immediately refill.
Finally, this week, there is always reproductive health news. This week, we got the Alan Guttmacher Institute’s for the year 2025, which both sides of the debate consider the most accurate, and it found that for the second year in a row, the number of abortions in the U.S. remained relatively stable, despite the fact that it’s outlawed or seriously restricted in nearly half the states. Of course, that’s because of the use of telehealth, which abortion opponents are furiously trying to get stopped, either by the FDA itself or by Congress. Last week, anti-abortion Sen. Josh Hawley of Missouri introduced legislation that would basically rescind approval for the abortion pill mifepristone. But that legislation is apparently giving some Republicans in the Senate heartburn, as they really don’t want to engage this issue before the midterms. And, apparently, the Trump administration doesn’t either, given what we know about the FDA saying that they’re still studying this. On the other hand, Republicans can’t afford to lose the backing of the anti-abortion activists either. They put lots of time, effort, and money into turning out votes, particularly in times like midterms. How big a controversy is this becoming, Shefali?
Luthra: This is a huge controversy, and it’s so interesting to watch this play out. When I saw Sen. Hawley’s bill, I mean, that stood out to me as positioning for 2028. He clearly wants to be a favorite among the anti-abortion movement heading into a future presidential primary. But at the same time, this is teasing out really potent and powerful dynamics among the anti-abortion movement and Republican lawmakers, exactly what you said. Republican lawmakers know this is not popular. They do not want to talk about abortion, an issue at which they are at a huge disadvantage with the public. Susan B Anthony List and other such organizations are trying to make the argument that if they are taken for granted, as they feel as if they are, that will result in an enthusiasm gap. Right? People will not turn out. They will not go door-knocking, they won’t deploy their tremendous resources to get victories in a lot of these contested, particularly Senate and House, races. And obviously, the president cares a lot about the midterms. He’s very concerned about what happens when Democrats take control of Congress. But I think what Republicans are wagering, and it’s a fair thought, is that where would anti-abortion activists go? Are they going to go to Democrats, who largely support abortion rights? And a lot of them seem confident that they would rather risk some people staying home and, overall, not alienating a very large sector of the American public that does not support restrictions on abortion nationwide, especially those that many are concerned are not in keeping with the actual science.
Rovner: Yeah, I think the White House, as you said, would like to make this not front and center, let’s put it that way, for the midterms. But yeah, and just to be clear, I mean, Sen. Hawley introduced this bill. It can’t pass. There’s no way it gets 60 votes in the Senate. I’d be surprised if it could get 50 votes in the Senate. So he’s obviously doing this just to turn up the heat on his colleagues, many of whom are not very happy about that.
Luthra: And anti-abortion activists are already thinking about 2028. They are, in fact, talking to people like Sen. Hawley, like the vice president, like Marco Rubio, trying to figure out who will actually be their champion in a post-Trump landscape. And so far, what I’m hearing, is that they are very optimistic that anyone else could be better for them than the president is because they are just so dissatisfied with how little they’ve gotten.
Rovner: Although they did get the overturn of Roe v. Wade.
Luthra: That’s true.
Rovner: But you know, it goes back to sort of my original thought for this week, which is that the number of abortions isn’t going down because of the relatively easy availability of abortion pills by mail. Well, speaking of which, in a somewhat related story, a woman in Georgia has been charged with murder for taking abortion pills later in pregnancy than it’s been approved for, and delivering a live fetus who subsequently died. But the judge in the case has already suggested the prosecutors have a giant hill to climb to convict her and set her bail at $1. Are we going to see our first murder trial of a woman for inducing her own abortion? We’ve been sort of flirting with this possibility for a while.
Luthra: It seems possible. I think it’s a really good question, and this moment certainly feels like a possible Rubicon, because going after people who get abortions is just so toxic for the anti-abortion movement. They have promised they would not go after people who are pregnant, who get abortions. And this is exactly what they are doing. And I think what really stands out to me about this case is so much of it depends on individual prosecutors and individual judges. You have the law enforcement officials who decided to make this a case, and they’re actually using, not the abortion law, even though the language in the case, right, really resonates, reflects with the law in Georgia’s six-week ban. Excuse me, with the language in Georgia’s six-week ban. But then you have a judge who says this is very suspect. And what feels so significant is that your rights and your protection under abortion laws depend not only on what state you live in, but who happens to be the local prosecutor, the local cop, the local judge, and that’s just a level of micro-precision that I think a lot of Americans would be very surprised to realize they live under.
Rovner: Yeah, absolutely. We should point out that the woman has been charged but not yet indicted, because many, many people are watching this case very, very carefully. And we will too.
All right, that is this week’s news. Now I’ll play my interview with Katie Keith of Georgetown University Law Center, and then we’ll come back with our extra credits.
I am pleased to welcome back to the podcast Katie Keith. Katie is the founding director of the Center for Health Policy and the Law at the Georgetown University Law Center and a contributing editor at Health Affairs, where she keeps all of us up to date on the latest health policy, legal happenings. Katie, thanks for joining us again. It’s been a minute.
Katie Keith: Yeah. Thanks for having me, Julie, and happy ACA anniversary.
Rovner: So you are my go-to for all things Affordable Care Act, which is why I wanted you this week in particular, when the health law turned 16. How would you describe the state of the ACA today?
Keith: Yeah, it’s a great question. So, the ACA remains a hugely important source of coverage for millions of people who do not have access to job-based coverage. I am thinking of farmers, and self-employed people, and small-business owners. And you know, in 2025, more than 24 million people relied on the marketplaces all across the country for this coverage. So it remains a hugely important place where people get their health insurance. And we are already starting to see real erosion in the gains made under the Biden administration as a result of, I think, three primary changes that were made in 2025. So the first would be Congress’ failure to extend the enhanced premium tax credits, which you have covered a ton, Julie and the team, as having a huge impact there. The second is the changes from the One Big Beautiful Bill Act. And then the third is some of the administrative changes made by the Trump administration that we’re already seeing. So we don’t yet have full data to understand the impact of all three of those things yet. We’re still waiting. But the preliminary data shows that already enrollments down by more than a million people. I’m expecting that to drop further. There was some KFF survey data out last week that about 1 in 10 people are going uninsured from the marketplace already, and that’s not even, doesn’t even account for all the people who are paying more but getting less, which their survey data shows is about, you know, 3 in 10 folks. So you know what makes all of this really, really tough, as you and I have discussed before, is, I think, 2025, was really a peak year. We saw peak enrollment at the ACA. We saw peak popularity of the law, which has been more popular than not ever since 2017, when Republicans in Congress tried to repeal it the first time. And тІ but now it feels like we’re sort of on this precipice for 2026, watching what’s going to happen with the data into this really important source of coverage for so many people.
Rovner: And тІ there’s been so much news that I think it’s been hard for people to absorb. You know, in 2017, when Republicans tried to repeal the Affordable Care Act, they said that, We’re trying to repeal the Affordable Care Act. Well, the 2025 you know, “Big, Beautiful Bill,” they didn’t call it a repeal, but it had pretty much the same impact, right?
Keith: It had a quite significant impact. And I think a lot, like, you know, there was so much coverage about how Democrats in Congress and the White House learned, in doing the Affordable Care Act, learned from the failed effort of the Clinton health reform in the ’90s. I think similarly here you saw Republicans in Congress, in the White House, learn from the failed effort in 2017 to be successful here. And so you’re exactly right. You did not hear any talk of “repeal and replace,” by any stretch of the imagination. I think in 2017 Republicans were judged harshly т and appropriately so, in my opinion т by the “replace” portion of what, you know, what they were going to do, and it just wasn’t there. And so you did not see that kind of framing this time around. Instead, it really is an attempt to do death by a thousand paper cuts and impose administrative burdens and a real focus on kind of who т you can’t see me, but air quotes, you know т who “deserves” coverage and a focus on immigrant populations. So тІ those changes, when you layer all of them on т changes to Medicaid coverage, Medicaid financing, paperwork burdens, all across all these different programs т you know, the One Big Beautiful Bill Act, it really does erect new barriers that fundamentally change how Medicaid and the Affordable Care Act will work for people. And so it’s not repealed. I think those programs will still be there, but they will look very different than how they have and, you know, the CBO [Congressional Budget Office] at the time, the coverage losses almost тІ they look quite close to, you know, the skinny repeal that we all remember in the middle of the morning т early, like, late night, Sen. John McCain with his thumbs down. The coverage losses were almost the same, and you’ve got the CBO now saying, estimating about 35 million uninsured people by 2028, which, you know, is not тІ it’s just erasing, I think, not all, but a lot of the gains we’ve made over the past 15, now 16, years under the Affordable Care Act.
Rovner: And now the Trump administration is proposing still more changes to the law, right?
Keith: Yep, that’s right. They’re continuing, I think, a lot of the same. There’s several changes that, you know, go back to the first Trump administration that they’re trying to reimpose. Others are sort of new ideas. I’m thinking some of the same ideas are some of the paperwork burdens. So really, in some cases, building off of what has been pushed in Congress. What’s maybe new this time around for 2027 that they’re pushing is a significant expansion of catastrophic plans. So huge, huge, high-deductible plans that, you know, really don’t cover much until you hit tens of thousands of dollars in out-of-pocket costs. You get your preventive services and three primary care visits, but that’s it. You’re on the hook for anything else you might need until you hit these really catastrophic costs. They’re punting to the states on core things like network adequacy. You know, again, some of it’s sort of new. Some of it’s a throwback to the first Trump administration, so not as surprising. And then on the legislative front, I don’t know what the prospects are, but you do continue to see President [Donald] Trump call for, you know, health savings account expansions. We think, I think, you know, the idea is to send people money to buy coverage, rather than send the money to the insurers, which I think folks have interpreted as health savings accounts. There’s a continued focus on funding cost-sharing reductions, but that issue continues to be snarled by abortion restrictions across the country. So that’s something that continues to be discussed, but I don’t know if it will ever happen. And you know anything else that’s kind of under the so-called Great Healthcare Plan that the White House has put out.
Rovner: You mentioned that 2025 was the peak not just of enrollment but of popularity. And we have seen in poll after poll that the changes that the Trump administration and Congress is making are not popular with the public, including the vast majority of independents and many, many Republicans as well. Is there any chance that Congress and President Trump might relent on some of these changes between now and the midterms? We did see a bunch of Republicans, you know, break with the rest of the party to try to extend the, you know, the enhanced premiums. Do you see any signs that they’re weakening or are we off onto other things entirely right now?
Keith: It’s a great question. I think you probably need a different analyst to ask that question to. I don’t think my crystal ball covers those types of predictions. But to your point, Julie, I thought that if there would have been time for a compromise and sort of a path forward, it would have been around the enhanced premium tax credits. And it was remarkable, you know, given what the history of this law has been and the politics surrounding it, to see 17 Republicans join all Democrats in the House to vote for a clean three-year extension of the premium tax credits. But no, I think especially thinking about where those enhanced tax credits have had the most benefit, it is states like Georgia, Florida, Texas, and I thought that maybe would, could have moved the needle if there was a needle to be moved. So I, it seems like there’s much more focus on prescription drugs and other issues, but anything can happen. So I guess we’ll all stay tuned.
Rovner: Well, we’ll do this again for the 17th anniversary. Katie Keith, thank you so much.
Keith: Thanks, Julie.
Rovner: OK, we’re back. It’s time for our extra-credit segment. That’s where we each recognize a story we read this week we think you should read too. Don’t worry if you miss it. We will post the links in our show notes on your phone or other mobile device. Lizzy, why don’t you start us off this week?
Lawrence: Sure. So my extra credit is by Nick [Nicholas] Florko, former Stat-ian, in The Atlantic, “” I immediately read this piece, because this is something that’s been driving me kind of crazy. Just seeing т if you’ve missed it т there have been тІ HHS has been posting AI-generated videos of Secretary Kennedy wrestling a Twinkie, wearing waterproof jeans, all of these things. And this has been, this is not unique to HHS т [the] White House in general has really embraced AI slop as a genre, and I can’t look away. And so I thought Nick did a good job just acknowledging how crazy this is, and then also what goes unsaid in these videos. I think I personally am just very curious if this resonates with people, or if it’s kind of disconcerting for the average American seeing these videos like, Oh, my government is making AI slop. Like I, you know, social media strategy is so important, so maybe for some people are really liking this. But yeah, I’m just kind of curious about public sentiment.
Rovner: I know I would say, you know, the National Park Service and the Consumer Product Safety Commission have been sort of famous for their very cutesy social media posts, but not quite to this extent. I mean, it’s one thing to be cheeky and funny. This is sort of beyond cheeky and funny. I agree with you. I have no idea how this is going over the public, but they keep doing it. It’s a really good story. Rachel.
Cohrs Zhang: Mine is a story in The Boston Globe, and the headline is “” by Tal Kopan. And this was a really good profile of Tony Lyons, who is Robert F. Kennedy Jr.’s book publisher, and he’s kind of had the role of institutionalizing all the political energy behind RFK Jr. and trying to make this into a more enduring political force. So I think he is, like, mostly a behind-the-scenes guy, not really like a D.C. fixture, more of like a New York book publishing figure. But I think his efforts and what they’re using, all the money they’re raising for, I think, is a really important thing to watch in the midterms, and like, whether they can actually leverage this beyond a Trump administration, or beyond however long Secretary Kennedy will be in his position. So I think it was just a good overview of all the tentacles of institutional MAHA that are trying to, you know, find their footing here, potentially for the long term.
Rovner: I had never heard of him, so I was glad to read this story. Shefali.
Luthra: My story is from NPR. It is by Tara Haelle. The headline is “.” Story says exactly what it promises, that if you have an infant, babies under 6 months, then getting a covid vaccine while you are pregnant will actually protect your baby, which is great because there is no vaccine for infants that young. I love this because it’s a good reminder of something that we were starting to see, and now it just really underscores that this is true, and in the midst of so much conversation around vaccines and safety and effectiveness, it’s a reminder that really, really good research can show us that it is a very good idea to take this vaccine, especially if you are pregnant.
Rovner: More fodder for the argument, I guess. All right, my extra credit this week is a clever story from Stat’s John Wilkerson called “.” And, spoiler, that loophole is that one way companies can avoid running afoul of their promise not to charge other countries less for their products than they charge U.S. patients is for them to simply delay launching those drugs in those other countries that have price controls. Already, most drugs are launched in the U.S. first, and apparently some of the companies that have done deals with the administration limited their promises to three years, anyway. That way they can charge U.S. consumers however much they think the market will bear before they take their smaller profits overseas. Like I said, clever. Maybe that’s why so many companies were ready to do those deals.
All right, that is this week’s show. As always, thanks to our editor, Emmarie Huetteman; our producer-engineer, Francis Ying; and our interview producer, Taylor Cook. A reminder: What the Health? is now available on WAMU platforms, the NPR app, and wherever you get your podcasts, as well as, of course, kffhealthnews.org. Also, as always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can still find me on X or on Bluesky . Where are you folks hanging these days? Shefali?
Luthra: I am on Bluesky .
Rovner: Rachel.
Cohrs Zhang: On X , or .
Rovner: Lizzy.
Lawrence: I’m on X and and .
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
Click here to find all our podcasts.
And subscribe to “What the Health? From бюЙѓхњДЋУНвюl Health News” on , , , , , or wherever you listen to podcasts.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/podcast/what-the-health-439-cdc-lacks-leader-march-26-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2173869&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>He was already thinking about delaying it т then his monthly Obamacare insurance premium payment tripled this year to $2,460, about a third of his income, he said. And with a $2,700 deductible, he’d be on the hook for most of the diagnostic exam, a financial hit he said he couldn’t stomach.
“It was going to cost close to $3,000,” said Galvin, who lives in North Kingstown, Rhode Island, and recently retired as director of a durable medical equipment company. “I put it off.”
Galvin said his wife, Nancy, is delaying a costly CT scan for a few years until she too qualifies for Medicare, so it can foot the bill. The federal health program offers coverage for all Americans 65 and older.
People on Affordable Care Act plans nearing retirement age experienced some of the largest price increases following the expiration of enhanced federal subsidies at the end of December. Those with incomes above 400% of the federal poverty level т т had been getting help paying for the plans since the Biden administration expanded the subsidies during the covid-19 pandemic. Adults ages 50 through 64 of those ACA enrollees.
Now, without that federal financial help, some in this age group say they’re wrestling with whether to delay care until they qualify for Medicare. Not only does that put their physical health at risk, said patient advocates, doctors, and health policy researchers, but it potentially just shifts the costs т and could lead to taxpayers’ footing even bigger bills to fix health issues that worsen amid the delays.
“There’s going to be a lot of pent-up demand and unmet need,” said , a health policy consultant who worked in the Obama and Biden administrations. “Medicare is going to have to spend a whole heck of a lot of money covering and dealing with their treatment.”
The Affordable Care Act has been a key source of health care coverage for people 50 through 64. Access to Obamacare plans helped cut the uninsured rate for this age group by half, , a lobbying group that represents older adults. That allowed some people to retire early while keeping coverage. It also has provided a safety net for small-business owners and those with jobs that don’t offer health insurance.
Last fall, the longest-ever government shutdown occurred amid an unsuccessful effort by Democrats to extend the enhanced subsidies. Republicans opposing the extension had said the assistance went to insurers, incentivizing fraud and wasteful coverage.
The issue will continue to have political relevance, especially in this year’s midterm elections, including among older Americans who reliably show up to the polls, said Republican strategist , who runs the Atlas Strategy Group.
“Is affordability going to be an issue? Absolutely,” he said. “Are health care prices going to factor into that? Yes.”
Even before the subsidies expired, the costs of medical care, nursing homes, and prescription drugs were among the top health-related concerns for people over 50, a found.
Middle-aged adults with Obamacare plans acutely feel the pinch of the expired subsidies, because to charge adults in their 60s up to three times as much for premiums as those in their 20s, who generally use fewer medical services.
And many middle-aged adults were already enrolled in the lowest-cost plans available, which leaves them without cheaper options to fall back on, said , a policy analyst with KFF, a health information nonprofit that includes бюЙѓхњДЋУНвюl Health News.
“This is very dire for the older marketplace enrollees,” he said.
Someone making a few dollars over 400% of the federal poverty level earns too much to get a subsidy now, and in some states average premium payments were due to for this group. Many people are seeing yearly rate increases of thousands of dollars, with premium payments totaling as much as a quarter of their incomes.
, a primary care physician and health policy researcher at the University of Michigan, said he has regular conversations with older patients who are trying to figure out how to afford their medical care. Some in their early 60s are likely to drop ACA coverage because of rising premiums, he said.
“That’s a gamble,” he added.
Marci Heinbaugh may take that bet. The 63-year-old social services worker, who lives in rural Illinois, said her monthly premium payments more than doubled, from roughly $1,100 to $2,333, for a plan with a $10,150 out-of-pocket maximum.
She knew she’d be paying more, she said, but wasn’t anticipating that kind of increase. A few months in, she’s not sure if she’ll stick with the plan for the rest of the year. She said she may go uninsured.
“I’m petrified to even think about that,” Heinbaugh said.
People want to buy their own insurance on the marketplace, and many middle-aged adults could afford it with just a little federal financial help, said , senior vice president of public policy at AARP. Those who drop coverage or delay care until they reach age 65 might save money now, but that could be more costly for them т and taxpayers т later.
“There’s significant possibility that the purported savings associated with reducing subsidies as people approach retirement end up turning into higher utilization costs for Medicare,” Weil said.
And Medicare enrollees aren’t insulated from rising costs. In January, for example, standard Medicare from $185 per month to almost $203.
Until Galvin joins Medicare, he said, he expects to burn through a $30,000 retirement account to cover his marketplace plan’s premium payments and deductible.
A found that 1 in 5 adults over 50 had no retirement savings and 3 in 5 were worried they wouldn’t have enough retirement savings to support themselves.
The expiration of these Obamacare subsidies puts additional financial pressure on Americans as they approach retirement, health policy researchers said.
“It’s forcing people to make impossible choices,” said , director of federal health advocacy for the national nonprofit Justice in Aging.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here to contact бюЙѓхњДЋУНвюl Health News and share your story.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/health-costs-middle-aged-adults-delay-affordable-care-act-obamacare-medicare/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2169414&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Oz, who heads the U.S. Centers for Medicare & Medicaid Services, there was approximately $3.5 billion of fraud in the hospice and home health care industry in Los Angeles County alone. “This administration under President [Donald] Trump is not going to tolerate taxpayer dollars being stolen because people aren’t paying attention anymore. We’re focused on this,” . He claimed the fraud was largely orchestrated by the “Russian, Armenian mafia” and said that most of the money spent on home and community-based services across California “might be fraudulent.”
However, CMS clarified that not all billing activities referenced by Oz were presumed to be improper. And a review of the most recent available data shows that there are hotbeds of health care fraud across the country and across practice areas, most of them allegedly perpetrated by health insurers and other domestic actors, and that California outperforms most other states in recovering fraud dollars.
As the temperature heats up in the conflict between the Trump administration and California, a handful of Republican state lawmakers have entered the fray, accusing Gov. Gavin Newsom in of allowing “rampant fraud.” Democratic state officials insist they aggressively combat fraud, and Newsom has filed a against Oz, calling language in the allegations “baseless and racially charged.”
“The Trump Administration is attempting to take the issue of fraud т a very real, and national issue т and weaponize it against Democratic states,” California Attorney General Rob Bonta said in an early February statement.
Oz said that he would halt “hundreds of millions of dollars” in payments to California if he didn’t get satisfactory answers from state officials. He and Vice President JD Vance announced in late February that they would delay about $260 million in Medicaid payments , another Democratic-led state, over fraud allegations there, and the state is now suing.
Oz has also launched social media campaigns alleging high-dollar public benefit fraud in Democratic-led Maine and New York. On March 17, he added a Republican-led state to his target list: Florida.
Georgetown University professor Andy Schneider, who served as a senior adviser primarily on Medicaid integrity issues during the Obama administration, said fraud has always been an issue across states, dating back decades. About $3.4 billion in Medicare and Medicaid fraud across the country was , according to the most recent report available. Insurers have paid the highest settlements in alleged health care fraud schemes.
“Bad actors trying to steal public health care funds have been around for a long time,” Schneider said.
How California Stacks Up
The federal government is responsible for Medicare, which primarily benefits older people, while Medicaid, which primarily serves people with lower incomes, is a joint federal-state program. Melissa Rumley, a spokesperson for the Department of Health and Human Services’ Office of Inspector General, said the office could not make state-by-state data on Medicare fraud available because the federal probes often cross jurisdictions.
States file annual reports on actions by Medicaid anti-fraud units that are jointly funded with the federal government and run by state attorneys general. They investigate fraud as well as abuse and neglect of Medicaid patients.
These reports provide a sense of the scale of Medicaid fraud across states. In fiscal 2024, states recovered , compared with $949 billion in total Medicaid spending, according to from the HHS Office of Inspector General. California recouped an outsize share, recovering more than 50% of all the criminal recoveries made by the anti-fraud units nationwide in fiscal 2024 even though the state made up only about 17% of enrollment.
California ranked fourth in the U.S. in 2024 in dollars recovered per Medicaid enrollee across civil and criminal investigations, behind the District of Columbia, Montana, and Delaware. It led all the most populous states, followed in order by Texas, Florida, and New York. (California and federal officials noted that state recovery data varies significantly year to year, often because of the length of investigations.)
Vulnerability of Hospice Care
One aspect of health care fraud that has been at the center of Oz’s attack on California is hospice fraud, which has plagued Republican and Democratic administrations.
The use of hospice, intended to provide care to patients expected to die within six months, increased by over 8% from fiscal 2020 to 2024, to about 1.84 million Medicare beneficiaries, significantly.
To combat fraud, the Biden administration in 2023 of hospices in California, Arizona, Nevada, and Texas. The Trump administration Ohio and Georgia.
CMS spokesperson Chris Krepich did not say specifically what criteria were used to choose which states to monitor, only that the decision was based on “activity typically indicative of hospice-related fraud.” As of June, the agency had revoked the Medicare enrollment of 122 hospices in the original four states, but Krepich said a breakdown by state was not available.
While Oz stated there was some $3.5 billion of fraud in the hospice and home health care industry in Los Angeles County alone, his agency clarified that the number is for overall Medicare billing related to hospice and home health services. Krepich said that “not all billing activity referenced in the remarks is presumed to be improper” and added that the agency could not identify the amount of fraudulent activity until an “evidence-based” investigation was completed.
That’s not to say there is no truth to allegations of hospice fraud.
A published in 2022 found “numerous indicators” of large-scale fraud in Los Angeles County, and a highlighted nearly 500 hospices within a 3-mile radius, including 89 companies registered to a single building in Van Nuys. that “hospice fraud has become an epidemic in California.” He noted that state officials have been aggressively combating it for years, including with .
In January, the state in Monterey County with hospice fraud. That follows hospice scam cases in and .
However, California public health officials are overdue in adopting that were supposed to be . The state’s Department of Public Health is currently revising the regulations, according to spokesperson Mark Smith.
In the interim, the state has revoked the licenses of more than 280 hospices over the past two years and is evaluating an additional 300 hospices, . California had licensed hospice agencies as of 2022, according to the state audit.
Civil Rights Complaint
Meanwhile, Newsom is pushing back on Oz. The governor filed his discrimination complaint with the at HHS, which oversees CMS. The office said it will first decide whether it has the authority to investigate, then, if so, will gather information through interviews and documents. However, the process seems designed to aid individuals who have lost a job to discrimination, or to correct a specific policy, and it is unclear whether there could be any real-world consequences.
The governor wants the agency to address “systematic bias from their leadership,” said Newsom spokesperson Marissa Saldivar.
Krepich said CMS “does not target communities, ethnic groups, or states” and bases its decisions on “confirmed investigative findings.” The allegations of organized fraud refer to “documented criminal cases,” Krepich said, providing a link to in which California residents were convicted of using the identities of foreign nationals to steal almost $16 million from Medicare.
It’s unclear what cases Oz was referring to when he spoke of the Russian and Armenian mafia.
Ciaran McEvoy, a spokesperson for the U.S. attorney’s office for the Central District of California, which includes Los Angeles County, said it doesn’t track whether hospice fraud defendants are alleged to be foreign nationals, but he pointed to the office’s online prosecution announcements. None alleged involvement by foreign influences or organized crime.
The state audit references by the U.S. Justice Department under President Barack Obama that an “Armenian-American organized crime enterprise” was behind a nationwide health care scam.
Federal officials at the time described an “international organized crime enterprise” based in Los Angeles and New York but with roots in Russia and Armenia. The scheme involved billing for unneeded medical treatments, not hospice fraud.
A revealed fraud schemes in which hospice operators recruited patients who were not actually terminally ill, then paid kickbacks to doctors who falsely certified these patients as dying so the hospices could bill Medicare. There was no mention of foreign involvement.
бюЙѓхњДЋУНвюl Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/hospice-fraud-medicaid-mehmet-oz-cms-california/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2166080&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>


